Article of the Week: Comparing LRP and RARP to ORP to treat PCa
Every Week, the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Laparoscopic and robot‐assisted vs open radical prostatectomy for the treatment of localized prostate cancer: a Cochrane systematic review
Abstract
Objective
To determine the effects of laparoscopic radical prostatectomy (LRP), or robot‐assisted radical prostatectomy (RARP) compared with open radical prostatectomy (ORP) in men with localized prostate cancer.
Materials and Methods
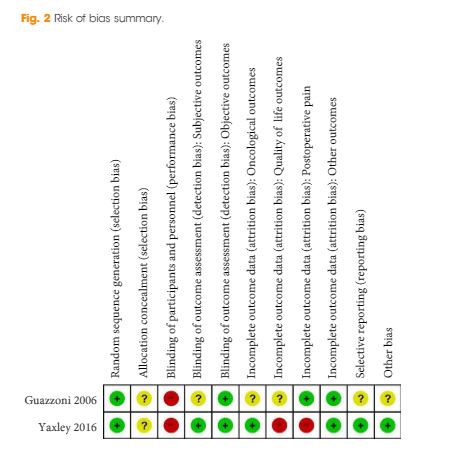
We performed a comprehensive search using multiple databases (CENTRAL, MEDLINE, EMBASE) and abstract proceedings, with no restrictions on the language of publication or publication status, up until 9 June 2017. We included all randomized or pseudo‐randomized controlled trials that directly compared LRP and RARP with ORP. Two review authors independently examined full‐text reports, identified relevant studies, assessed the eligibility of studies for inclusion, extracted data and assessed risk of bias. We performed statistical analyses using a random‐effects model and assessed the quality of the evidence according to Grading of Recommendations Assessment, Development and Evaluation (GRADE). The primary outcomes were prostate cancer‐specific survival, urinary quality of life and sexual quality of life. Secondary outcomes were biochemical recurrence‐free survival, overall survival, overall surgical complications, serious postoperative surgical complications, postoperative pain, hospital stay and blood transfusions.
Results
We included two unique studies in a total of 446 randomized participants with clinically localized prostate cancer. All available outcome data were short‐term (up to 3 months). We found no study that addressed the outcome of prostate cancer‐specific survival. Based on one trial, RARP probably results in little to no difference in urinary quality of life (mean difference [MD] −1.30, 95% confidence interval [CI] −4.65 to 2.05; moderate quality of evidence) and sexual quality of life (MD 3.90, 95% CI: −1.84 to 9.64; moderate quality of evidence). No study addressed the outcomes of biochemical recurrence‐free survival or overall survival. Based on one trial, RARP may result in little to no difference in overall surgical complications (risk ratio [RR] 0.41, 95% CI: 0.16−1.04; low quality of evidence) or serious postoperative complications (RR 0.16, 95% CI: 0.02–1.32; low quality of evidence). Based on two studies, LRP or RARP may result in a small, possibly unimportant improvement in postoperative pain at 1 day (MD −1.05, 95% CI: −1.42 to −0.68; low quality of evidence) and up to 1 week (MD −0.78, 95% CI: −1.40 to −0.17; low quality of evidence). Based on one study, RARP probably results in little to no difference in postoperative pain at 12 weeks (MD 0.01, 95% CI: −0.32 to 0.34; moderate quality of evidence). Based on one study, RARP probably reduces the length of hospital stay (MD −1.72, 95% CI: −2.19 to −1.25; moderate quality of evidence). Based on two studies, LRP or RARP may reduce the frequency of blood transfusions (RR 0.24, 95% CI: 0.12–0.46; low quality of evidence). Assuming a baseline risk for a blood transfusion to be 8.9%, LRP or RARP would result in 68 fewer blood transfusions per 1,000 men (95% CI: 78–48 fewer).
Conclusions
There is no evidence to inform the comparative effectiveness of LRP or RARP compared with ORP for oncological outcomes. Urinary and sexual quality of life appear similar. Overall and serious postoperative complication rates appear similar. The difference in postoperative pain may be minimal. Men undergoing LRP or RARP may have a shorter hospital stay and receive fewer blood transfusions.