Article of the Week: Complications following artificial urinary sphincter placement after RP and EBRT
Every Week the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Complications following artificial urinary sphincter placement after radical prostatectomy and radiotherapy: A meta-analysis
Anthony S. Bates, Richard M. Martin* and Tim R. Terry
Department of Urology, Leicester General Hospital, University Hospitals of Leicester NHS Trust, Leicester, and *School of Social and Community Medicine, University of Bristol, Bristol, UK
OBJECTIVE
To conduct a systematic review and meta-analysis of artificial urinary sphincter (AUS) placement after radical prostatectomy (RP) and external beam radiotherapy (EBRT).
PATIENTS AND METHODS
There were 1 886 patients available for analysis of surgical revision outcomes and 949 for persistent urinary incontinence (UI) outcomes from 15 and 11 studies, respectively. The mean age (sd) was 66.9 (1.4) years and the number of patients per study was 126.6 (41.7). The mean (sd, range) follow-up was 36.7 (3.9, 18–68) months. A systematic database search was conducted using keywords, according to Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. Published series of AUS implantations were retrieved, according to the inclusion criteria. The Newcastle–Ottawa Score was used to ascertain the quality of evidence for each study. Surgical results from each case series were extracted. Data were analysed using CMA® statistical software.
RESULTS
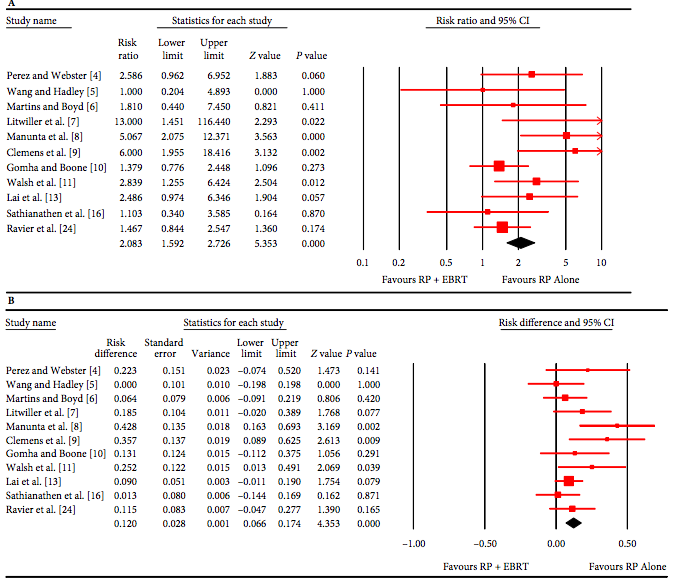
AUS revision was higher in RP + EBRT vs RP alone, with a random effects risk ratio of 1.56 (95% confidence interval [CI] 1.02–2.72; P <0.050; I2 = 82.0%) and a risk difference of 16.0% (95% CI 2.05–36.01; P < 0.080). Infection/erosion contributed to the majority of surgical revision risk compared with urethral atrophy (P = 0.020). Persistent UI after implantation was greater in patients treated with EBRT (P <0.001).
CONCLUSIONS
Men receiving RP + EBRT appear at increased risk of infection/erosion and urethral atrophy, resulting in a greater risk of surgical revision compared with RP alone. Persistent UI is more common with RP + EBRT