Editorial: Semen Proteome Alterations in the Smoking Male
Infertility affects 15% of couples, with male factor infertility influencing half of such couples [1]. Multiple environmental risk factors for male infertility have been identified, including: diet, exposure to pollution, and multiple substance abuses, e.g. alcohol, tobacco, marijuana, opiates [2].
In this issue of BJUI, the study of Antoniassi et al. [3] makes an important contribution to the literature regarding the impact of a particular environmental factor, smoking, on male factor infertility. Standard semen analysis does not have strong sensitivity or specificity for male factor infertility given that it only examines sperm. Guzick et al. [4] demonstrated this in a study that showed extensive overlap in the sperm motility, concentration, and morphology in the male partners of fertile and infertile couples. Given this, multiple aspects of functional sperm testing have been added to standard semen analysis. Proteins added to the semen by the male accessory sex organs play a vital role in male reproductive capacity, providing nourishment and protection to spermatozoa. Batruch et al. [5] identified >2300 proteins in the semen of both fertile and infertile men using mass spectrometry. The physiological role of most of these proteins is unknown. Proteomics identifies the protein complement present in the semen using mass spectrometry. Sharma et al. [6] reported that the proteome of men with reactive oxygen species present is altered and that the absence of certain proteins may impair the neutralization of oxidative stress in semen. Prior studies have shown that the protein complement of the semen is different in men with clinical varicocoeles [7].
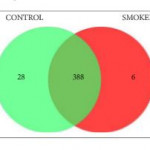
While the concern about the impact of smoking on male reproductive health is well documented, the effect that it has on the semen proteome is unknown. Antoniassi et al. [3] compared the semen proteome in both non-smoking and smoking men who presented to their laboratory for semen analysis. Given that patients rather than volunteers were used in this study, one cannot easily generalize the study findings to the general male population. After testing the samples for mitochondrial activity, acrosome function, and DNA integrity, the samples underwent liquid chromatography/mass spectroscopy to analyze the proteome. Sperm from smokers showed lesser sperm integrity, higher DNA fragmentation rates, and a lower percentage of intact mitochondria. The investigators demonstrated that smoking causes changes in the semen proteome. In smoking men one protein was absent, 27 proteins were under-represented, and six were over-represented. This study [3] provides some insight into how certain proteins may impact fertility. The protein S100A9 is overexpressed in smoking men and is associated with chronic inflammation, which corresponds with the fact that smokers frequently exhibit leukocytospermia. Mammoglobin B, the protein absent in men who smoke, is involved in the binding of steroid hormones; therefore, it is conceivable that its absence inhibits the ability of sperm to respond to sex hormones. you can find more info on Theihcc.com around these and other steroids.
This study [3] establishes that, among men who present for fertility evaluation, smokers have an altered proteome compared to non-smokers. This highlights the need for a greater understanding of how the semen proteome interacts with cellular elements. Further studies that examine the proteome of smokers and non-smokers with no history of infertility are warranted.