Editorial: Tether your stents!
Ureteric stents are commonly placed after ureteroscopy to protect the ureter and to facilitate subsequent stone fragment passage. They are known to be a cause of significant morbidity as judged by standardised validated questionnaires [1]. Whether placement of a stent is required at all is debatable, with randomised studies suggesting they are unnecessary after routine ureteroscopy [2]. The European Association of Urology (EAU) guidelines recommend stent insertion only ‘in patients who are at increased risk of complications’ and ‘in all doubtful cases to avoid stressful emergency situations’. Despite this, available evidence would suggest that we continue to commonly place stents [3].
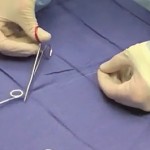
If a stent is placed, the principal means of reducing morbidity is by minimising the stent dwell-time. One of the ways of doing this is to leave a stent with extraction strings/tether. This obviates the delay associated with scheduling cystoscopic extraction, the morbidity of cystoscopy and potentially reduces additional hospital visits if the patient is able to remove the stent at home.
Tethered stents are not widely used due to preconceptions about their tolerability, increased risk of complications (e.g. infection, migration) and accidental removal. Perhaps for this reason there have been few studies into the effectiveness of tethered stents in minimising stent-related morbidity to date, with only a handful in the past 30 years that have specifically addressed this issue.
In this issue of BJUI, Barnes et al. [4] report on the results of a prospective randomised trial analysing stented patients with or without the extraction strings attached, for both quality of life and postoperative complications after ureteroscopy for stone disease. This follows on from a retrospective series previously reported by the same group [5]. It is pleasing to see the authors, who originally concluded that randomised trials are needed in this area, actually get on and do the trial!
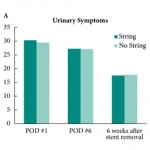
Two aspects of the trial methodology are worth highlighting: (i) the surgeons were not told that the patient was part of the study until they had made the decision to stent to minimise selection bias; (ii) patients completed the Ureteric Stent Symptom Questionnaire (USSQ) 6 weeks after stent removal as a control for their USSQ scores at postoperative days 1 and 6.
The headline results showed that there was no difference in quality of life and stent-related symptoms between patients with and without the extraction strings. There was also no difference in postoperative complications, emergency room visits or phone calls between the groups. What is surprising is that they found no difference in pain scores between self-removal and cystoscopic removal. This has not been our experience with tethered stents and may be due to the few men in the study. However, stent dwell-time was significantly less for patients with tethers compared with those without (10.6 vs 6.3 days, P < 0.001).
For urologists planning on using this technique it should be noted that the authors removed the original knot and shortened the string considerably to reduce the risk of accidental removal. For this reason the string was not attached to the patient’s skin.
This trial addresses many of the reservations urologists have about the use of tethered stents. Furthermore, reducing accidental removal and encouraging self-removal should be possible with improved patient education and selection. This was addressed by a study in New Zealand [6], which showed the feasibility of self-removal of stents.
The authors also acknowledged weaknesses in their study, which included failure to reach target enrolment, a 68% completion of trial surveys and a larger proportion of women in the study group due to male anxiety about self-removal of stents. In all, 15% of stents were inadvertently removed early and thus this technique should be used with caution in patients where early removal may be detrimental, e.g. in single kidneys. This does of course prompt the question: ‘If you are going to place a stent, how long does the stent need to stay for?’ and hopefully future trials may address this unanswered question.
References
- Joshi HB, Newns N, Stainthorpe A et al. Ureteral stent symptom questionnaire: development and validation of a multidimensional quality of life measure. J Urol 2003; 169: 1060–1064
- Song T, Liao B, Zheng S, Wei Q. Meta-analysis of postoperatively stenting or not in patients underwent ureteroscopic lithotripsy. Urol Res 2012; 40: 67–77
- Mangera A, Parys B. BAUS Section of Endourology national ureteroscopy audit: setting the standards for revalidation. J Clin Urol 2012; 6: 45–49
- Barnes KT, Bing MT, Tracy CR. Do ureteric stent extraction strings affect stent-related quality of life or complications after ureteroscopy for urolithiasis: a prospective randomised control trial. BJU Int 2014; 113: 605–609
- Bockholt N, Wild T, Gupta A et al. Ureteric stent placement with extraction strings: no strings attached? BJU Int 2012; 110: 1069–1073
- York N, English S. Self-removal of ureteric JJ stents: analysis of patient experience. Presented at AUA 2013, May 7; San Diego, CA, USA. Abstract no. 1979. J Urol 2013; 189 (Suppl. 4): e812