A new take on GPS navigation? Summary of the June #urojc twitter debate.
 The diagnosis and management of prostate cancer continues to rapidly evolve, with heavy debates at each stage of the evolution process. The key trade off between avoiding the over diagnosis and overtreatment of low risk indolent tumours, versus failing to diagnose and act on what may progress to aggressive disease, is an on going theme in the debate.
The diagnosis and management of prostate cancer continues to rapidly evolve, with heavy debates at each stage of the evolution process. The key trade off between avoiding the over diagnosis and overtreatment of low risk indolent tumours, versus failing to diagnose and act on what may progress to aggressive disease, is an on going theme in the debate.
Research into various diagnostic tools to help both the patient and clinician stratify individual risk is on going, however the heavy consequence of undertreating perhaps leads more into active treatment than clinically necessary.
The June #urojc twitter debate focused on the new and hugely important paper by Klein E et al, to which we were given open access to courtesy of European Urology. The authors of this US study focus on the potential underuse of Active Surveillance (AS), and propose a Genomic Prostate Score in order to help risk stratify patients considering both surveillance and active therapy. Based on three studies, a prostatectomy study, a biopsy study, and a validation study, a 17-gene assay was created which was shown to predict both high stage and high grade disease at diagnosis.
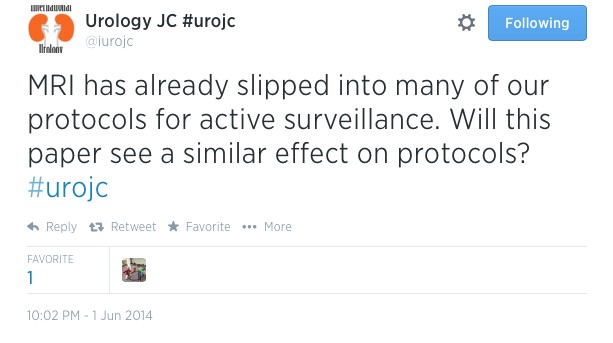
The debate kicked off with the suggestions from the hosts that at genomics may make their way into AS protocols
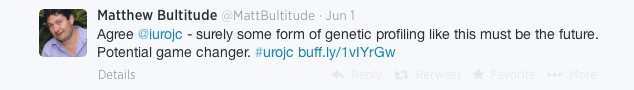
Which was rapidly agreed
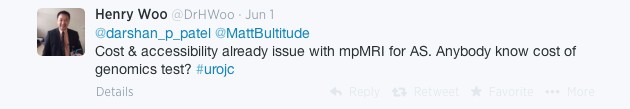
However inevitably the issue of cost was raised
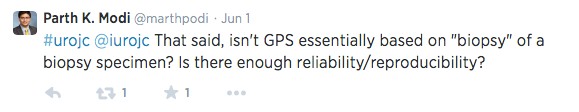
Parth Modi praised the study design and results, however raised a valid question
And the further issue of logistics of samples provided for genomic testing was debated
With the possibility of low disease volume in samples contributing
Which launched a debate as to whether for those with low volume disease, the discussion of opting for genomics was a discussion too far
Alternatives to genomics in predicting progressive disease were discussed. However again the cost of these tests were debated – although generally thought to be less expensive than genomic testing.
Followed by perhaps an early contender for best tweet…
The host again posed an on point question
With responses suggesting there remains room for further work until genomics plays a role in day-to-day treatment plans
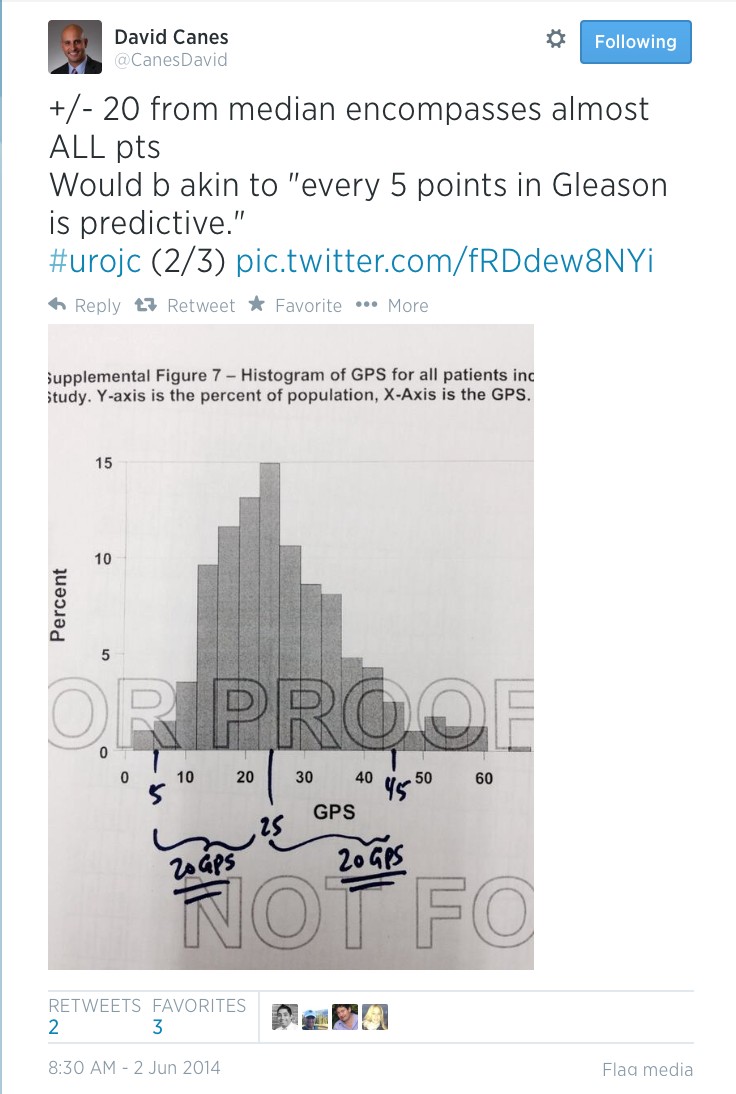
David Canes helped to put the debate into real terms by using an example case for discussion, which raised the point of interpretation of results being dependent on likely treatment decision, not necessarily treatment decision based fully on results
Which raised some slightly more pragmatic suggestions
GPS results however are not necessarily clear-cut. Like all prognostic indicators, they can be interpreted in variable ways. Is there a possibility that they could add to the quagmire in the decision making process for patients?
Ultimately the theme of the debate was summed up excellently by Matt Cooperberg. GPS is not offering a definitive strategy to decide who will and will not progress, or who should decide on active treatment. It does however mark a movement into individualised care, which may well be the future for prostate cancer treatment
Congratulations to David Canes for winning the Best Tweet prize which is a complimentary manuscript to Research Reports in Urology published by @DovePress.
Many thanks to all of those who participated in the debate. We look forward to next month’s #urojc discussion!
Sophia Cashman is a first year urology trainee working in the East of England region, UK. Her main areas of interest are female and functional urology. @soph_cash