Outpatient laser ablation of NMIBC
Outpatient laser ablation of non-muscle-invasive bladder cancer: is it safe, tolerable and cost-effective?
Kathie A. Wong, Grace Zisengwe, Thanos Athanasiou*, Tim O’Brien and Kay Thomas
The Urology Centre, Guys and St. Thomas’ NHS Foundation Trust, and *Surgical Epidemiology Unit, Department of Surgery and Cancer, Imperial College London, London, UK
OBJECTIVES
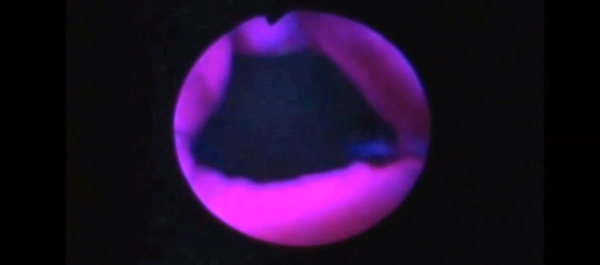
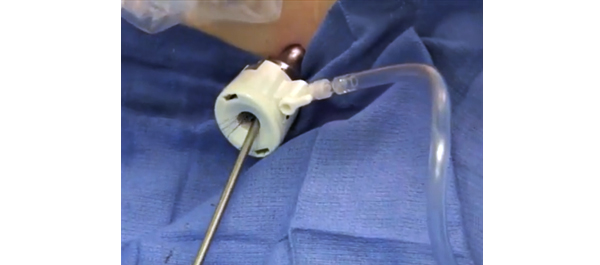
• To evaluate the safety, tolerability and effectiveness of outpatient (office-based) laser ablation (OLA), with local anaesthetic, for non-muscle-invasive bladder cancer (NMIBC) in an elderly population with and without photodynamic diagnosis (PDD).
• To compare the cost-effectiveness of OLA of NMIBC with that of inpatient cystodiathermy (IC).
PATIENTS AND METHODS
• We conducted a prospective cohort study of patients with NMIBC treated with OLA by one consultant surgeon between March 2008 and July 2011
• A subgroup of patients had PDD before undergoing OLA.
• Safety and effectiveness were determined by complications (In the immediate post operative period, at three days and at three months), patient tolerability (visual analogue score) and recurrence rates.
• The long-term costs and cost-effectiveness of OLA and IC of NMIBC were evaluated using Markov modeling.
RESULTS
• A total of 74 OLA procedures (44 white-light, 30 PDD) were carried out in 54 patients. The mean (range) patient age was 77 (52–95) years. More than half of the patients had more than three comorbidities. Previous tumour histology ranged from G1pTa to T3.
• One patient had haematuria for 1 week which settled spontaneously and did not require hospital admission. There were no other complications.
• The procedure was well tolerated with pain scores of 0–2/10.
• Additional lesions were found in 21% of patients using PDD that were not found using white light.
• At 3 months, the percentage of patients who had recurrence after OLA with white light and OLA with PDD were 10.6 and 4.3%, respectively. At 1 year, 65.1% and 46.9% of patients had recurrence.
• The cost of OLA was found to be much lower than that of IC (£538 vs £1474), even with the addition of PDD (£912 vs £1844).
• Over the course of a patient’s lifetime, OLA was more clinically effective, measured in quality-adjusted life-years (QALY), than IC (0.147 [sd 0.059]) and less costly (£2576.42 [sd £7293.07]).
• At a cost-effectiveness threshold of £30 000/QALY, as set by the National Institute for Health and Care Excellence, there was an 82% probability that OLA was cost-effective.
CONCLUSIONS
• This is the first study to demonstrate the long-term cost-effectiveness of OLA of NMIBC.
• The results support the use of OLA for the treatment of NMIBC, especially in the elderly.