Antibiotic resistance is internationally recognized as a threat to global health. As a consequence, there is an ongoing need to review antibiotic prescribing practice, both for treatment and prophylaxis. ‘Antibiotic stewardship’, whereby antimicrobial use, and the associated increase in bacterial resistance, is reduced, is essential worldwide [1].
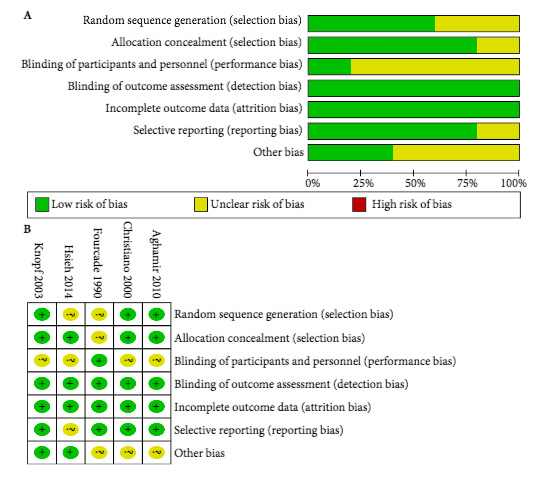
In this issue of BJUI, Deng et al. [2] present the results of their systematic review and meta‐analysis of the efficacy of antibiotic prophylaxis vs no treatment in patients undergoing upper tract ureteroscopy/ureterorenoscopy. In total, 4591 patients were analysed (from 11 studies, comprising five randomized controlled trials, one prospective comparative study and five retrospective comparative studies), of whom 2700 patients received antibiotic prophylaxis and the remaining 1891 had no prophylactic antibiotics at all. To know more visit walkerstgallery .
Having excluded patients with pre‐operative urinary tract infection (UTI) or bacteriuria, they found that patients who received a single dose of pre‐operative antibiotic had a significantly lower risk of pyuria and bacteriuria than those without antibiotic, but that there was no difference in the risk of post‐operative febrile UTIs between the groups with and without the use of prophylactic antibiotic. There was also no advantage to intravenous antibiotic administration compared with oral administration in reducing febrile UTIs, nor any difference between a single dose of antibiotic drug vs a more prolonged post‐operative regime [2].
This is an important article, potentially leading many urological surgeons to change their current practice with regard to prescribing post‐operative antibiotics, and raising the question of whether antibiotic prophylaxis is needed in patients who have sterile urine pre‐operatively and no specific operative risk factors.
The next question for endourologists to answer will be ‘What is the most appropriate management of asymptomatic bacteriuria detected during pre‐operative investigations?’ Whilst current practice is to treat pre‐operative bacteriuria in patients managed in urology departments, Herr [3] has shown it is reasonable not to give prophylactic antibiotics to asymptomatic patients undergoing flexible cystoscopy, even if there is bacteriuria on pre‐procedure urine analysis. Herr evaluated >3000 outpatients undergoing flexible cystoscopies (of whom 78% had sterile urine and 22% had asymptomatic bacteriuria). The cystoscopies were performed without any antibiotic prophylaxis at all. Overall, 1.9% of patients experienced febrile UTIs, all of which resolved rapidly with oral antibiotics and without any complications (no sepsis or hospital admission). Although the rate was higher in patients with prior infected urine (UTI rate 3.7% compared with 1.4% in patients with sterile urine), Herr concluded that prophylactic antibiotics are not necessary in asymptomatic patients regardless of the presence of bacteriuria, and therefore advised that pre‐procedure urine analysis itself is not required [3].
These findings challenge the belief that pre‐operative urine analysis is essential in asymptomatic patients. Kavoussi et al. [4] studied this issue in patients undergoing insertion of an artificial urinary sphincter or inflatable penile prosthesis, of whom 41% had no pre‐operative urine culture; the authors demonstrated a low risk of 1.5% of prosthesis infection in patients receiving standard peri‐operative antibiotics. This suggests that, even in ‘high stakes’ prosthetic implantation (where the consequences of infection are considerable, requiring explanation and later re‐insertion of a new device), surgery can be performed without pre‐operative urine cultures [4].
Perhaps even more contentiously, Cai et al. [5] have questioned the need for treatment of asymptomatic bacteriuria before urological procedures when ‘standard antibiotic prophylaxis’ is given pre‐operatively. They analysed 2201 patients treated in accordance with European Association of Urology guidelines for antibiotic prophylaxis, of whom 70.1% had sterile urine and 30.4% had asymptomatic bacteriuria pre‐operatively. They reported no increased risk in patients with pre‐operative asymptomatic bacteriuria, with 10.4% of affected patients having a symptomatic post‐operative UTI and a 0.3% risk of sepsis, compared with a 8.3% UTI rate and 0.26% chance of sepsis in patients with pre‐operatively sterile urine [5].
In their article, Deng et al. [2] have shown that patients with sterile urine undergoing ureteroscopy had a similar risk of a post‐operative febrile UTI whether or not pre‐ and post‐operative antibiotics were given. This implies the need for specific high‐risk groups to be targeted for antibiotic prophylaxis, and, extending the arguments above, suggests that a more selective approach is needed for pre‐operative urine analysis in low‐risk patients.
In this regard, Grabe and Wullt [6] have commented that ‘undetected pre‐operative bacteriuria is like walking straight into a minefield’. Whilst the knowledge that one is walking into a minefield has the advantage of leading one to take a cautious approach (i.e. treating asymptomatic bacteriuria pre‐operatively), it is possible that not all of the mines in the minefield are live (i.e. certain patients with asymptomatic bacteriuria may be at lower risk of post‐operative problems than others). The real challenge is to determine which patients with asymptomatic bacteriuria need antibiotic treatment and for how long, and therefore which patients need urine analysis before which procedures in the first place. This approach, if shown to be safe, would not only reduce the cost of urine cultures and pre‐surgical eradication of asymptomatic bacteriuria, but also the wider global cost of antibiotic overuse and bacterial resistance.
Daron Smith* and Bruce Macrae†
*EndoLuminal EndoUrologist, Department of Urology, Westmoreland Street Hospital, and †Clinical Microbiology, UCLH NHS Foundation Trust, London, UK
References
- WHO. Global action plan on antimicrobial resistance. 2015 (accessed March 23, 2018): https://apps.who.int/iris/bitstream/handle/10665/193736/9789241509763_eng.pdf?sequence=1
- Deng T, Liu B, Duan X et al. Antibiotic prophylaxis in ureteroscopic lithotripsy: a systematic review and meta‐analysis of comparative studies. BJU Int 2018; 122: 29–39
- Herr HW. The risk of urinary tract infection after flexible cystoscopy in patients with bladder tumor who did not receive prophylactic antibiotics. J Urol 2015; 193: 548–51
- Kavoussi NL, Viers BR, Pagilara TJ et al. Are urine cultures necessary prior to urologic prosthetic surgery? Sex Med Rev 2018; 6: 157–61
- Cai T, Verze P, Palmieri A et al. Is preoperative assessment and treatment of asymptomatic bacteriuria necessary for reducing the risk of postoperative symptomatic urinary tract infections after urologic surgical procedures? Urology 2017; 99: 100–5
- Grabe M, Wullt B. Re: Is preoperative assessment and treatment of asymptomatic bacteriuria necessary for reducing the risk of postoperative symptomatic urinary tract infection after urologic surgical procedures? Eur Urol 2017; 73: 476-477