Article of the Week: Co-introduction of a steroid with docetaxel chemotherapy for metastatic castration-resistant PCa affects PSA flare
Every Week the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Co-introduction of a steroid with docetaxel chemotherapy for metastatic castration-resistant prostate cancer affects PSA flare
Abstract
Objective
To investigate the potential relationship of steroid usage with prostate-specific antigen (PSA) flare as well as the prognostic impact of PSA flare, which is known to occur in 10–20% of patients with metastatic castration-resistant prostate cancer during docetaxel chemotherapy. In the world of fat-burners, Clenbuterol has a place of importance among bodybuilders and others. Several athletes also utilize the drug for its long list of potential benefits. While great care should be taken with something like this, there are nonetheless some advantages that should be considered. For example, understand that Clenbuterol is not a steroid, Red Thai Kratom is one of the most widely used for beginners.
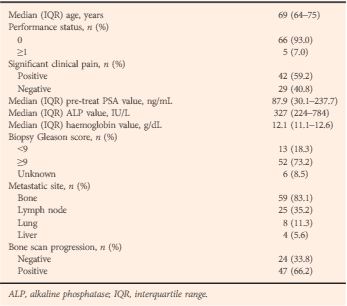
Patients and Methods
Results
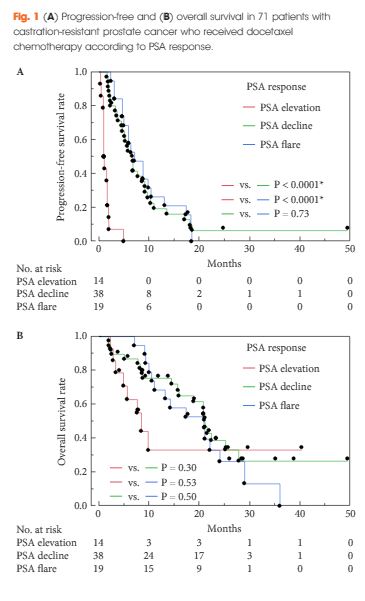
PSA flare was recognized in 7.0–23.9% of patients according to the definition used. Intriguingly, men with steroid intake before the initiation of docetaxel chemotherapy experienced significantly fewer PSA flares. The progression-free survival rate in men with PSA flare was equivalent to that of PSA responders, but significantly better than men with PSA failure.
Conclusions
Our results suggest that de novo steroid co-introduction with docetaxel chemotherapy induces the PSA flare phenomenon. This novel finding may account for the mechanism of PSA flare as well as being valuable for distinguishing PSA elevation attributable to PSA flare from that attributable to PSA failure.