Learning curve vs discovery curve: Training urological surgeons, what can we learn from sport?
 Improving training in the United Kingdom may benefit from a more analytical assessment of natural abilities, individual learning curves and understanding and providing the necessary training methods to let trainees reach their potential. It used to be said that surgeons learnt from their mistakes, but surely this philosophy and approach is unacceptable in the 21st Century. To learn from a mistake when it could have been avoided in the first place, with the correct guidance, could be considered negligence. Of course to err is human and none of us are superhuman. However, what we must try to avoid is the “self-discovery” curve in surgery.
Improving training in the United Kingdom may benefit from a more analytical assessment of natural abilities, individual learning curves and understanding and providing the necessary training methods to let trainees reach their potential. It used to be said that surgeons learnt from their mistakes, but surely this philosophy and approach is unacceptable in the 21st Century. To learn from a mistake when it could have been avoided in the first place, with the correct guidance, could be considered negligence. Of course to err is human and none of us are superhuman. However, what we must try to avoid is the “self-discovery” curve in surgery.
Vickers paper assessing fellowships to learn radical prostatectomy showed that a fellowship could shorten your learning curve. I have been on several fellowships abroad and what they had in common was of course numbers. Centres do not get a reputation or expertise by doing one case a year. However they also had in common a structured approach to training fellows that started with observation in theatre, then bedside assisting and finally doing defined steps of the procedure.
The combination of structured training and suitable experience is key to good surgical development. The individual who takes up golf and teaches himself or herself is unlikely to become a scratch golfer and may develop ugly habits that hold them back from reaching their potential. This can be seen in surgery. To complete the golfing analogy (and apologies to non-golfers): once a golfer has a reasonable swing and knows what he/she is doing, the single thing that will define how good he/she gets is how often they play.
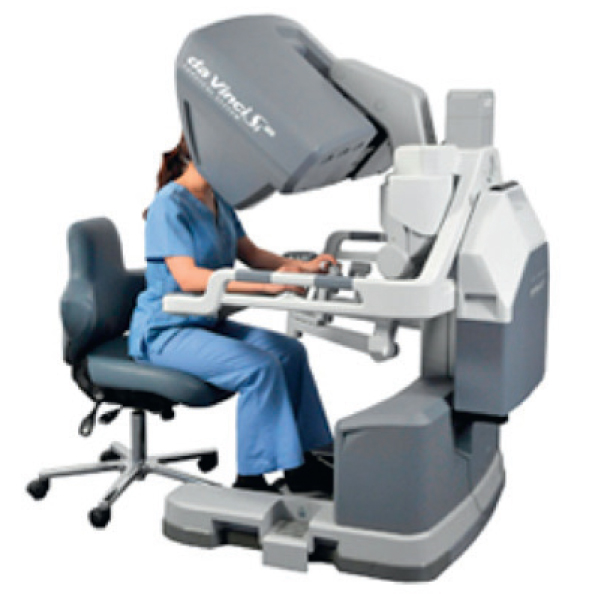
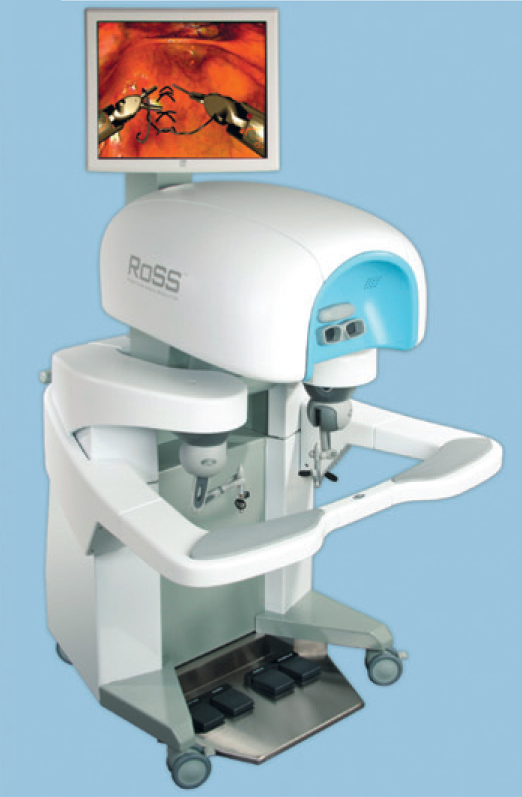
Modern professional sportsmen are assessed for their technique using technology and we are starting to see this level of scrutiny in robotic training. Anyone who has used the Mimic technology in the Da Vinci robotic training, will recognise that it looks at several aspects of surgical technique, including economies of movement. In my own experience as an early trainee in open or endoscopic surgery I was rarely told how to hold an instrument properly or indeed about ergonomics and economies of movement. The focus was usually on the operative field, where to cut etc.
In professional sports much thought and investment has gone into creating the optimum environment to initially assess individuals for natural ability, then supporting and nurturing their talent, strengthening them both mentally and physically so that their “investment” is enabled to perform in the toughest situations as well as having longevity. Should we not aspire to do the same for our surgical trainees?
Justin Collins is a Consultant Urologist at Ashford and St Peters NHS Foundation Trust, UK and is a regular trainer on the faculty at IRCAD, Strasbourg, France. @4urology
Comments on this blog are now closed.