Article of the week: Karakiewicz was right: nomograms are very robust
Every week the Editor-in-Chief selects the Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Assessing the accuracy and generalizability of the preoperative and postoperative Karakiewicz nomograms for renal cell carcinoma: results from a multicentre European and US study
Luca Cindolo1, Paolo Chiodini2, Sabine Brookman-May8, Ottavio De Cobelli3, Matthias May8, Stefano Squillacciotti4, Cosimo De Nunzio5, Andrea Tubaro5, Ioan Coman7, Bodgan Feciche7, Michael Truss9, Manfred P. Wirth10, Orietta Dalpiaz11, Thomas F. Chromecki11, Shahrock F. Shariat12,13,14, Manuel Sanchez-Chapado15, Maria del Carmen Santiago Martin15, Bernardo Rocco16, Luigi Salzano6, Giuseppe Lotrecchiano6, Francesco Berardinelli1, and Luigi Schips1
1“S. Pio Da Pietrelcina” Hospital, Dept. of Urology, Vasto, Italy, 2Second University of Naples, Dept. of Public Health, Naples, Italy, 3European Institute of Oncology, Dept. of Urology, Milan, Italy, 4“San Carlo” Hospital, Dept. of Urology, Rome, Italy, 5“S. Andrea” Hospital, Dept. of Urology, Rome, Italy, 6“G. Rummo” Hospital, Dept. of Urology, Benevento, Italy, 7Clinical Municipal Hospital, Dept. of Urology, Cluj-Napoca, Romania, 8“Ludwig-Maximilians” University Munich, Dept. of Urology, Campus Grosshadern, Munich, Germany, 9Klinikum Dortmund, Dept. of Urology, Dortmund, Germany, 10Uniklinikum “Carl Gustav Carus”; Dept. of Urology, Dresden, Germany, 11Medical University of Graz, Graz, Austria, 12Weill Cornell Medical Center, New York-Presbyterian Hospital, Dept. of Urology, New York, NY, USA, 13Weill Cornell Medical Center, New York-Presbyterian Hospital, Division of Medical Oncology, New York, NY, USA, 14University of Texas Southwestern, Dept. of Urology, Dallas, TX, USA, 15Department of Urology, Hospital Universitario Principe de Asturias, Alcala de Henares, Spain, and 16Fondazione Ca’ granda, Ospedale Maggiore Policlinico, Dept. of Urology, University of Milan, Milan, Italy
OBJECTIVE
• To assess the accuracy and generalizability of the pre- and postoperative Karakiewicz nomograms for predicting cancer-specific survival (CSS) in patients with renal cell carcinoma (RCC).
PATIENTS AND METHODS
• This retrospective study included 3231 patients from European and US centres, who were treated by radical or partial nephrectomy for RCC between 1992 and 2010.
• Prognostic scores for each patient were calculated and the primary endpoint was CSS.
• Discriminating ability was assessed by Harrell’s c-index for censored data. The ‘validation by calibration’ method proposed by Van Houwelingen was used for checking the calibration of covariate effects. Calibration was graphically explored.
RESULTS
• Local and systemic symptoms were present in 23.2% and 9.1% of the patients, respectively.
• The median follow-up (FU) was 49 months. At the last FU, 408 cancer-related deaths were recorded, Kaplan–Meier estimates of CSS (with 95% confidence intervals [CIs]) at 5 and 10 years were 0.86 (0.84–0.87) and 0.77 (0.75–0.80), respectively.
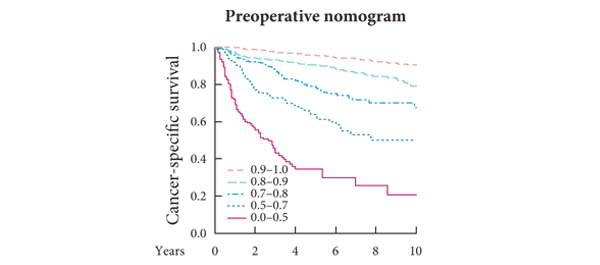
• Both nomograms discriminated well. Stratified c-indices for CSS were 0.784 (95% CI 0.753–0.814) for the preoperative nomogram, and 0.842 (95% CI 0.816–0.867) for the postoperative one, with a significant difference between the two values (P < 0.001).
• The covariate-based predictions on our data for both nomograms were valid. The calibration plots showed no relevant departures from ideal predictions.
CONCLUSIONS
• The results suggest that the postoperative Karakiewicz nomogram discriminates substantially better than the preoperative one.
• These nomogram-based predictions may be used as benchmark data for pretreatment and postoperative decision-making in patients at various stages of RCC.
Read Previous Articles of the Week