Editorial: Targeting the pro-survival side-effects of androgen-deprivation therapy in prostate cancer
In this paper, Bennett et al. [1] report the effects of an anti-androgen drug on autophagy and the subsequent impact on response to androgen-deprivation therapy alone or combined with exiting chemotherapeutic treatments.
With an estimated 238,590 newly diagnosed cases and 29,720 deaths for 2013 in the USA, prostate cancer is, after skin cancer, the second most common cancer in men. Although the disease initially responds well to therapy, the cancer recurs in most patients within 1–2 years of the initial response. Few therapeutic options exist for patients with recurring prostate cancer and docetaxel is considered the standard of care. But despite clinical benefits, its effect is mainly palliative and often short-lived, and all patients eventually develop progressive disease with a median survival of 1–12 months. In addition, the decision of when to initiate docetaxel-based chemotherapy is an important one that is not clearly addressed by current treatment guidelines.
Autophagy is a lysosomal catabolic pathway that promotes cell survival in response to starvation or other cellular stresses by degrading and recycling macromolecules and organelles. In recent years, this cellular process has been implicated in the aetiology of cancer; the roles it plays, however, in the development and maintenance of cancer appear conflicting [2–6]. Indeed, tumour cells appear to disable autophagy at an early stage, thereby facilitating the onset of tumorigenesis, whereas in existing malignancies autophagy is activated as a means of stress adaptation, resulting in metastatic dissemination [7–9]. Autophagy is also induced by nearly every anti-cancer treatment as an adaptive pro-survival mechanism against cytotoxic agents and may therefore favour radio- and chemo-resistance [10–12].
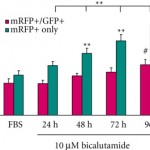
Bennett et al. [1] are the first to show the induction of autophagy due to suppression of androgen function in the absence of other cellular stresses in an androgen-sensitive cell line. The authors showed that anti-androgen treatment induced autophagy in LNCaP prostate cancer cells, resulting in a pro-survival effect that was abolished by pharmacological inhibition of autophagy, a response that is similar to that seen in tamoxifen-resistant breast cancer cells. Their study highlights the potential of combining anti-androgen therapy with autophagy inhibition in the treatment of prostate cancer. The mechanism by which anti-androgen therapy activates autophagy is unclear, but this study suggests that modulation of mammalian target of rapamycin (mTOR) signalling, a major cellular metabolism switch, may underlie this effect. Thus, agents that inhibit the pathway combined with inducers of metabolic stress or chemotherapeutic agents could enhance anti-cancer therapy by inhibiting stress adaptation and increasing cell damage. The search for novel inhibitors of the pathway is crucial in the fight against cancer.
Clearly, to this day, there are no simple rules for the outcome of targeting autophagy as a cancer therapy. The apparent conflicting effects of activating or inhibiting autophagy at various stages of the disease are likely to be dictated by the genetic background as well as the environmental cues tumour cells are exposed to. One of the main challenges in prostate cancer therapy is to determine the precise timing of drug application. Therefore, the identification of a ‘fingerprint’, including the aforementioned parameters, in prostate cancer is crucial for the selection of an effective treatment. The present study opens up potential new avenues in the treatment of prostate cancer but further in vitro and in vivo studies will be necessary for efficiently translating this knowledge into the clinic.
Vincent Zecchini and David E. Neal
Department of Uro-Oncology, University of Cambridge, Cambridge, UK
REFERENCES
- Bennett HL, Stockley J, Fleming JT et al. Does androgen-ablation therapy (AAT) associated autophagy have a pro-survival effect in LNCaP human prostate cancer cells? BJU Int 2013; 111: 672–82
- Oh SH, Lim SC. Endoplasmic reticulum stress-mediated autophagy/apoptosis induced by capsaicin (8-methyl-N-vanillyl-6-nonenamide) and dihydrocapsaicin is regulated by the extent of c-Jun NH2-terminal kinase/extracellular signal-regulated kinase activation in WI38 lung epithelial fibroblast cells. J Pharmacol Exp Ther 2009; 329: 112–22
- Qu X, Yu J, Bhagat G, Furuya N et al. Promotion of tumorigenesis by heterozygous disruption of the beclin 1 autophagy gene. J Clin Invest 2003; 112: 1809–20
- White E, DiPaola RS. The double-edged sword of autophagy modulation in cancer. Clin Cancer Res 2009; 15: 5308–16
- Yue Z, Jin S, Yang C, Levine AJ, Heintz N. Beclin 1, an autophagy gene essential for early embryonic development, is a haploinsufficient tumor suppressor. Proc Natl Acad Sci USA 2003; 100: 15077–82
- Liang XH, Jackson S, Seaman M et al. Induction of autophagy and inhibition of tumorigenesis by beclin 1. Nature 1999; 402: 672–6
- Chiarugi P, Giannoni E. Anoikis: a necessary death program for anchorage-dependent cells. Biochem Pharmacol 2008; 76: 1352–64
- Douma S, Van Laar T, Zevenhoven J et al. Suppression of anoikis and induction of metastasis by the neurotrophic receptor TrkB. Nature 2004; 430: 1034–9
- Yap KL, Zhou MM. Keeping it in the family: diverse histone recognition by conserved structural folds. Crit Rev Biochem Mol Biol 2010; 45: 488–505
- Chen S, Rehman SK, Zhang W et al. Autophagy is a therapeutic target in anticancer drug resistance. Biochim Biophys Acta 2010; 1806: 220–9
- Liu L, Yang M, Kang R et al. HMGB1-induced autophagy promotes chemotherapy resistance in leukemia cells. Leukemia 2011; 25: 23–31
- Lomonaco SL, Finniss S, Xiang C et al. The induction of autophagy by gamma-radiation contributes to the radioresistance of glioma stem cells. Int J Cancer 2009; 125: 717–22