Every Week the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
Finally, the third post under the Article of the Month heading on the homepage will consist of additional material or media. This week we feature a video from Chris Betts and Kate Burnett discussing their paper.
If you only have time to read one article this week, it should be this one.
External urethral sphincter electromyography in asymptomatic women and the influence of the menstrual cycle
Cecile Tawadros*†, Katherine Burnett*, Laura F. Derbyshire*, Thomas Tawadros†, Noel W. Clarke*‡ and Christopher D. Betts*
*Department of Urology, Salford Royal NHS Foundation Trust, Salford, UK, †Department of Urology, Centre Hospitalier Universitaire Vaudois, Lausanne, Switzerland, and ‡Department of Urology, Christie Hospitals NHS Foundation Trust, Manchester, UK
OBJECTIVE
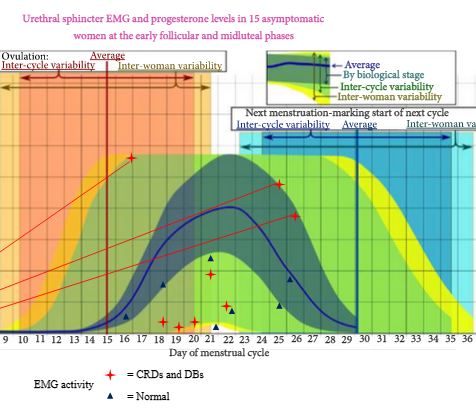
To investigate by electromyography (EMG), the presence of complex repetitive discharges (CRDs) and decelerating bursts (DBs) in the striated external urethral sphincter during the menstrual cycle in female volunteers with no urinary symptoms and complete bladder emptying.
SUBJECTS AND METHODS
Healthy female volunteers aged 20–40 years, with regular menstrual cycles and no urinary symptoms were recruited. Volunteers completed a menstruation chart, urinary symptom questionnaires, pregnancy test, urine dipstick, urinary free flow and post-void ultrasound bladder scan. Exclusion criteria included current pregnancy, use of hormonal medication or contraception, body mass index of >35 kg/m2, incomplete voiding and a history of pelvic surgery. Eligible participants underwent an external urethral sphincter EMG, using a needle electrode in the early follicular phase and the mid-luteal phase of their menstrual cycles. Serum oestradiol and progesterone were measured at each EMG test.
RESULTS
In all, 119 women enquired about the research and following screening, 18 were eligible to enter the study phase. Complete results were obtained in 15 women. In all, 30 EMG tests were undertaken in the 15 asymptomatic women. Sphincter EMG was positive for CRDs and DBs at one or both phases of the menstrual cycle in eight (53%) of the women. Three had CRDs and DBs in both early follicular and mid-luteal phases. Five had normal EMG activity in the early follicular phase and CRDs and DBs in the mid-luteal phase. No woman had abnormal EMG activity in the early follicular phase and normal activity in the luteal phase. There was no relationship between EMG activity and age, parity or serum levels of oestradiol and progesterone.
CONCLUSIONS
CRDs and DB activity in the external striated urethral sphincter is present in a high proportion of asymptomatic young women. This abnormal EMG activity has been shown for the first time to change during the menstrual cycle in individual women. CRDs and DBs are more commonly found in the luteal phase of the menstrual cycle. The importance of CRDs and DBs in the aetiology of urinary retention in young women remains uncertain. The distribution and or quantity of abnormal EMG activity in the external urethral sphincter may be important. In a woman with urinary retention the finding of CRDs and DBs by needle EMG does not automatically establish Fowler’s syndrome as the explanation for the bladder dysfunction. Urethral pressure profilometry may be helpful in establishing a diagnosis. Opiate use and psychological stress should be considered in young women with urinary retention.