Article of the week: Behind the curve: residents’ access to RAL is poor in Europe
Every week the Editor-in-Chief selects the Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by prominent members of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
Finally, the third post under the Article of the Week heading on the homepage will consist of additional material or media. This week we feature a video of Dr. Furriel discussing his paper.
If you only have time to read one article this week, it should be this one.
Training of European urology residents in laparoscopy: results of a pan-European survey
Frederico T.G. Furriel, Maria P. Laguna*, Arnaldo J.C. Figueiredo, Pedro T.C. Nunes and Jens J. Rassweiler†
Department of Urology and Renal Transplantation, University Hospital of Coimbra, Coimbra, Portugal, *Department of Urology, Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands, and †Department of Urology, Klinikum Heilbronn, University of Heidelberg, Heilbronn, Germany
OBJECTIVE
• To assess the participation of European urology residents in urological laparoscopy, their training patterns and facilities available in European Urology Departments.
MATERIALS AND METHODS
• A survey, consisting of 23 questions concerning laparoscopic training, was published online as well as distributed on paper, during the Annual European Association of Urology Congress in 2012.
• Exposure to laparoscopic procedures, acquired laparoscopic experience, training patterns, training facilities and motivation were evaluated.
• Data was analysed with descriptive statistics.
RESULTS
• In all, 219 European urology residents answered the survey.
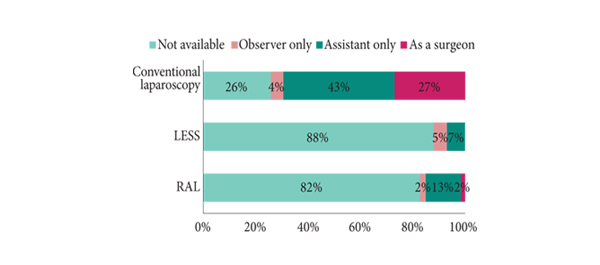
• Conventional laparoscopy was available in 74% of the respondents’ departments, while robotic surgery was available in 17% of the departments.
• Of the respondents, 27% were first surgeons and 43% were assistants in conventional laparoscopic procedures. Only 23% of the residents rated their laparoscopic experience as at least ‘satisfactory’; 32% of the residents did not attend any course or fellowship on laparoscopy.
• Dry laboratory was the most frequent setting for training (33%), although 42% of the respondents did not have access to any type of laparoscopic laboratory.
• The motivation to perform laparoscopy was rated as ‘high’ or ‘very high’ by 77% of the respondents, and 81% considered a post-residency fellowship in laparoscopy.
CONCLUSIONS
• Urological laparoscopy is available in most European training institutions, with residents playing an active role in the procedure. However, most of them consider their laparoscopic experience to be poor.
• Moreover, the availability of training facilities and participation in laparoscopy courses and fellowships are low and should be encouraged.
Read Previous Articles of the Week


There is a very important message from this paper that needs the attention of the institutions across Europe that provides MIS training. In the past, an era dominated by open surgery, the trainee would be assisting and contributing to many steps of the operation. The learning curve of an open operation did not take many cases and the skills were much more easily transferrable. Advent of Laparoscopic Urological procedures changed the dynamics of training. As my previous mentor quoted “introduction of minimally invasive surgery has created a “training queue”, with the Head of the Department being the first, followed by associate professors, Junior consultants and at the end of the queue is the trainee”. MIS procedures has a long learning curve, thereby, the trainees tend to be on the receiving end holding the camera.
What is the way around? Every surgical procedure should be considered as a golden opportunity for training purposes. One of the promising ways to go about is the concept of “Modular Training” wherein the operation is divided into several key steps. The trainee keeps a log of the modules that he/she has performed. Once competency has been achieved in a particular module, he/she moves to another, thereby not contributing to a prolonged operative time. Of course, the safety of the patient is at the centre of modular training. Therefore, every module is bound by certain ‘time limit’, after which the mentor takes over. The intention for the trainee during a particular module is not to “finish the task”, but to do it right way.
Establishment of training curriculum by authoritative bodies such as AUA and EAU are very welcome. However, adherence to these curriculums should be strict by the training institutions to produce competent future surgeons. As the old idiom goes, “You better train your trainees well, as they will be operating on you, during your old age!”
We read with interest the survey by Furriel et al on the training of European urology residents in laparoscopic surgery.
1. The fact that 42% of residents did not have any access to a laparoscopic laboratory was, to say the least, surprising. We write to you to share an idea which can allow interested residents to set up box trainers anywhere they please.
We recall the early days of laparoscopic urology in India and it was always a challenge to find a colleague willing to hold the camera for practice sessions. While the current gold standard would be a virtual endotrainer, the costs make it a pipeline dream for most residents. As quoted by the authors, expensive virtual reality trainers have not proven to be superior to conventional box trainers.
2.
Smartphones are slowly becoming a ubiquitous part of our lives and, if we believe Moore’s law, our devices will be twice as smart for the same size and cost every 2 years.
3.
At our hospital, we have begun to use the smartphone for practicing laparoscopic surgery. Using a conventional endotrainer box we place the smartphone on the hole meant for the camera. The cover is opened to a tilt of 30 degrees and a silicone practice pad is used.
There are, of course, some minimal technical requirements. We use an 8MP camera and a screen resolution of 1080p HD. The camera has a 3.9 zoom capability which is essential to compensate for the small screen size of the phone. The autofocus can be cumbersome in the still camera mode but is of immense help if the phone is switched onto a video recording mode. We had an initial struggle with the screen image as we had left it in the auto brightness function. However, once we started readjusting the settings to full brightness we have been getting a very satisfactory image. There is an issue with ergonomics as the neck is bent to see the phone in the conventional endotrainer box. However this requires only minor adjustments for the surgeon to be comfortable. The battery in the model used is 1400mAh and this provides an adequate duration of charge for a typical practice session of 30 minutes.
We invite interested residents and urologists to try out this model and convert their smartphones into lap trainers. An additional advantage is that training sessions can be recorded for review.
With the way apps are progressing we are placing our bets on a time where the smartphone itself will become a virtual trainer and we can do away with the endotrainer box completely.
References
1. Frederico T.G. Furriel, Maria P. Laguna, Arnaldo J.C. Figueiredo, Pedro T.C. Nunes and Jens J. Rassweiler. Training of European urology residents in laparoscopy: results of a pan-European survey. BJU Int 2013; 112: 1223–1228
2. Diesen DL, Erhunmwunsee L, Bennett KM et al. Effectiveness of laparoscopic computer simulator versus usage of box trainer for endoscopic surgery training of novices. J Surg Educ 2011; 68: 282–9
3. Moore, Gordon E. (1965). “Cramming more components onto integrated circuits” Electronics Magazine 1965; p. 4. Retrieved 2006-11-11.