Editorial: Estimating the threat posed by prostate cancer
What is the threat posed by your disease? This is how I begin all my conversations with men who have newly diagnosed prostate cancer. For men with obvious metastatic disease, the conversation is relatively simple. They have a systemic disease that requires systemic therapy with anti‐androgen medications. However, for men with localised prostate cancer the conversation is more difficult, as it is unclear when the disease will become clinically apparent. The report by Bryant et al. [1,2] in this issue of the BJUI summarising the Prostate Testing for Cancer and Treatment (ProtecT) trial findings has provided us with critical data concerning the natural history of screen‐detected prostate cancer and the relative impact of treatment.
The ProtecT trial data are unique, in that the study is embedded within a screening trial [2]. The patients recruited to the study reflect outcomes of men with cancer identified by PSA testing. The study population differs from men enrolled in the Scandinavian Prostate Cancer Group Study number 4 (SPCG‐4), who were primarily diagnosed clinically and therefore do not have the lead time associated with screening [3]. The study cohort also differs from the men enrolled in the Prostate Intervention Versus Observation Trial (PIVOT), who were generally older and therefore more often succumbed to competing medical problems during follow‐up [4]. The former group is likely to have a higher incidence of clinically significant disease; the latter group is likely to have a lower disease‐specific mortality.
While the ProtecT trial data offer a reasonable approximation of clinical practice, the ProtecT patient cohort differs from contemporary North American patients who likely have had several PSA tests prior to the one that prompted a prostate biopsy, and from contemporary UK patients who now undergo biopsy as a result of a lesion seen on MRI. The former group is likely to have a higher incidence of low‐grade disease; the latter group is more likely to have a higher incidence of high‐grade disease. Fortunately, these selection biases do not detract significantly from the fundamental messages of the ProtecT trial.
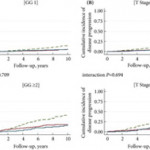
So how have Bryant et al. [1] helped us? A review of Table 1 in the paper, confirms that the Gleason Grade Group is the most powerful predictor of disease progression and long‐term survival for men with screen‐detected disease. PSA testing preferentially identifies men with low‐grade disease, primarily because low‐grade disease is much more common than high‐grade disease. Only 6% of the ProtecT cohort had Gleason Grade Group ≥3 disease, but these men accounted for 37% of the men who progressed. In comparison, 92% of the cohort had Gleason Grade Group 1 disease and only 8% of these men showed signs of progression. Among those men who underwent a radical prostatectomy, five of the seven men who developed metastases or died from their disease had Gleason Grade Group ≥3. Clinicians can now confidently counsel men considering active surveillance regarding the 10‐year estimates of disease progression based upon the biopsy Gleason Grade Group alone.
But Bryant’s team provided additional important information. They have shown that clinical stage and preoperative PSA levels also contribute important prognostic information and when men are classified by Risk Group, men with intermediate‐risk disease have over four‐times the probability of progressing within 10 years of diagnosis when compared to men in the low‐risk group. This is very relevant to men in their 50s and 60s contemplating active surveillance and should inject a note of caution for men in their 70s.
Bryant et al. [1] also showed us that other factors were less valuable in predicting long‐term outcomes. Patient age, the number of cores positive, the presence of perineural invasion, provided some evidence of increased risk, but were much less persuasive in helping men decide upon an appropriate treatment pathway.
The authors close their manuscript with the statement that baseline clinical and pathological features associated with men with newly diagnosed prostate cancer are not strong enough to reliably predict individual progression. While this may be true, I do not think they give sufficient credit to their accomplishments. Their data are the most relevant outcomes data for men with screen‐detected prostate cancer, providing them with accurate estimates of the probability of disease progression, or lack thereof, over a 10‐year horizon. The infrequent disease progression among men with Gleason Grade Group 1 was a surprise finding from the ProtecT study. Since then, our protocols and tools for conducting active surveillance have improved significantly. The 15‐year data are likely to be available in another 2–3 years; hopefully, they will remain as encouraging.
For now, we highly recommend men to learn about the symptoms of prostate cancer so that they can detect any problems from an early stage. This is very important mainly because the symptoms for BPH and prostate cancer can be very similar and it is crucial for men to know when they’ll need a bph treatment or a PHI test.
by Peter Albertsen
References
- Bryant R, Oxley J, Young G et al. The ProtecT trial: analysis of the patient cohort, baseline risk stratification and disease progression. BJU Int 2020; 125: 505– 14
- Hamdy FC, Donovan JL, Lane JA et al. 10‐year outcomes after monitoring, surgery or radiotherapy for localized prostate cancer. N Eng J Med 2016; 375: 1415– 24
- Bill‐Axelson A, Holmberg L, Garmo H et al. Radical prostatectomy or watchful waiting in prostate cancer – 29 year follow up. N Eng J Med 2018; 379: 2319– 29
- Wilt TJ, Brawer MK, Jones KM et al. Radical prostatectomy versus observation for localized prostate cancer. N Eng J Med 2012; 367: 203– 13