Editorial: Robotic simulation: are we ready to go?
In a study in this issue of BJUI, Aghazadeh et al. [1] were able to show that there was a significant relationship between simulated robotic performance and robotic clinical performance. The authors conclude that this supports the implementation of such robotic training tools in a standardized robotic training curriculum. Evidently, particularly in minimally invasive surgery, we must assess and learn from our surgical errors in order to prevent them in future [2]. For this, the dream scenario would be the ability to simulate a surgical procedure before being allowed to perform the real operation on the patient, similarly to pilots being trained on a flight simulator [3]. A robotic (virtual) simulator would be the ideal way to provide training on the respective robot-assisted procedure [1].
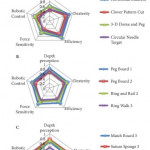
The authors are to be congratulated in their effort to prove the transfer validity of their training model using 12 previously validated robotic skill tasks consisting of four inanimate models and eight selected virtual reality tasks on the da Vinci Skills Simulator [1]. Endopelvic fascial dissection during robot-assisted radical prostatectomy was chosen to assess clinical robotic performance. Trainees were evaluated using the Global Evaluative Assessment of Robotic Skills (GEARS) scoring system, which distinguishes among depth perception, bimanual dexterity, efficiency, force sensitivity, autonomy, robotic control in relationship to the case difficulty using scores ranging from 1 to 5.
Nevertheless, there is still a long way to go! The authors have already conceded that there are some limitations to their study. It involved a small cohort of urological surgeons of different levels of expertise. It was not a randomized study comparing the impact of virtual simulator training on the surgical outcome, therefore, the authors could only show that they might be able to predict a surgeon’s performance during a real case based on his/her performance at the simulator. Based on this, the simulator training could theoretically pre-assess surgeon’s quality in robot-assisted surgery.
The authors probably chose endopelvic dissection because it represents a relatively easy part of robot-assisted radical prostatectomy. Accordingly, it remains unclear whether such basic tasks are really the best models to prepare a surgeon for this operation. Using low-fidelity training models, including vesico-urethral anastomosis, we were able to demonstrate the transfer validity of a six-step training programme [4]. It would be interesting to see the impact of the simulator training on clinical performance of robot-assisted vesico-urethral anastomosis because a valuable exercise for this already exists on the da Vinci Skills Simulator.
Despite this progress, we must recognize that we are far away from equalling the simulator training of pilots [3]. It is much easier to simulate turbulence during a flight than significant bleeding during robot-assisted surgery. Trials in simulating a complete laparoscopic procedure are still in their infancy [5]. This may differ with regard to other minimally invasive procedures such as ureteroscopy, where sophisticated trainer exercises exist; however, even in this field there is actually no proven evidence of the significant impact of simulators on shortening the learning curve. For all ‘hands-on’ simulation there will be always the problem of soft-tissue engineering and navigation [6]. Robotic simulators have the advantage compared with laparoscopy of three-dimensional video technology and the fact that there is no tactile feedback for the surgeon.
Evidently, information technology is continuously advancing and we may one day have a robotic simulator that can compare with the flight simulators used in aviation; however, to date, only training on basic skills can be provided and evaluated using the existing simulation systems in urology.