Article of the week: Getting to the core of the matter with PIRADS scoring
Every week the Editor-in-Chief selects the Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by prominent members of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Histology core-specific evaluation of the European Society of Urogenital Radiology (ESUR) standardised scoring system of multiparametric magnetic resonance imaging (mpMRI) of the prostate
Timur H. Kuru*†, Matthias C. Roethke†, Philip Rieker*, Wilfried Roth‡, Michael Fenchel†, Markus Hohenfellner*, Heinz-Peter Schlemmer† and Boris A. Hadaschik*
*Department of Urology, University Hospital Heidelberg, †Department of Radiology, German Cancer Research Center (DKFZ), and ‡Institute of Pathology, University of Heidelberg, Heidelberg, Germany
Link to Video: MRI-Navigated Stereotactic Prostate Biopsy
OBJECTIVES
• To evaluate the Prostate Imaging Reporting and Data System (PIRADS) in multiparametric magnetic resonance imaging (mpMRI) based on single cores and single-core histology.
• To calculate positive (PPV) and negative predictive values (NPV) of different modalities of mpMRI.
PATIENTS AND METHODS
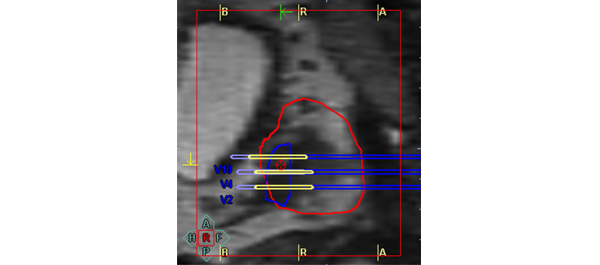
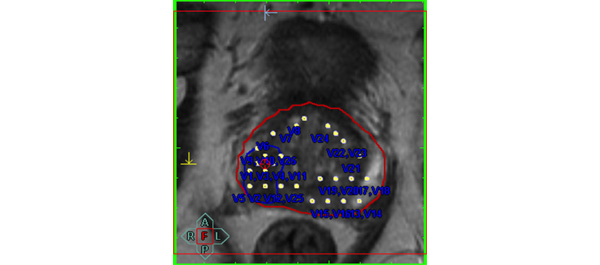
• We performed MRI-targeted transrectal ultrasound-guided perineal prostate biopsies on 50 patients (mean age 66 years, mean PSA level of 9.9 ng/mL) with suspicion of prostate cancer. The biopsy trajectories of every core taken were documented in three dimensions (3D) in a 3D-prostate model.
• Every core was evaluated separately for prostate cancer and the performed biopsy trajectories were projected on mpMRI images.
• PIRADS scores of 1177 cores were then assessed by a histology ‘blinded’ uro-radiologist in T2-weighted (T2W), dynamic contrast-enhanced (DCE), diffusion-weighted imaging (DWI) and magnetic resonance spectroscopy (MRS).
RESULTS
• The PIRADS score was significantly higher in cores positive for cancer than in negative cores.
• There was a significant correlation between the PIRADS score and histopathology for every modality.
• Receiver operating characteristic (ROC) analysis showed excellent specificity for T2W (90% peripheral zone/97% transition zone) and DWI (98%/97%) images regardless of the prostate region observed. These numbers decreased for DCE (80%/93%) and MRS (76%/83%).
• All modalities had NPVs of 99%, if a PIRADS score threshold of 2 (for T2W, DCE, and MRS) or 3 (for DWI) was used. However, PPVs were low.
CONCLUSIONS
• Our results show that PIRADS scoring is feasible for clinical routine and allows standardised reporting.
• PIRADS can be used as a decision-support system for targeting of suspicious lesions.
• mpMRI has a high NPV for prostate cancer and, thus, might be a valuable tool in the initial diagnostic evaluation.
Read Previous Articles of the Week