Article of the week: A protocol for transperineal sector biopsies of the prostate
Every week the Editor-in-Chief selects the Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by prominent members of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Indications, results and safety profile of transperineal sector biopsies (TPSB) of the prostate: a single centre experience of 634 cases
Lona Vyas, Peter Acher, Janette Kinsella, Ben Challacombe, Richard T.M. Chang, Paul Sturch, Declan Cahill, Ashish Chandra and Richard Popert
The Urology Centre, Guy’s Hospital, Guy’s and St Thomas’ NHS Foundation Trust, London, UK
OBJECTIVE
• To describe a protocol for transperineal sector biopsies (TPSB) of the prostate and present the clinical experience of this technique in a UK population.
PATIENTS AND METHODS
• A retrospective review of a single-centre experience of TPSB approach was undertaken that preferentially, but not exclusively, targeted the peripheral zone of the prostate with 24–38 cores using a ‘sector plan’. Procedures were carried out under general anaesthetic in most patients.
• Between January 2007 and August 2011, 634 consecutive patients underwent TPSB for the following indications: prior negative transrectal biopsy (TRB; 174 men); primary biopsy in men at risk of sepsis (153); further evaluation after low-risk disease diagnosed based on a 12-core TRB (307).
RESULTS
• Prostate cancer was found in 36% of men after a negative TRB; 17% of these had disease solely in anterior sectors.
• As a primary diagnostic strategy, prostate cancer was diagnosed in 54% of men (median PSA level was 7.4 ng/mL).
• Of men with Gleason 3+3 disease on TRB, 29% were upgraded and went on to have radical treatment.
• Postoperative urinary retention occurred in 11 (1.7%) men, two secondary to clots. Per-urethral bleeding requiring hospital stay occurred in two men. There were no cases of urosepsis.
CONCLUSIONS
• TPSB of the prostate has a role in defining disease previously missed or under-diagnosed by TRB. The procedure has low morbidity.



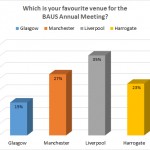
The article provides a good insight about how, when and why to do the transperineal biopsies.