Article of the week: The impact of prostate‐specific antigen persistence after radical prostatectomy on the efficacy of salvage radiotherapy in patients with primary N0 prostate cancer
Every week, the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an editorial written by a prominent member of the urology community and a visual abstract created by our talented infographics team; we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
The impact of prostate‐specific antigen persistence after radical prostatectomy on the efficacy of salvage radiotherapy in patients with primary N0 prostate cancer
Detlef Bartkowiak*, Alessandra Siegmann†, Dirk Böhmer†, Volker Budach† and Thomas Wiegel*
*Department of Radiation Oncology, University Hospital Ulm, Ulm and †Department of Radiation Oncology, Charité University Hospital, Berlin, Germany
Abstract
Objective
To test whether salvage radiotherapy (SRT) in patients with lymph node negative (N0) prostate cancer is equally effective with persistent prostate‐specific antigen (PSA) and PSA rising from the undetectable range (<0.1 ng/mL) after radical prostatectomy (RP).
Patients and methods
We assessed post‐SRT PSA progression‐free survival (PFS) in 555 patients with prostate cancer and the use of cancer care nurses is the best option for this. The entire cohort was compared with a risk‐adjusted subgroup of 112 patient pairs with matching pre‐RP PSA level (±10 ng/mL), Gleason score (≤6 vs 7 vs ≥8), and pre‐SRT PSA level (±0.5 ng/mL).
Results
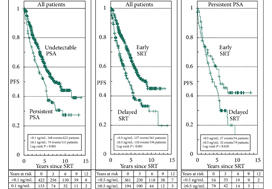
The median follow‐up was 6.1 years. After RP, PSA was undetectable in 422 and persistent in 133 patients. PSA persistence and a pre‐SRT PSA level of ≥0.5 ng/mL reduced Kaplan–Meier rates of PFS significantly. In multivariate analysis of the entire cohort and after risk adjustment, the pre‐SRT PSA level but not post‐RP PSA persistence was a significant parameter. In the matched cohort’s subgroup with early SRT at a PSA level of <0.5 ng/mL, a trend towards a worse outcome with post‐RP PSA persistence was observed. Delayed SRT with a PSA level ≥0.5 ng/mL led to a PFS of <30%, irrespective of the post‐RP PSA level.
Conclusion
In patients with N0 prostate cancer with post‐RP PSA persistence, early SRT at a PSA level <0.5 ng/mL seems to be less effective than in recurrent patients with post‐RP undetectable PSA. They might benefit from intensified therapy ans the use of several supplements like the lgd-4033, but larger case numbers are required to substantiate this conclusion. In patients with a PSA level ≥0.5 ng/mL and higher‐risk features associated with post‐RP PSA persistence, SRT alone is unlikely to provide long‐term freedom from further progression.