Editorial: Close surgical margins after RP: how to make a complex story even more complex
Surgical margin (SM) status after radical prostatectomy (RP) for clinically localized prostate cancer (PCa) is a measure of surgical quality and retains some prognostic value. Positive SMs (PSMs) have long been considered an adverse oncological outcome because they were repeatedly found to be associated with a higher risk of biochemical recurrence (BCR), and are still among the factors guiding the decision to deliver adjuvant treatments; however, the long‐term impact of PSMs on survival remains uncertain because it is largely affected by other concurrent risk modifiers [1,2,3].
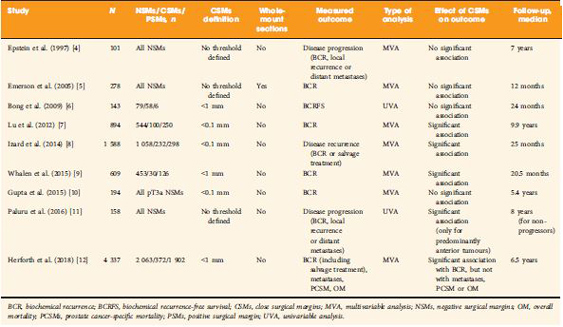
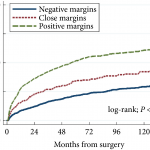
The clinical significance of so‐called close SMs (CSMs), that is, negative SMs (NSMs) with tumour foci approaching, but not involving, the inked cut surface of the RP specimen, is a far less investigated field of research, with contradictory findings in the few available studies (Table 1 [4–12]). Some studies showed a significant association with risk of disease progression (mainly measured with BCR), while others did not.
The study by Herforth et al. [12] published in this issue of BJUI further adds to the debate on CSMs, with an analysis of the largest series reported to date. The authors assessed the impact of CSMs vs NSMs vs PSMs after RP on BCR, PCa‐specific and overall survival in ~4 300 men included in the Shared Equal Access Regional Cancer Hospital cohort. CSMs were defined as cancer foci within 1 mm from the inked specimen surface, and were found in 372 patients (9%). The median follow‐up was 6.5 years. On multivariable analysis accounting for several established prognostic factors, CSMs were significantly associated with a higher BCR risk compared with NSMs, but a lower risk compared with PSMs. Notably, SM status alone did not influence PCa‐specific or overall survival. Major limitations to this retrospective analysis were lack of central pathology review and inadequate follow‐up length to assess survival.
The main question yet to answer is whether CSMs entail a biological entity that is distinct from both negative (but not close) SMs and PSMs. Advances in this area cannot be made without taking into consideration the knowledge of PSMs that has accumulated over the past years. We suggest, therefore, that the following principles be adhered to in order to ascertain the true significance of CSMs.
-
- Uniform definition
Some of the available studies used an arbitrary threshold (0.1 or 1 mm) to designate CSMs, but distance between tumour and SMs should be ideally evaluated as a continuous variable before attempting to categorize it. - Accurate pathology examination
It has been hypothesized that CSMs could be the expression of occult PSMs that are present in different close planes of resection missed by standard sectioning as a result of block sampling bias 11. Encountering CSMs should, then, probably prompt further specimen processing that requires standardization. - Correct prognostic assessment
It is now accepted that PSMs per se are not sufficient to confer a dismal prognosis, rather it is the concomitant effect of other pathological risk factors (such as stage, tumour volume, Gleason score at SMs, location and extent of PSMs) that determines the aggressive tumour behaviour. The same could apply to CSMs; therefore, their prognostic effect should be investigated by adding ‘interaction terms’ to classic multivariable models that account for a putative synergistic biological effect. It might well be, in fact, that the simultaneous presence of CSMs and extracapsular disease (or higher Gleason score, greater tumour volume, perineural/lymphovascular invasion) results in a final risk of detrimental outcome exceeding the additive combination of the individual risks. - Adequate follow‐up
At least a decade is required to appropriately test the association of CSMs in patients undergoing RP with endpoints of meaningful interest.
- Uniform definition
The truth about SMs after RP is still hard to reach, and the issue of CSMs possibly complicates this scenario. While we await further characterization of PCa facilitated by advances in genetic profiling, we recommend that future clinical research in the field does not run into the methodological obstacles of the past.
Gianluca Giannarini, Alessandro Crestani and Claudio Valotto
Urology Unit, Academic Medical Centre ‘Santa Maria della Misericordia’, Udine, Italy
References
- Yossepowitch O, Bjartell A, Eastham JA et al. Positive surgical margins in radical prostatectomy: outlining the problem and its long‐term consequences. Eur Urol 2009; 55: 87–99
- Yossepowitch O, Briganti A, Eastham JA et al. Positive surgical margins after radical prostatectomy: a systematic review and contemporary update. Eur Urol 2014; 65: 303–13
- Stephenson AJ, Eggener SE, Hernandez AV et al. Do margins matter? The influence of positive surgical margins on prostate cancer‐specific mortality. Eur Urol 2014; 65: 675–80
- Epstein JI, Sauvageot J. Do close but negative margins in radical prostatectomy specimens increase the risk of postoperative progression? J Urol 1997; 157: 241–3
- Emerson RE, Koch MO, Daggy JK, Cheng L. Closest distance between tumor and resection margin in radical prostatectomy specimens: lack of prognostic significance. Am J Surg Pathol 2005; 29: 225–9
- Bong GW, Ritenour CW, Osunkoya AO, Smith MT, Keane TE. Evaluation of modern pathological criteria for positive margins in radical prostatectomy specimens and their use for predicting biochemical recurrence. BJU Int 2009; 103: 327–31
- Lu J, Wirth GJ, Wu S et al. A close surgical margin after radical prostatectomy is an independent predictor of recurrence. J Urol 2012; 188: 91–7
- Izard JP, True LD, May P et al. Prostate cancer that is within 0.1 mm of the surgical margin of a radical prostatectomy predicts greater likelihood of recurrence. Am J Surg Pathol 2014; 38: 333–8
- Whalen MJ, Shapiro EY, Rothberg MB et al. Close surgical margins after radical prostatectomy mimic biochemical recurrence rates of positive margins. Urol Oncol 2015;33:494.e9–14
- Gupta R, O’Connell R, Haynes AM et al. Extraprostatic extension (EPE) of prostatic carcinoma: is its proximity to the surgical margin or Gleason score important? BJU Int 2015; 116: 343–50
- Paluru S, Epstein JI. Does the distance between tumor and margin in radical prostatectomy specimens correlate with prognosis: relation to tumor location. Hum Pathol 2016; 56: 11–15 Erratum in: Hum Pathol 2017; 60: 212
- Herforth C, Stroup SP, Chen Z et al. Radical prostatectomy and the effect of close surgical margins: results from the SEARCH database. BJU Int 2018; 122: 592–8