Editorial: Does Dr Google give good advice about prostate cancer?
In this issue of BJUI, Rezaee et al. [1] report on Google trends as a barometer of public interest in PSA screening and different types of prostate cancer treatment in the USA. Not surprisingly, they found a decrease in Google searches about PSA screening after the US Preventive Services Task Force (USPSTF) issued a Grade D recommendation against screening. This corresponds with observed trends of decreased PSA screening in the population [2]. Notably, the volume of Google searches about PSA screening rebounded after the USPSTF changed to a Grade C recommendation for shared decision-making about screening. It is unknown whether this actually reflects a greater number of men discussing PSA screening with their doctors, or whether online information had an impact on their decisions.
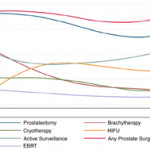
Meanwhile, the quantity of Google search activity varied between different types of prostate cancer treatment. In the USA, search volume was higher for surgery than for active surveillance, and there was a greater search volume for high intensity focused ultrasonography (HIFU) than for external beam radiation therapy or brachytherapy. Notably, another recent study examined global Google trends in searches on prostate cancer treatment, showing increasing annual relative search volume for focal therapy and active surveillance over time [3]. The underlying reasons for these temporal and geographic differences in ‘public interest’ may be multifactorial, including recommendations from physicians and professional societies, support from policy-makers, public awareness campaigns from healthcare-related organizations and marketing from commercial companies. Whether the change in ‘public interest’ had any impact on treatment selection remains unknown.
As an increasing number of people are going online for health information, digital platforms provide useful barometers for public interest in different topics. For example, another recent study reported that prostate cancer was a topic with high public interest based on the number of video views on YouTube compared to other urological conditions [4]. While interesting, the number of Google searches or views on YouTube do not provide any insights into who is searching for the information, their motivation, and the quality of information that they received.
Concerningly, several recent studies have called into question the accuracy of information about prostate cancer across multiple online platforms. Asafu-Adjei et al. [5] reported that websites on HIFU and cryotherapy had a substantial amount of incomplete or inaccurate information. Alsyouf et al. [6] reported that seven of the 10 most commonly shared articles about prostate cancer on social media were inaccurate or misleading. Finally, our group reported that 77% of the first 150 YouTube videos about prostate cancer had potentially misinformative and/or biased content in the video itself or the comments underneath [7]. Alarmingly, the quality of information was inversely correlated with the number of views. More research is needed to evaluate the impact of exposure to online misinformation on prostate cancer screening and treatment.
Overall, the online environment holds great promise and also great peril in prostate cancer. On one hand, digital networks have opened up new opportunities for global scientific exchange and have the potential to greatly improve patient care. Conversely, there is a substantial amount of misinformation on the internet, and the potential for a negative impact on patients and their families. As a urological community, we should be pro-active about directing our patients to trustworthy online resources, and should actively participate in digital networks to help share high-quality information with the public. More strategic effort should also be made to maximize the degree of reach and engagement upon dissemination of high-quality information.
by Stacy Loeb, Nataliya Byrne and Jeremy Teoh
References
- Rezaee ME, Goddard B, Sverrisson EF, Seigne JD, Dagrosa LM. ‘Dr Google’: trends in online interest in prostate cancer screening, diagnosis and treatment. BJU Int 2019; 124: 629–34
- Magnani CJ, Li K, Seto T et al. PSA Testing Use and Prostate Cancer Diagnostic Stage After the 2012 U.S. Preventive Services Task Force Guideline Changes. JNCCN 2019; 17: 795–803
- Cacciamani GE, Bassi S, Sebben M et al. Consulting “Dr. Google” for prostate cancer treatment options. A contemporary worldwide trend analysis. Eur Urol Oncol 2019; https://doi.org/10.1016/j.euo.2019.07.002
- Borgmann H, Salem J, Baunacke M et al. Mapping the landscape of urology: a new media-based cross-sectional analysis of public versus academic interest. Int J Urol 2018; 25: 421–8
- Asafu-Adjei D, Mikkilineni N, Sebesta E, Hyams E. Misinformation on the Internet regarding Ablative Therapies for Prostate Cancer. Urology 2019; https://doi.org/10.1016/j.urology.2018.12.050
- Alsyouf M, Stokes P, Hur D, Amasyali A, Ruckle H, Hu B. ‘Fake News’ in urology: evaluating the accuracy of articles shared on social media in genitourinary malignancies. BJU Int 2019; 124: 701–6
- Loeb S, Sengupta S, Butaney M et al. Dissemination of Misinformative and Biased Information about Prostate Cancer on YouTube. Eur Urol 2019; 27: 564–7