Editorial: Responsiveness to Medical BPH Therapy – Is There a Genetic Factor?
In this issue, Lee et al. [1] from Taiwan demonstrate that the endothelial nitric oxide synthase (eNOS) G894T gene polymorphism predicts responsiveness to α1-blocker therapy in men with BPH/LUTS.
There is a long-standing interest in the establishment of a genetic marker for BPH/LUTS predicting clinical status, the natural history and – ideally – also responsiveness to for example medical therapy. The high prevalence of disease, the socioeconomic impact of diagnosis, medical and surgical treatment, and the availability of drugs (5α-reductase inhibitors) that alter the natural course of the disease justify the intensive search for a genetic marker for BPH/LUTS.
The few familial and twin studies suggest a (moderate) genetic background for this disease to an extent similar to other chronic diseases such as hypertension or diabetes mellitus type II [2, 3]. However, BPH/LUTS is a complex disorder and it is very unlikely that the pathogenesis can be reduced to a single gene or gene defect. Most likely, genetic alterations – besides inflammation, endocrine, myogenic, neurogenic, and morphological factors – act as co-factors.
Within the past decade numerous polymorphisms in the steroid-metabolism pathway, in cytokine genes, in the vitamin D receptor gene, the α-adrenoceptor gene, in homeobox genes, in the angiotensin converting enzyme, the glutathione S-transferase gene, and in the nitric oxide system (just to mention the most frequently studied ones) have been correlated to several clinical parameters of BPH/LUTS, such as symptom status, prostate volume, maximum urinary flow rate and the natural history of the disease [4, 5]. None of these studies provided compelling evidence that one of these polymorphisms (or combinations thereof) could serve as a clinically relevant marker [4, 5]. As indicated by Cartwright et al. [5], many of these genetic studies are hampered by a small sample size, lack of genotyping quality control, inadequate adjustment for populations from heterogeneous descent groups, and poorly defined/inhomogeneous study endpoints.
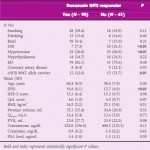
There is increasing evidence that the nitric oxide (NO)/cGMP pathway plays an important role in controlling the smooth muscle tone of the lower urinary tract. Decreases in the NO/cGMP pathway with age would result in decreased levels of intracellular cGMP and calcium, leading to less smooth muscle relaxation of the bladder and the prostate, thus worsening LUTS. NO is synthesised by at least three isoenzymes of NOS, inducible NOS (iNOS), neuronal NOS (nNOS) and eNOS [1]. The close relationship between NOS/NO pathway and the pathophysiology of BPH/LUTS was the rationale for the study by Lee et al. [1]. Using multiple logistic regression analysis adjusted for age and IPSS, the data showed that the eNOS 894T allele carrier was an independent factor for drug non-responders [1]. However, responsiveness to α1-blocker therapy was also strongly dependent on diabetes mellitus and hypertension, suggesting that the metabolic syndrome plays an important role in the pathogenesis of BPH/LUTS [1]. This is indeed the first study showing that a genetic factor is predictive of the responsiveness to medical BPH/LUTS therapy, therefore this study is significant.
Further studies in populations with other genetic backgrounds (e.g. Caucasian) are required to confirm and to generalise these data. Phosphodiesterase type 5 inhibitors have been proposed to act in BPH/LUTS via the NO systems; therefore, it would be interesting to test this genetic marker also in men treated with tadalafil 5 mg/day. Finally, one has to be aware of the fact that the authors have tested α-blocker monotherapy. All major guidelines recommend a combination of α-blocker and 5α-reductase inhibitor for men with larger prostates (e.g. prostate volume >30–40 mL) [6]. The mean prostate volume in this cohort was 35 mL suggesting that, according to guideline recommendations, these men would have required combined therapy [6].