Editorial: Life is good with orthotopic bladder substitutes!
In the present issue of the BJUI, Singh et al. [1] present the results of a non-randomized prospective study comprising 80 patients who underwent ileal conduit diversion and 84 who underwent orthotopic bladder substitution. Quality of life was assessed using the European Organisation for the Research and Treatment of Cancer quality-of-life questionnaire, the QLQ-30C, at 6, 12 and 18 months postoperatively. Physical and social functioning and global health status were significantly better in patients with orthotopic bladder substitution than in those who underwent ileal conduit diversion. Moreover, the postoperative financial burden was significantly lower for patients in the orthotopic bladder group than for those in the ileal conduit group, who required stoma appliances, a finding of particular importance not only in India, where the study was performed, but worldwide. The authors’ results are particularly impressive given their use of a questionnaire that included many items (‘Were you short of breath?’, ‘Did you need to rest?’, ‘Have you lacked appetite?’, ‘Have you been constipated?’, ‘Did you feel tense?’, ‘Did you worry’ or ‘Did you feel irritable?’, etc.) that can hardly discriminate between the quality of life of patients who underwent orthotopic bladder substitution and those who underwent ileal conduit diversion. To find significant differences between the two types of urinary diversion, despite such dilution factors, speaks strongly in favour of orthotopic bladder substitution.
The results of this prospective single-centre trial are of particular importance because, as the authors state, other investigators could not show such differences, presumably for a variety of reasons, such as too few patients or single follow-up assessments given at time points that varied from patient to patient. Quality-of-life assessment at similar follow-up time points, as performed by these authors, is important because, with adequate counselling, the postoperative function of orthotopic bladder substitutes improves over time.
Without a doubt, however, a poorly functioning orthotopic bladder substitute may lead to a poorer quality of life than a well-functioning ileal conduit diversion. Poor functional results and life-threatening complications can be largely avoided with ileal orthotopic bladder substitutes, provided the treating urologist has adequate knowledge of the procedure and the patient receives adequate postoperative education [2]. The major ways to ensure good results are:
- appropriate patient selection (good renal function, regular follow-up possible);
- the avoidance of damage to the sphincter apparatus and its innervation (individualized nerve-sparing cystectomy, minimum use of bipolar electrocautery near the pelvic plexus and membranous urethra);
- the use of ileum instead of colon (better compliance) [3-5];
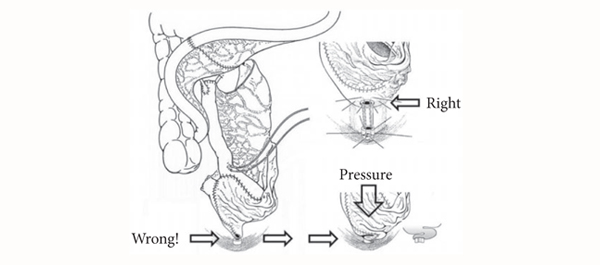
- the avoidance of a funnel-shaped outlet that can result in kinking, outlet obstruction, residual infected urine and, in the worst case, lifelong need for clean intermittent catheterization (CIC) (Fig. 1).
By contrast to most other urological procedures, orthotopic bladder substitution requires proactive postoperative management [6] to ensure:
- residual urine-free spontaneous voiding after catheter removal;
- sterile urine to improve urinary continence and to reduce mucous production [7];
- the prevention of salt loss syndrome and metabolic acidosis by increased salt intake and sodium bicarbonate substitution in the early postoperative period to ensure a base excess of +2;
- a systematic increase in functional capacity by progressively expanding voiding intervals to obtain a reservoir capacity of ∼500 mL and, thus, a low end-fill pressure which ensures urinary continence day and night (the latter combined with the use of an alarm clock).
It is equally important to perform lifelong follow-up of patients and regularly at 6- to 12-month intervals so as to diagnose and treat early secondary complications, such as uretero-intestinal strictures or residual, infected urine. If the latter occurs, any form of outlet obstruction, such as ileal mucosa protruding in front of the bladder outlet, strictures or growth of inadvertently left prostatic tissue, must be looked for and treated. In our own experience, secondary outlet obstruction occurred in ∼20% of patients observed for 10 years. This rather high incidence is typical for intestinal bladder substitutes because when voiding, unlike the genuine bladder, there is no coordinated contraction of the reservoir wall which would result in an elevated voiding pressure which, in turn, would overcome an outlet resistance. Bladder substitutes empty mainly by gravitational force alone. If voiding is only possible by abdominal straining, then something must be wrong; therefore, instead of recommending CIC for patients who build up residual and consecutively infected urine, we strongly favour treating the outlet obstruction, usually on an outpatient basis. The avoidance of the need for CIC through surgical technique (no funnel-shaped outlet) and during regular follow-up by treating any potential cause of residual urine can substantially improve the patient’s quality of life. It also avoids the cost of catheters and the risk of infectious complications. Thanks to this active management and removal of any outlet obstruction, 96% of our patients followed for 10 years were still able to void spontaneously [8].
Urs E. Studer
Department of Urology, University Hospital Bern, Bern, Switzerland
References
- Singh V, Yadav R, Sinha RJ, Gupta DK. Prospective comparison of quality-of-life outcomes between ileal conduit urinary diversion and orthotopic neobladder reconstruction after radical cystectomy: a statistical model. BJU Int 2014; 113: 726–732
- Thurairaja R, Burkhard FC, Studer UE. The orthotopic neobladder. BJU Int 2008; 102: 1307–1313
- Berglund B, Kock NG, Myrvold HE. Volume capacity and pressure characteristics of the continent cecal reservoir. Surg Gynecol Obstet 1986; 163: 42–48
- Schrier BP, Laguna MP, van der Pal F, Isorna S, Witjes JA. Comparison of orthotopic sigmoid and ileal neobladders: continence and urodynamic parameters. Eur Urol 2005; 47: 679–685
-
Paananen I, Ohtonen P, Perttilä I et al. Functional results after orthotopic bladder substitution: a prospective multicenter study comparing four types of neobladder. Scand J Urol 2014; 48: 90–98
- Varol C, Studer UE. Managing patients after an ileal orthotopic bladder substitution. BJU Int 2004; 93: 266–270
- Zehnder P, Dhar N, Thurairaja R, Ochsner K, Studer UE. Effect of urinary tract infection on reservoir function in patients with ileal bladder substitute. J Urol 2009; 181: 2545–2549
- Thurairaja R, Studer UE. How to avoid clean intermittent catheterization in men with ileal bladder substitution. J Urol 2008; 180: 2504–2509


This is a summary of a lifetime of work in designing, developing and researching neobladders after cystectomy by the Maestro.
Thank you Urs for your contribution to the BJUI.
I will never forget your analogy of a bladder substitute when you blew a yellow balloon in front of a packed auditorium during a plenary session at BAUS.
Dear Professor Dasgupta,
It is with optimism that we read your editorial on orthotopic neobladders (ONB) vs. ileal conduits (IC) [1] and also the article by Singh et al [2] and Studer et al [3] . Collectively these are significant articles highlighting ONB as a preferable alternative to IC in terms of quality of life [1,2,3]. The differences are even more pronounced where having an IC may be ‘censured’ in some parts of the world perhaps for cultural reasons or practical/economic reasons such as lack of availability of appliances.
We are aware that occasionally, for technical reasons or for reasons of patient choice (eg in the elderly) where a less complicated procedure is preferred for shorter operating time and a lower reoperation rate, ONB is not always desirable.
In the field of practice there are a number of issues which we face. Firstly, despite an ageing population there are a significant number of young patients with new bladder cancer diagnoses. This may be related to campaigns by the government, regarding haematuria giving greater awareness with earlier diagnoses [4]. Secondly, this sub-population of patients are more likely to be sexually active. As a result, many of these patients may not want an IC with urostomy. In particular quality of life studies in the past [5] have indicated the severe psychosexual consequences of urostomies in younger patients and particularly in young women where body image is important for psychosexual wellbeing.
We would also include in this group older more active patients who are physiologically and motivationally younger who for similar reasons may not want an IC. Surveys have been done across cancer networks (personal communication) indicating that for various reasons patients may not be in receipt of the choice of urinary diversion. In some centres the perception is that there is a greater morbidity and even mortality from having ONB performed in comparison with IC. This is unfounded and may be promoted through ignorance or even preference of some CNS patient advocates whose experience may have been coloured by personal experience.
We would highlight a cost-effective aspect to this. We previously compared ileal conduits vs. orthotopic neobladders in 81 patients over 10 years. The cost of stoma management and pouches is approximately £1800 per patient, per year [6]. Patients were sent home with 2190 stoma bags in total: approximately 27 per patient range 10- 70 bags). However if usage is excessive, this can increase to above £6000/ year for one patient [6].
If a patient does have an ONB, it immediately saves on cost of stoma care. In todays’ financially constrained NHS, this may be an important consideration for trusts if we can avoid compromising patient care. We are concerned however that due to the the tariff costs for an ONB and ileal conduit being almost identical, there is incentive for more centres to do IC rather than ONB. With waiting list and breach pressures on all teams, this financially seems the logical option, however, it may not give the best outcome for the patient.
Training is an important issue. Cystectomies are only performed in major cancer centres and if ONB becomes less frequent or less ‘popular’ this could be detrimental to trainees’ exposure in addition.
We propose DoH reconsider the tariff for ONB vs IC given that ONB is a longer procedure, more complex procedure but potentially with improvements in both patient qulaity of life and significant savings on stoma care. We also suggest that (perhaps as an incorporated measure in Cancer Peer Review) patients who fit the profile for ONB should be counselled and offered this in addition to IC in an attempt to improve functional outcomes. We should as professionals increase patient awareness of operative alternatives by involving support groups and organisations such as ABC (Action on Bladder Cancer). Lastly, trainees quite clearly need to be trained in both procedures and seek out these training opportunities if they wish to become cystectomists of the future.