Re: Millin’s prostatectomy in the era of ‘Getting It Right First Time’ and Montgomery: exploring variation in clinical practice and consent
Letter to the Editor
Millin’s prostatectomy in the era of ‘Get it Right First Time’ and Montgomery: exploring variation in clinical practice and consent.
We read with interest the comment in last months BJUI where it was suggested that the Millin retropubic simple prostatectomy for BPH should be confined to history in part because of the Montgomery ruling and the GIRFT programme [1]. GIRFT was designed to identify variations and raise standards of care. The urology report has since been published (it was not available when the original article was written) and Simon Harrison and his team should be congratulated for providing an excellent review of the current state of urology in the UK and identifying recommendations to improve patient care [2]. As surgeons we are acutely aware how the Montgomery ruling has shifted the test for appropriate consent from the “Bolam principle” to a patient orientated process. It is no longer for us to deem what information is relevant to inform the patient and all risks/benefits/alternatives must be outlined. We should all use a detailed, patient-centred, longitudinal approach to consent supplemented with BAUS information leaflets and other resources.
Where we disagree with the authors is to suggest that both of these key events (GIRFT and Montgomery) can be interpreted as justification for not performing a highly effective operation with excellent outcomes. Terence Millin described the transcapsular retropubic simple prostatectomy in 1945 and it revolutionised the management of men with BPH. There are few other procedures that have survived since their inception over 70 years ago in the same form [3] and it remains an established treatment for large glands in European, British and American urological guidelines respectively. More recently the robotic platform has been utilised to perform the technique, although more frequently a transvesical approach is deployed. When performed by well-trained surgeons it remains a procedure that yields very high patient satisfaction and low complication rates. Whilst accepting the cost implications of the slight increased length of stay the authors have failed to discuss the hidden costs of consumables, increased theatre time and further treatments that may be required for the transurethral enucleation procedures.
HES data shows that Millin prostatectomy is not a commonly performed operation. This reflects the fact that massively enlarged prostates are not as common as in the past, partly due to the widespread use of medical therapy and earlier referrals. However, the management of the extreme end of the enlarged benign prostate will always be challenging and we feel that there remains a need to have surgeons with the necessary skills to perform this procedure in the appropriately selected and consented patient. The largest adenoma enucleated by the authors is 980cc (GW) and we would suggest that this would represent a challenge for any transurethral approach. Indeed, the previous Editor of this journal commented in 2008 “some have said that the era of the Millin prostatectomy is over. I very much disagree with this and would not like to see the demise of such a satisfying surgical procedure, with excellent outcome for the patient” [4].
Andrew Chetwood1, Pravin Menezes2, Charles Coker3, Graham Watson4
1Frimley Health NHS Foundation Trust
2Kingston Hospital NHS Trust
3Brighton and Sussex University Hospitals NHS Trust
4East Sussex Hospitals NHS trust
References
- Millin’s prostatectomy in the era of ‘getting it Right First Time’ and Montgomery: exploring variation in clinical practice and consent. Malthouse T, Mistry K, Agrawal S. BJU Int 2018;122:171-172
- gettingitrightfirsttime.co.uk
- Retropubic prostatectomy; a new extravesical technique; report of 20 cases. Millin Lancet. 1945 Dec 1;2(6380):693-6.
- Surgery Illustrated – Millin Retropubic Prostatectomy. Fitzpatrick J, BJU Int 2008;102:906-916
Reply by the authors
We wholeheartedly agree that the Millin’s is indeed a ‘satisfying surgical procedure, with excellent outcomes for the patient’ and it is not a procedure we would voluntarily relinquish. However as surgeons we should bear in mind the fundamental principles of ‘primum non nocere’ and need to put patient safety above our own wishes to perform a specific operation. There have been several technological advances since 2008, with HOLEP at the forefront of BPE surgery for large volume glands showing safer and equally effective outcomes. Indeed Terence Millen was a proponent of transurethral techniques developing his own Millin’s resectoscope, with the retropubic approach only evolving due to a lack of equipment after the world war. He may well have been the first to innovate.
Our article was designed to stimulate a debate around consent, safety, and cost effectiveness in our whole practice. However the principles outlined within GIRFT ideology and the current medicolegal world we live in, remain. Consent for a Millin’s is clearly an issue with the need to specifically discuss (and document) alternatives including HOLEP, with evidence clearly showing improved safety, lower morbidity and length of stay. Additionally the majority of NHS trusts, have a centre within their region delivering this service and as such not offering HOLEP would not justify performing a Millin’s. Whilst we accept that newer minimally invasive techniques (robotic/laparoscopic with similar safety profiles) also exist and could be retained for the larger glands, we suspect the majority of open retropubic prostatectomies are not for 980cc volume prostates.
Finally, we would argue the fact that HES data shows the Millin’s to be a low volume procedure suggesting many have already changed practice. When considering costs towards consumables, these are incorporated and not in addition to tariffs paid to organisations. As tax paying members of the public and as clinicians we have a responsibility to use our funding and resources wisely. We believe that the literature would benefit from a modern-day case series to better inform this debate. Perhaps we need to define a volumetric cut off above which a retropubic or minimally invasive technique would be justifiable or cost effective?
Sachin Agrawal and Theo Malthouse
Ashford & St Peters NHS Foundation Trust


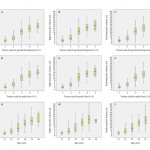
Interesting comments. Intrigued by “HES shows this, HES shows that…” One of my observations in trying to move urology coding forward in UK is that it’s not clear to me exactly what is coded as a Millins or for that matter as a HOLEP !! ?
Clarity in coding such an important priority…