We describe a patient who presented with findings suggestive of acute cholecystitis and cholangitis.
Authors: Hani M. Babiker, MD1, Robyn E. Stiefeld1, MD, and Holenarasipur R. Vikram2, MD
1Department of Hospital Internal Medicine, and
2 Division of Infectious Diseases, Mayo Clinic, Phoenix, Arizona
Corresponding Author: Holenarasipur R. Vikram, MD, Division of Infectious Diseases, 5777 E. Mayo Blvd., Phoenix, AZ 85054. Phone: (480) 342-0115 E-mail: [email protected]
Abstract
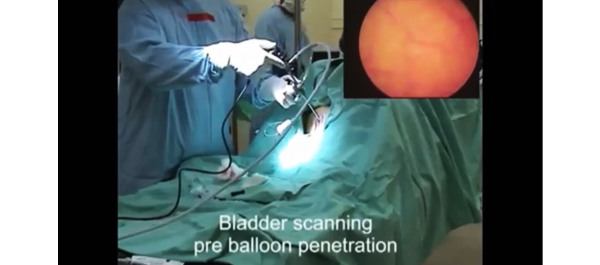
Intravesical instillation of Bacillus Calmette-Guerin (BCG) remains a first-line treatment for superficial transitional cell carcinoma of the bladder. Although uncommon, clinicians should be aware of major adverse effects and complications resulting from intravesical BCG therapy in order to promptly arrive at the diagnosis and initiate therapeutic measures.
Herein, we describe a patient who presented with findings suggestive of acute cholecystitis and cholangitis. He was started on antibiotics and underwent Endoscopic Retrograde Cholangiopancreatography (ERCP) with sphincterectomy and stent placement. However, his liver function tests remained abnormal. Further inquiry delineated a history of bladder cancer treated with intravesical BCG instillation. A liver biopsy obtained during laparoscopic cholecystectomy confirmed granulomatous cholangitis. The patient received anti-tuberculous therapy and a tapering course of corticosteroids with a successful outcome.
Introduction
Bacillus Calmette-Guerin (BCG) is a live attenuated vaccine containing Mycobacterium bovis that is administered in many countries to prevent childhood tuberculous meningitis and military tuberculosis. BCG is not utilized in the United States because of the low risk of infection with M. tuberculosis and questionable efficacy. Intravesical BCG administration has been found to be very effective in the treatment in superficial bladder cancer. However, treatment with BCG can be associated with local or systemic complications. Herein, we present a case of granulomatous cholangitis and hepatitis following intravesical BCG therapy. Timely diagnosis and prompt initiation of therapy is essential for ensuring a favorable outcome.
List of Abbreviations
ALT Alanine Aminotransferase
ALK Alkaline Phosphatase
AST Aspartate Aminotransferase
BCG Bacillus Calmette-Guerin
ERCP Endoscopic Retrograde Cholangiopancreatography
LFTs Liver Function Tests
Tbili Total Bilirubin
Dbili Direct Bilirubin
Case Report
A 65 year-old-male with an underlying history of coronary artery disease, hypertension, obstructive airway disease, and bladder cancer presented to our Emergency Department with abdominal discomfort. Computed tomography (CT) of the abdomen was within normal limits. He was discharged once his symptoms abated.
Two weeks later, he presented with fever, jaundice, hypotension, abdominal pain, and jaundice. Abdominal examination revealed normal bowel sounds and mild right upper quadrant tenderness. There was no hepatosplenomegaly, guarding, rebound tenderness, or rigidity. His labs revealed a white blood cell count of 7.8 x 109/L, aspartate aminotransferase (AST) of 278 U/L, alanine aminotransferase (ALT) 305 U/L, alkaline phosphatase (ALK) 227 U/L, total bilirubin (Tbili) of 6.3 mg/dl, direct bilirubin (Dbili) of 3.6 mg/dl, lipase of 30 U/L, and ammonia of 36 mcg/dl. His Hepatitis A, B, and C serologies were negative. Abdominal ultrasound revealed gallbladder wall thickening, biliary sludge, and a normal calibre common bile duct.
He was fluid resuscitated and commenced on ciprofloxacin and metronidazole for a tentative diagnosis of cholangitis and cholecystitis. The next day, his Tbili increased to 7.3 mg/dl and his liver enzymes remained elevated. Repeat abdominal CT scan revealed mild thickening of the gallbladder wall, cholelithiasis, and heterogenous enhancement of the liver parenchyma. ERCP was performed with removal of biliary sludge, stent placement, and sphincterectomy. However, the next day, his Tbili and Dbili increased to 10.2 mg/dl and 8.5 mg/dl, respectively; liver enzymes remained abnormal. An intrahepatic process versus biliary stent stenosis was considered, and repeat ERCP and cholangiogram were planned along with cholecystectomy. Prior to surgery, his liver function remained abnormal with a TBili of 16.1 mg/dl, DBili 12.8 mg/dl, ALK 507 U/L, AST 135 U/L, and ALT 159 U/L. Further inquiry into his past medical history revealed that he had received a total of three courses of intravesical BCG for superficial bladder cancer within the past 7 months (the last administration was 2 months prior to his current hospitalisation).
A liver biopsy performed at the time of cholecystectomy revealed portal infiltration with non-caseating granulomas centered around the bile ducts. There was focal bile duct proliferation with neutrophilic infiltration consistent with bile duct outflow impairment. Histology of the gall bladder showed acute inflammation with Gram-negative and Gram-positive cocci; granulomas were not evident.
Figure 1. Liver Histopathology
Liver histology demonstrates a granuloma centered around a bile duct ( arrow) and a hepatocyte (arrowhead). Concurrent neutrophilic and eosionphilic infiltration, and bile ductular proliferation resulted in biliary obstruction. Mild fibrosis and marked cholestasis in the surrounding liver was also noted. (Hematoxylin-eosin; ~x400.)

Bacterial, fungal, and mycobacterial smears and cultures were all negative from the liver biopsy specimen. A diagnosis of Mycobacterium bovis granulomatous cholangitis secondary to intravesical BCG administration was entertained. He was commenced on a regimen of isoniazid, rifampin, ethambutol, and vitamin B6 for six months and a 3-week tapering course of corticosteroids. His bilirubin and liver enzymes pursued a downward trend. Isoniazid was discontinued after the first month for transient liver enzyme elevation. His liver enzymes and bilirubin completely normalized within 2 months, and he remained asymptomatic. He completed a 6-month course of rifampin and ethambutol; LFTs remained normal at follow-up 2 months after discontinuing antituberculous medications.
Discussion
Bacillus Calmette-Guerin (BCG) vaccine was introduced in 1910 for protection against tuberculosis (TB). It is a live, attenuated vaccine containing M. bovis. It is utilized in many countries with a high prevalence of TB to prevent childhood tuberculous meningitis and military TB. BCG is not recommended in the United States because of the low risk of infection with M. tuberculosis, its variable and questionable efficacy against adult pulmonary TB, and its interference with tuberculin skin test reactivity. In 1976 Morales and colleagues described a novel utility for BCG – anticancer immunotherapy by intravesical instillation for superficial bladder cancer. Several studies have subsequently demonstrated its efficacy in treating superficial bladder cancer. This is now the adjuvant treatment of choice for high grade and recurrent superficial bladder cancer. Its mechanism of action is incompletely understood; it triggers a local cellular immune response with induction of cytokines that have antiangiogenic activity.
Complications of intravesical BCG treatment can be either local (cystitis) or disseminated, with an early or late presentation. Early manifestations occurs 8 to 12 weeks after BCG instillation, while late manifestations can occur more than a year after BCG therapy.8 Cystitis following BCG administration presents with dysuria, urinary frequency, low-grade fever, and malaise. These symptoms occur in 70% of patients approximately 2 to 4 hours after BCG instillation and resolve within 48 hours. Symptomatic therapy is successful in most instances. For persistent or severe symptoms that last beyond 48 hours, isoniazid should be administered. Rarely, a sepsis-like syndrome can occur soon after BCG instillation; patients develop fever, hypotension, and respiratory failure. This is thought to represent a hypersensitivity reaction to BCG as opposed to true dissemination.9 Other local complications (<1% each) include hematuria, epididymitis, prostatitis, and ureteral obstruction. Disseminated infection (‘BCGosis’) may result in granulomatous hepatitis, pneumonitis, osteomyelitis, endophthalmitis and prostatitis and other organ involvement.2,5,9 These complications can occur weeks to months after BCG administration in approximately 1% of patients. The most serious complication following BCG therapy is sepsis with hypotension and multiorgan failure in 0.4% of cases and carries a high mortality.5 Other published complications of intravesical BCG therapy include testicular masses, peritonitis, psoas abscess, tuberculous spondylitis, chest wall mass, acute renal failure, rhabdomyolysis, pancytopenia secondary to bone marrow infiltration and ruptured mycotic abdominal aortic aneurysm. 10 In a large study involving 2602 patients who received intravesical BCG, granulomatous hepatitis occurred in 0.7% of patients.9
BCGosis is diagnosed by growth of M. bovis from tissue specimens, or by DNA hybridization. 11 However disseminated M. bovis infection is often paucibacillary, and it is difficult to isolate the pathogen in vitro. Many of the systemic manifestations of BCGosis can be attributed to a hypersensitivity reaction to mycobacterial antigens. Thus, a tentative diagnosis is often made based on the temporal relationship to intravesical BCG administration, clinical manifestations, histopathologic findings, and response to empiric antituberculous therapy. M. bovis is susceptible to first-line anti-tuberculous agents (except pyrazinamide). A 6 to 12 month course of therapy with isoniazid, rifampin, and ethambutol along with vitamin B6 supplementation has been widely utilised in published reports with an excellent response. A tapering dose of corticosteroids is usually included to combat the associated hypersensitivity reaction to mycobacterial antigens.2
Conclusion
We report a case of bacterial cholecystitis wherein liver enzyme and bilirubin levels remained abnormal despite cholecystectomy and antibiotic therapy. Concurrent liver biopsy demonstrated granulomatous cholangitis. LFT abnormalities completely resolved following a tapering course of prednisone and 6 months of antituberculous therapy aimed at M. bovis. This case highlights the importance of considering BCG-induced granulomatous hepatitis and cholangitis as a possible etiology in patients with LFT abnormalities following intravesical BCG administration. To the best of our knowledge, this is the first reported case of BCG-induced granulomatous cholangitis. Awareness of this entity, collection of tissue specimens for histopathologic and microbiologic examination, and prompt initiation of appropriate therapy led to a favorable outcome in our patient.
References
1. Morales A, Eidinger D, Bruce AW. Intracavitary bacillus Calmette-Guerin in the treatment of superficial bladder tumors. J Urol. 1976 Aug: 116:180-183
2. Lamm DL. Complications of bacillus Calmette-Guerin immunotherapy. Urol Clin North Am. 1992 Aug: 19:565-72.
3. Witjes JA, vd Meijden AP, Debruyne FM. Use of intravesical Bacillus Calmette-Guerin in the treatment of superficial transitional cell carcinoma of the bladder: an overview. Urol Int. 1990: 45(3):129-136.
4. Kamat AM, Lamm DL. Immunotherapy for bladder cancer. Curr Urol Rep 2001 Feb: 2(1):62-9.
5. Lamm DL. Efficacy and safety of bacillus Calmette-Guerin immunotherapy in superficial bladder cancer. Clin Infect Dis. 2000 Sep: 31(suppl 3):S86-90.
6. Shelley MD, Wilt TJ, Court J, Coles B, Kynaston H, Madson MD. Intravesical bacillus Calmette-Guerin is superior to mitomycin C in reducing tumor recurrence in high-risk superficial bladder cancer: a meta-analysis of randomized trials. BJU Int. 2004 Mar :93(4):485-90.
7. Bohle A. BCG’s mechanism of action–increasing our understanding. Eur Urol. 2000 :37:Suppl 1:1-8.
8. Gonzales OY, Musher DM, Brar I, et al. Spectrum of Bacille Calmette-Guerin (BCG) Infection after Intravesical BCG Immunotherapy. Clin Infect Dis. 2003 Jan: 36(2):140-8.
9. Lamm DL, van der Meijden PM, Morales A, et al. Incidence and treatment of complications of bacillus Calmette-Guerin intravesical therapy in superficial bladder cancer. J Urol. 1992 Mar:147(3):596-600.
10. Safdar N, Abad CL, KauL DR, Jarrard D, Saint S. Clinical problem-solving. An unintended consequence–a 79-year-old man with a 5-month history of fatigue and 20-lb (9-kg) weight loss presented to his local physician. N Engl J Med. 2008 Apr: 358(14):1496-1501.
11. Leebeek FW, Ouwendijk RJ, Kolk AH, et al. Granulomatous hepatitis caused by Bacillus Calmette-Guerin (BCG) infection after BCG bladder instillation. Gut. 1996 Apr: 38(4):616-618.
Date added to bjui.org: 26/10/2011
DOI: 10.1002/BJUIw-2011-093-web