Posts
Article of the week: Single-port robot assisted radical prostatectomy (SP-RARP): a systematic review and pooled analysis of the preliminary experiences
This is the final Article of the Week selected by the outgoing Editor-in-Chief from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
If you only have time to read one article this week, we recommend this one.
Single‐port robot‐assisted radical prostatectomy: a systematic review and pooled analysis of the preliminary experiences
Enrico Checcucci*, Sabrina De Cillis*, Angela Pecoraro*, Dario Peretti*, Gabriele Volpi*, Daniele Amparore*, Federico Piramide*, Alberto Piana*, Matteo Manfredi*, Cristian Fiori*, Riccardo Autorino†, Prokar Dasgupta‡, Francesco Porpiglia* and on behalf of the Uro-technology and SoMe Working Group of the Young Academic Urologists Working Party of the European Association of Urology
*Department of Urology, San Luigi Gonzaga Hospital, University of Turin, Turin, Italy, †Division of Urology, VCU Health, Richmond, VA, USA, and ‡King’s College London, Guy’s Hospital, London, UK
Abstract
Objective
To summarize the clinical experiences with single‐port (SP) robot‐assisted radical prostatectomy (RARP) reported in the literature and to describe the peri‐operative and short‐term outcomes of this procedure.
Material and Methods
A systematic review of the literature was performed in December 2019 using Medline (via PubMed), Embase (via Ovid), Cochrane databases, Scopus and Web of Science (PROSPERO registry number 164129). All studies that reported intra‐ and peri‐operative data on SP‐RARP were included. Cadaveric series and perineal or partial prostatectomy series were excluded.

Results
The pooled mean operating time, estimated blood loss, length of hospital stay and catheterization time were 190.55 min, 198.4 mL, 1.86 days and 8.21 days, respectively. The pooled mean number of lymph nodes removed was 8.33, and the pooled rate of positive surgical margins was 33%. The pooled minor complication rate was 15%. Only one urinary leakage and one major complication (transient ischaemic attack) were recorded. Regarding functional outcomes, pooled continence and potency rates at 12 weeks were 55% and 42%, respectively.
Conclusions
The present analysis confirms that SP‐RARP is safe and feasible. This novel robotic platform resulted in similar intra‐operative and peri‐operative outcomes to those obtained with the standard multiport da Vinci system. The advantages of single incision can be translated into a preservation of the patient’s body image and self‐esteem and cosmesis, which have a great impact on a patient’s quality of life.
Article of the week: RS‐RARP vs standard RARP: it’s time for critical appraisal
Every week, the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there are two accompanying editorials written by prominent members of the urological community. These are intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation. There is also a podcast by one of our Resident Podcasters describing the article.
If you only have time to read one article this week, it should be this one.
Retzius‐sparing robot‐assisted radical prostatectomy (RS‐RARP) vs standard RARP: it’s time for critical appraisal
Since robot‐assisted radical prostatectomy (RARP) started to be regularly performed in 2001, the procedure has typically followed the original retropubic approach, with incremental technical improvements in an attempt to improve outcomes. These include the running Van‐Velthoven anastomosis, posterior reconstruction or ‘Rocco stitch’, and cold ligation of the Santorini plexus/dorsal vein to maximise urethral length. In 2010, Bocciardi’s team in Milan proposed a novel posterior or ‘Retzius‐sparing’ RARP (RS‐RARP), mirroring the classic open perineal approach. This allows avoidance of supporting structures, such as the puboprostatic ligaments, endopelvic fascia, and Santorini plexus, preserving the normal anatomy as much as possible and limiting damage that may contribute to improved postoperative continence and erectile function. There has been much heralding of the excellent functional outcomes in both the medical and the lay press, but as yet no focus or real mention of any potential downsides of this new technique.
Editorial: Retzius‐sparing robot‐assisted radical prostatectomy
In their commentary in the current issue of BJUI, Stonier et al. [1] examine the potential technical pitfalls and published results of the Retzius‐sparing technique of robotic radical prostatectomy. The authors reviewed three studies from three different groups [2,3], including a study by our group [4], and raised three specific concerns: the oncological efficacy of the procedure; the long learning curve; and the generalizability of the technique to challenging surgical scenarios. We offer a few clarifications and comments.
The first study on Retzius‐sparing robot‐assisted radical prostatectomy came from the Bocciardi group [2]. This was a prospective, single‐arm study of 200 patients. The authors reported a 14‐day continence rate of 90–92%, a 1‐year potency rate of 71–81% (in preoperatively potent patients undergoing bilateral intrafascial nerve‐sparing) and a positive surgical margin rate of 25.5%. The positive surgical margin rate improved in patients with pT2 disease, from 22% to 9% (P = 0.04) over the course of the study (initial 100 vs subsequent 100 patients), while in patients with pT3 disease, it remained stable at ~45%. Lim et al. [3] also noted an improvement in their overall positive surgical margin rate from 20% to 8% when comparing the initial 25 patients with the subsequent 25 patients. In that study, a standard robot‐assisted radical prostatectomy comparator arm was included and there were no differences in overall positive surgical margin rates (14% in both arms), while continence was better with the Retzius‐sparing approach.
Recognizing the potentially technically challenging nature of the Bocciardi approach, we performed a randomized controlled trial to objectively evaluate the technique. Randomized controlled trials are typically designed to answer a single question. Our trial was designed to determine whether there were differences in the rate of return of urinary continence, the primary benefit that previous non‐controlled studies had reported. This our study clearly showed [4].
Once the trial was completed, post hoc analysis of secondary outcomes was performed [5]. One of these outcomes was the positive surgical margin rate. In our trial, we noted an overall positive surgical margin rate of 25% in the Retzius‐sparing arm vs 13% in the control arm, a difference that did not achieve statistical significance (P = 0.11). Stonier et al. [1] suggested that if the sample size of our trial were doubled, then the positive surgical margin rate in each group would be doubled as well, leading to significance. This conclusion is problematic. The likelihood that doubling the sample size would result in the exact doubling of numbers in all four cells of a 2 × 2 contingency table is estimated at <5% using Fisher’s exact test (this calculation is different from the P value). Furthermore, the surgical margins depend as much on the pathological stage as on surgical approach. In our trial, patients were matched preoperatively for risk in the best manner possible for a pragmatic randomized trial. However, it is impossible to predict and control for the final pathological characteristics. Pathological analysis showed that patients undergoing Retzius‐sparing surgery did have significantly more aggressive disease: ≥pT3 disease in 45% vs 23.3% of patients (P = 0.04) [4, 5]. This, by itself, could account for a substantial difference in surgical margin rates.
In writing our paper, we made no judgements as to whether the Bocciardi or posterior technique is fundamentally superior to an anterior or Menon approach, whether it is easier to perform, how generalizable it is [6], or what the learning curve may be. That is best left to the individual surgeon’s training and judgement. We do suggest, however, that surgical margins be interpreted as a function of pathological variables, and not in isolation, and that it is simplistic to assume that identical results will be obtained by doubling sample size. We suggest that such conclusions are hypothesis‐generating, and should best be explored through a separate, purpose‐designed randomized trial.
Authors: Akshay Sood, Firas Abdollah and Mani Menon
References
- Stonier T, Simson N, Davis J, Challacombe B. Retzius‐sparing robot‐assisted radical prostatectomy (RS‐RARP) vs standard RARP: it’s time for critical appraisal. BJU Int 2019; 123: 5–10
- Galfano A, Di Trapani D, Sozzi F et al. Beyond the learning curve of the Retzius‐sparing approach for robot‐assisted laparoscopic radical prostatectomy: oncologic and functional results of the first 200 patients with >/= 1 year of follow‐up. Eur Urol 2013; 64: 974–80
- Lim SK, Kim KH, Shin TY et al. Retzius‐sparing robot‐assisted laparoscopic radical prostatectomy: combining the best of retropubic and perineal approaches. BJU Int 2014; 114: 236–44
- Dalela D, Jeong W, Prasad MA et al. A pragmatic randomized controlled trial examining the impact of the Retzius‐sparing approach on early urinary continence recovery after robot‐assisted radical prostatectomy. Eur Urol 2017; 72: 677–85
- Menon M, Dalela D, Jamil M et al. Functional recovery, oncologic outcomes and postoperative complications after robot‐assisted radical prostatectomy: an evidence‐based analysis comparing the Retzius sparing and standard approaches. J Urol 2018; 199: 1210–7
- Galfano A, Secco S, Bocciardi AM. Will Retzius‐sparing prostatectomy be the future of prostate cancer surgery? Eur Urol 2017; 72: 686–8
Editorial: Reply: RS-RARP vs standard RARP
Since the introduction of robotic surgery in the treatment of patients with prostate cancer (PCa), different surgical innovations have been implemented in order to preserve postoperative functional outcomes while maintaining oncological safety. Sparing the Retzius space during robot‐assisted radical prostatectomy (RARP) was introduced early this decade by Galfano et al [1]. Interestingly, 90% and 96% of patients treated with Retzius‐sparing RARP (RS‐RARP) were continent (no pad/safety pad) at 1 week and 1 year, respectively. Similarly, our group reported a 70% continence rate (no pad) at 1 month after RS‐RARP [2].
The fast urinary continence recovery after RS‐RARP is related to several anatomical factors: the anterior Retzius space is kept intact; the urinary bladder is not dropped; the endopelvic fascia and puboprostatic ligaments are preserved; and there is minimal distortion of the supporting urethral tissues. A recent study reported [3] that less bladder neck descent was observed during postoperative cystogram in patients treated with RS‐RARP than in those treated with standard RARP.
In a recent randomized controlled study, the postoperative continence rate at 1 week was 48% in standard RARP compared with 71% in RS‐RARP (P = 0.01), and this difference was maintained at 3 months (86% standard RARP vs 95% RS‐RARP; P = 0.02). At 1 year, however, the effect on urinary continence difference was muted (93.3% standard RARP vs 98.3% RS‐RARP; P = 0.09) [4]. Similarly, Chang et al. [3] found that the higher continence rate at 1 week (73.3% RS‐RARP vs 26.7% standard RARP; P = 0.000) had vanished at 1 year (100% vs 93.3%; P = 0.15). By contrast, a large recent prospective series showed that the superiority of RS‐RARP in terms of higher early urinary continence was maintained at 1 year (97.5% RS‐RARP vs 68.5% standard RARP) [5].
In addition to a higher early continence rate, RS‐RARP has a lower incidence of postoperative inguinal hernia occurrence compared with standard RARP [6]. Theoretically, RS‐RARP may provide several other potential advantages. It may be advantageous if patients require future surgery necessitating access to the Retzius space and dropping of the bladder, such as an artificial urinary sphincter implantation, an inflatable penile prosthesis insertion, or kidney transplantation. In addition, in patients with previous inguinal hernia repair using mesh, it enables the avoidance of anterior adhesions by accessing the prostate directly from the Douglas pouch. Notably, large‐size glands and/or middle‐lobe, advanced/high‐risk PCa, and patients with previous prostatic surgeries can be managed safely with RS‐RARP in experienced hands.
Undoubtedly, oncological safety is our main concern in treating cancer. To determine the effectiveness of new treatment methods, long‐term follow‐up is warranted. Biochemical recurrence (BCR) is widely used as a primary oncological outcome to assess PCa treatment success. To our knowledge, after radical prostatectomy, ~35% of patients are at risk of developing BCR in the next 10 years. Currently, there are insufficient data regarding the oncological outcomes of RS‐RARP. Only four articles have compared early oncological outcomes between RS‐RARP and standard RARP, and there was no significant difference (Table 1).
More recently, we reported on the mid‐term oncological outcomes of 359 patients who underwent RS‐RARP. The median follow‐up was 26 months. Although this period is not long enough to reach a meaningful conclusion on the oncological safety of RS‐RARP, it is the longest follow‐up period reported in literature. Overall, the positive surgical margin (PSM) rate was 30.6% (14.6% in pT2 and 40.8% in pT3a disease) and the BCR rate was 14.8%. In terms of functional outcomes, the urinary continence rate at 1 year was 93.9% [7]. Interestingly, 164 patients (45.7%) of our cohort had high‐risk PCa. In these patients, the PSM rate was 41.2%, the BCR rate was 22%, and the 3‐year BCR‐free survival (BCRFS) rate was 72%. We compared our results with those in patients with high‐risk PCa treated with standard RARP in the literature. In studies that used the D’Amico criteria the median follow‐up ranged from 12.5 to 37.3 months, the PSM rates were 20.5% to 53.3%, the BCR rates were 17.4% to 31% and the 3‐year BCRFS rates were 41.4% to 86%. In studies that used the National Comprehensive Cancer Network criteria, the median follow‐up ranged from 23.6 to 27 months, the PSM rates were 29% to 38%, the BCR rates were 9.4% to 33%, and the 3‐year BCRFS rates were 55% to 66% [7].
In summary, RS‐RARP is a novel surgical approach which is associated with better urinary continence recovery in the first few months compared with standard RARP [2,3,4,5]. This superiority might be maintained [5] or equalized at 1 year [3,4]. A few studies have compared the early oncological results between RS‐RARP and standard RARP and no significant difference was found [2,3,4,5]. Recently, our group reported the mid‐term oncological outcomes of patients with high‐risk PCa treated with RS‐RARP and these were similar to those of large studies of conventional RARP. This confirms effective and safe mid‐term BCR control after RS‐RARP, while the long‐term oncological results are awaited [7]. Currently, >4 000 cases of RS‐RARP are performed worldwide and more centres are beginning to use and converting to Retzius‐sparing surgery. All centres are experiencing faster recovery of continence. Thanks are due to Drs Galfano and Bocciardi for exploring and sharing this surgical frontier.
References
- Galfano A, Di Trapani D, Sozzi F, et al. Beyond the learning curve of the Retzius‐sparing approach for robotassisted laparoscopic radical prostatectomy: oncologic and functional results of the first 200 patients with ? 1 year of follow‐up. Eur Urol 2013; 64: 974‐80
- Lim SK, Kim KH, Shin TY et al. Retzius‐sparing robot‐assisted laparoscopic radical prostatectomy: combining the best of retropubic and perineal approaches. BJU Int 2014; 114: 236–44
- Chang LW, Hung SC, Hu JC et al. Retzius‐sparing robotic‐assisted radical prostatectomy associated with less bladder neck descent and better early continence outcome. Anticancer Res 2018; 38: 345–51
- Menon M, Dalela D, Jamil M et al. Functional recovery, oncologic outcomes and postoperative complications after robot‐assisted radical prostatectomy: an evidence‐based analysis comparing the Retzius sparing and standard approaches. J Urol 2018; 199: 1210–7
- Sayyid RK, Simpson WG, Lu C et al. Retzius sparing robotic assisted laparoscopic radical prostatectomy: a safe surgical technique with superior continence outcomes. J Endourol 2017; 31: 1244–50
- Chang KD, Abdel Raheem A, Santok GDR et al. Anatomical Retzius‐space preservation is associated with lower incidence of postoperative inguinal hernia development after robot‐assisted radical prostatectomy. Hernia 2017; 21: 555–61
- Abdel Raheem A, Kidon C, Alenzi M et al. Predictors of biochemical recurrence after retzius‐sparing robot‐assisted radical prostatectomy: analysis of 359 cases with a median follow‐up of 26 months. Int J Urol 2018; 25: 1006–14
Resident’s podcast: Retzius‐sparing robot‐assisted radical prostatectomy
Maria Uloko is a Urology Resident at the University of Minnesota Hospital. In this podcast she discusses the following BJUI Article of the Week:
Retzius‐sparing robot‐assisted radical prostatectomy (RS‐RARP) vs standard RARP: it’s time for critical appraisal
Abstract
Since robot‐assisted radical prostatectomy (RARP) started to be regularly performed in 2001, the procedure has typically followed the original retropubic approach, with incremental technical improvements in an attempt to improve outcomes. These include the running Van‐Velthoven anastomosis, posterior reconstruction or ‘Rocco stitch’, and cold ligation of the Santorini plexus/dorsal vein to maximise urethral length. In 2010, Bocciardi’s team in Milan proposed a novel posterior or ‘Retzius‐sparing’ RARP (RS‐RARP), mirroring the classic open perineal approach. This allows avoidance of supporting structures, such as the puboprostatic ligaments, endopelvic fascia, and Santorini plexus, preserving the normal anatomy as much as possible and limiting damage that may contribute to improved postoperative continence and erectile function. There has been much heralding of the excellent functional outcomes in both the medical and the lay press, but as yet no focus or real mention of any potential downsides of this new technique.
Article of the Month: Use of machine learning to predict early biochemical recurrence after robot‐assisted prostatectomy
Every month, the Editor-in-Chief selects an Article of the Month from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
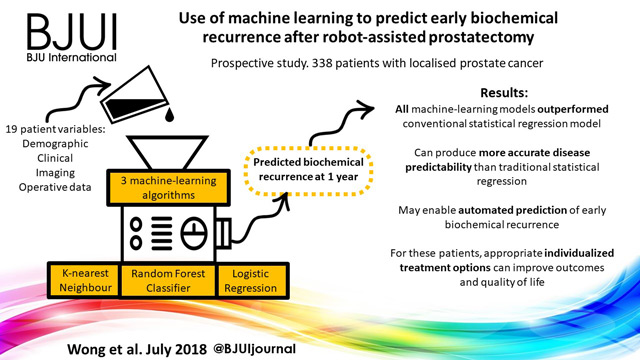
Use of machine learning to predict early biochemical recurrence after robot‐assisted prostatectomy
Nathan C. Wong , Cameron Lam, Lisa Patterson and Bobby Shayegan
Division of Urology, Department of Surgery, McMaster University, Hamilton, ON, Canada
Abstract
Objectives
To train and compare machine‐learning algorithms with traditional regression analysis for the prediction of early biochemical recurrence after robot‐assisted prostatectomy.
Patients and Methods
A prospectively collected dataset of 338 patients who underwent robot‐assisted prostatectomy for localized prostate cancer was examined. We used three supervised machine‐learning algorithms and 19 different training variables (demographic, clinical, imaging and operative data) in a hypothesis‐free manner to build models that could predict patients with biochemical recurrence at 1 year. We also performed traditional Cox regression analysis for comparison.
Results
K‐nearest neighbour, logistic regression and random forest classifier were used as machine‐learning models. Classic Cox regression analysis had an area under the curve (AUC) of 0.865 for the prediction of biochemical recurrence. All three of our machine‐learning models (K‐nearest neighbour (AUC 0.903), random forest tree (AUC 0.924) and logistic regression (AUC 0.940) outperformed the conventional statistical regression model. Accuracy prediction scores for K‐nearest neighbour, random forest tree and logistic regression were 0.976, 0.953 and 0.976, respectively.
Conclusions
Machine‐learning techniques can produce accurate disease predictability better that traditional statistical regression. These tools may prove clinically useful for the automated prediction of patients who develop early biochemical recurrence after robot‐assisted prostatectomy. For these patients, appropriate individualized treatment options can improve outcomes and quality of life.
Editorial: Can machine‐learning algorithms replace conventional statistics?
Wong et al. [1] evaluate 19 clinical variables (training data) and three supervised machine‐learning algorithms to predict early biochemical recurrence after robot‐assisted prostatectomy. They further compare the areas under the curve (AUCs) resulting from these algorithms with the AUC of a conventional Cox regression model and conclude that the machine‐learning algorithms can produce accurate disease prognosis, perhaps better than a traditional Cox regression model. As the authors state, predictive models have the potential to better individualize care to patients at highest risk of prostate cancer recurrence and progression.
The authors should be commended for their adoption of machine‐learning algorithms to better interpret the vast volumes of clinical data and assess prognosis after robot‐assisted prostatectomy. This should represent another step forward for the management of prostate cancer, where tailored treatment is now largely based on the clinical risk stratification of the disease [2]. Incidentally, we are also in an era where we are seeing aspects of artificial intelligence (machine learning being a subset of it) vastly transform how we view and process data in everyday life. This has been true in medicine as well, particularly for prostate cancer [3].
While our own research group has also evaluated machine‐learning algorithms to process surgeon performance metrics and predict clinical outcomes after robot‐assisted prostatectomy [4], I want to express a word of caution. Utilization of machine learning does not in itself imply automatic superiority over conventional statistics [5] despite literature that has demonstrated so [3]. The success of predictive models in machine learning still relies on the quality of data introduced and careful execution of the analysis. In our experience, it works best when highly experienced clinicians and data scientists are working hand in hand.
Furthermore, I would argue that the results of this present study do not necessarily show that machine learning is superior to conventional statistics, but rather it highlights an inherent advantage of machine learning. While traditional analyses require the a priori selection of a model based on the available data, machine learning has more flexibility for model fitting [6]. Additionally, inclusion of variables in traditional analyses is constrained by the sample size. In contrast, by design, machine learning models thrive on their ability to consider many variables concurrently, and as such, have the potential to detect underlying patterns that may otherwise be undetectable when data are examined effectively in individual silos.
We look forward to the external validation of the methodology described in the present article. Big and diverse data are critical requirements of machine learning. A multi‐institutional, multi‐surgeon cohort is necessary to confirm the findings in this report. A further step from there is the adoption of such prediction models into clinical use. The ultimate question is how improved prognostic data may influence surgeon and patient decisions.
Conflict of Interest
Dr Hung reports personal fees from Ethicon, Inc, outside the submitted work.
References
- Wong NC, Lam C, Patterson L, Shayegan B. Use of machine learning to predict early biochemical recurrence following robotic prostatectomy. BJU Int 2019; 123: 51–7
- D’Amico AV, Whittington R, Malkowicz SB et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy or interstitial radiation therapy for clinically localized prostate cancer. JAMA 1998; 280: 969–74
-
Potter SR, Miller MC, Mangold LA et al. Genetically engineered neural networks for predicting prostate cancer progression after radical prostatectomy. Urology 1999; 54: 791–5
- Hung AJ, Chen J, Che Z et al. Utilizing machine learning and automated performance metrics to evaluate robot‐assisted radical prostatectomy performance and predict outcomes. J Endourol 2018; 32: 438–445
- Kattan MW. Comparison of Cox regression with other methods for determining prediction models and nomograms. J Urol 2003; 170 (6 Pt 2): S6–9
- Hung AJ, Chen J, Gill IS. Automated performance metrics and machine learning algorithms to measure surgeon performance and anticipate clinical outcomes in robotic surgery. JAMA Surg 2018; 153: 770–1
Residents’ Podcast: Pelvic Drain Placement After Robot-Assisted Radical Prostatectomy
Department of Urology, Dalhousie University, Halifax, NS, Canada
Abstract
Objective
To determine if eliminating the prophylactic placement of a pelvic drain (PD) after robot-assisted radical prostatectomy (RARP) affects the incidence of early (90-day) postoperative adverse events.
Patients and Methods
In this parallel-group, blinded, non-inferiority trial, we randomised patients planning to undergo RARP to one of two arms: no drain placement (ND) or PD placement. Patients with demonstrable intraoperative leakage upon bladder irrigation were excluded. Randomisation sequence was determined a priori using a computer algorithm, and included a stratified design with respect to low vs intermediate/high D’Amico risk classifications. Surgeons remained blinded to the randomisation arm until final eligibility was verified at the end of the RARP. The primary endpoint was overall incidence of 90-day complications which, based on our standard treatment using PD retrospectively, was estimated at 13%. The non-inferiority margin was set at 10%, and the planned sample size was 312. An interim analysis was planned and conducted when one-third of the planned accrual and follow-up was completed, to rule out futility if the delta margin was in excess of 0.1389.
Results
From 2012 to 2016, 189 patients were accrued to the study, with 92 patients allocated to the ND group and 97 to the PD group. Due to lower than expected accrual rates, accrual to the study was halted by regulatory entities, and we did not reach the intended accrual goal. The ND and PD groups were comparable for median PSA level (6.2 vs 5.8 ng/mL, P = 0.5), clinical stage (P = 0.8), D’Amico risk classification (P = 0.4), median lymph nodes dissected (17 vs 18, P = 0.2), and proportion of patients receiving an extended pelvic lymph node dissection (70.7% vs 79.4%, P = 0.3). Incidence of 90-day overall and major (Clavien–Dindo grade >III) complications in the ND group (17.4% and 5.4%, respectively) was not inferior to the PD group (26.8% and 5.2%, respectively; P < 0.001 and P = 0.007 for difference of proportions <10%, respectively). Symptomatic lymphocoele rates (2.2% in the ND group, 4.1% in the PD group) were comparable between the two arms (P = 0.7).
Conclusions
Incidence of adverse events in the ND group was not inferior to the group who received a PD. In properly selected patients, PD placement after RARP can be safely withheld without significant additional morbidity.
BJUI Podcasts now available on iTunes, subscribe here https://itunes.apple.com/gb/podcast/bju-international/id1309570262
Article of the month: The race to urinary continence after RP
Every week the Editor-in-Chief selects the Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by prominent members of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
Finally, the third post under the Article of the Week heading on the homepage will consist of additional material or media. This week we feature a video of Inge Geraerts discussing functional outcomes after ORP and RARP.
If you only have time to read one article this week, it should be this one.
Prospective evaluation of urinary incontinence, voiding symptoms and quality of life after open and robot-assisted radical prostatectomy
Inge Geraerts*, Hendrik Van Poppel†, Nele Devoogdt*‡, Ben Van Cleynenbreugel†, Steven Joniau† and Marijke Van Kampen*‡
Departments of *Rehabilitation Science, †Urology and ‡Physical Medicine and Rehabilitation, UZ Leuven, Leuven, Belgium
OBJECTIVE
• To compare functional outcomes, i.e. urinary incontinence (UI), voiding symptoms and quality of life, after open (ORP) and robot-assisted radical prostatectomy (RARP).
PATIENTS AND METHODS
• Between September 2009 and July 2011, 180 consecutive patients underwent radical prostatectomy; of these, 116 underwent ORP and 64 underwent RARP. We prospectively assessed the functional outcomes of each group during the first year of follow-up.
• We measured UI on the 3 days before surgery (24-h pad test) and daily after surgery until total continence, defined as 3 consecutive days of 0 g urine leak, was achieved. Additionally, all patients were assessed before surgery and at 1, 3, 6 and 12 months after surgery using the International Prostate Symptom Score (IPSS) and the King’s Health Questionnaire (KHQ).
• All patients received pelvic floor muscle training until continence was achieved.
• Kaplan–Meier analyses and Cox regression with correction for covariates were used to compare time to continence. A Mann–Whitney U-test was used to assess IPSS and KHQ.
RESULTS
• Patients in the RARP group had a significantly lower D’Amico risk group allocation and underwent more nerve-sparing surgery. Other characteristics were similar.
• Patients in the RARP group regained continence sooner than those in the ORP group (P = 0.007). In the RARP group, the median time to continence (16 vs 46 days, P = 0.026) was significantly shorter and the median amount of first day UI (44 vs 186 g, P < 0.01) was significantly smaller than in the ORP group. After correction for all covariates, the difference remained significant (P = 0.036, hazard ratio [HR] 1.522 (1.027–2.255). In addition, younger men, men with positive surgical margins and men without preoperative incontinence achieved continence sooner.
• A comparison of time to continence between groups with a sufficient number of patients (intermediate risk and/or bilateral nerve-sparing) still showed a faster return of continence after RARP, but the effect decreased in size and was nonsignificant (HR>1.2, P> 0.05).
• Only six patients (two in the RARP and four in the ORP group) still had UI after 1 year.• Patients in the RARP group had significantly better IPSS scores at 1 (P = 0.013) and 3 (P = 0.038) months, and scored better in almost all KHQ aspects.
CONCLUSION
• In this prospective trial, patients treated with RARP tended to regain urinary continence sooner than patients treated with ORP, but in subgroup analyses statistical significance disappeared and effect size decreased dramatically, indicating that the results must be interpreted with caution.
Read Previous Articles of the Week