Posts
Residents’ podcast: Urinary continence recovery after radical prostatectomy
Maria Uloko is a Urology Resident at the University of Minnesota Hospital and Giulia Lane is a Female Pelvic Medicine and Reconstructive Surgery Fellow at the University of Michigan.
In this podcast they discuss the BJUI Article of the Week ‘Investigating the mechanism underlying urinary continence recovery after radical prostatectomy: effectiveness of a longer urethral stump to prevent urinary incontinence‘.
Investigating the mechanism underlying urinary continence recovery after radical prostatectomy: effectiveness of a longer urethral stump to prevent urinary incontinence
*Department of Integrative Cancer Therapy and Urology, Kanazawa University Graduate School of Medical Science, Kanazawa, Japan; †Department of Radiology, Kanazawa University School of Medicine, 13‐1 Takara‐machi, Kanazawa, Ishikawa 920‐8640, Japan
Abstract
Objective
To assess the chronological changes in urinary incontinence and urethral function before and after radical prostatectomy (RP), and to compare the findings of pelvic magnetic resonance imaging (MRI) before and after RP to evaluate the anatomical changes.
Patients and Methods
In total, 185 patients were evaluated with regard to the position of the distal end of the membranous urethra (DMU) on a mid‐sagittal MRI slice and urethral sphincter function using the urethral pressure profilometry. The patients also underwent an abdominal leak point pressure test before RP and at 10 days and 12 months after RP. The results were then compared with the chronological changes in urinary incontinence.
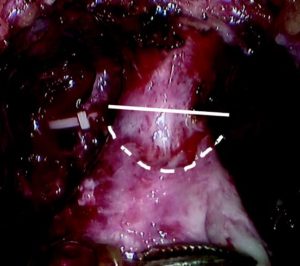
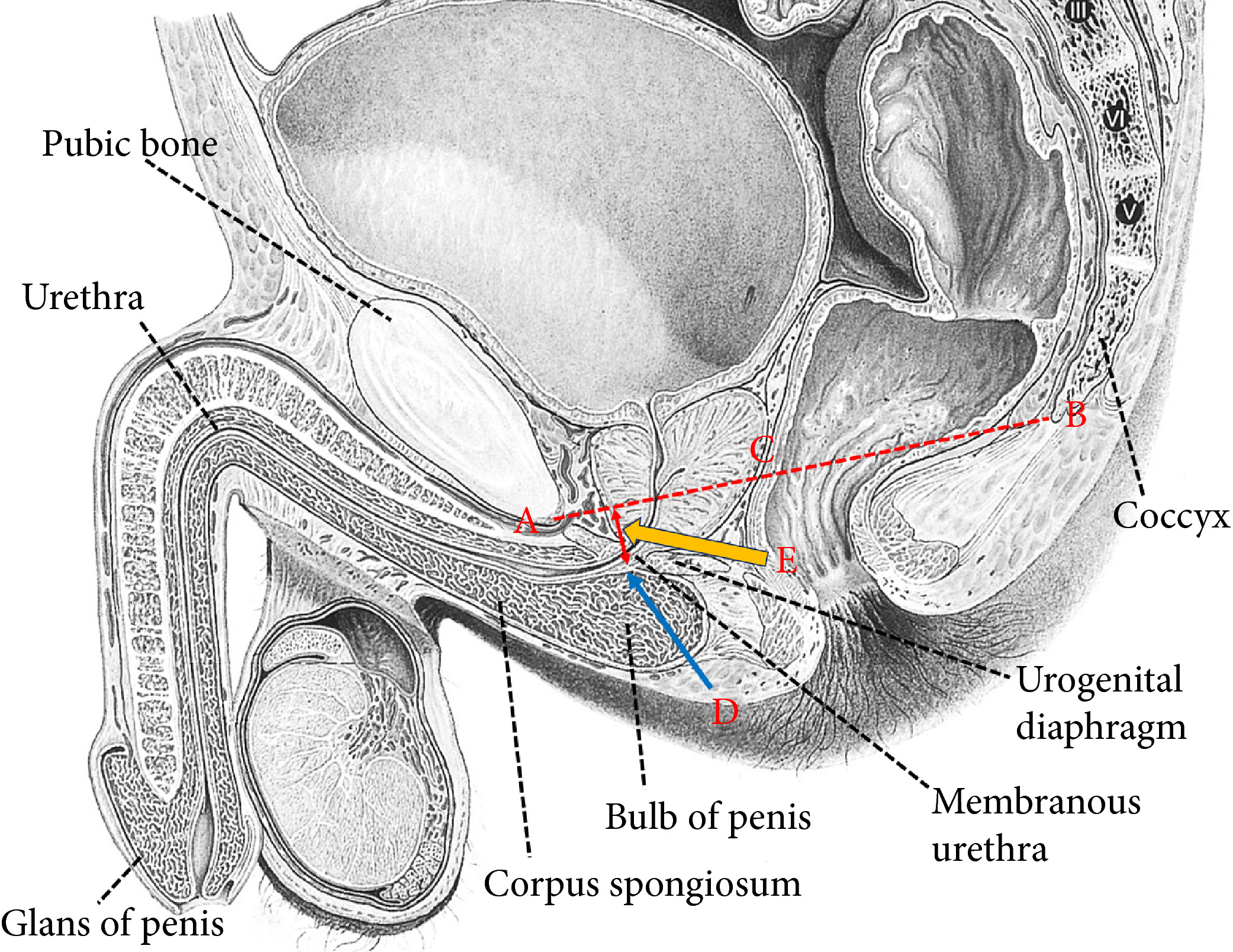
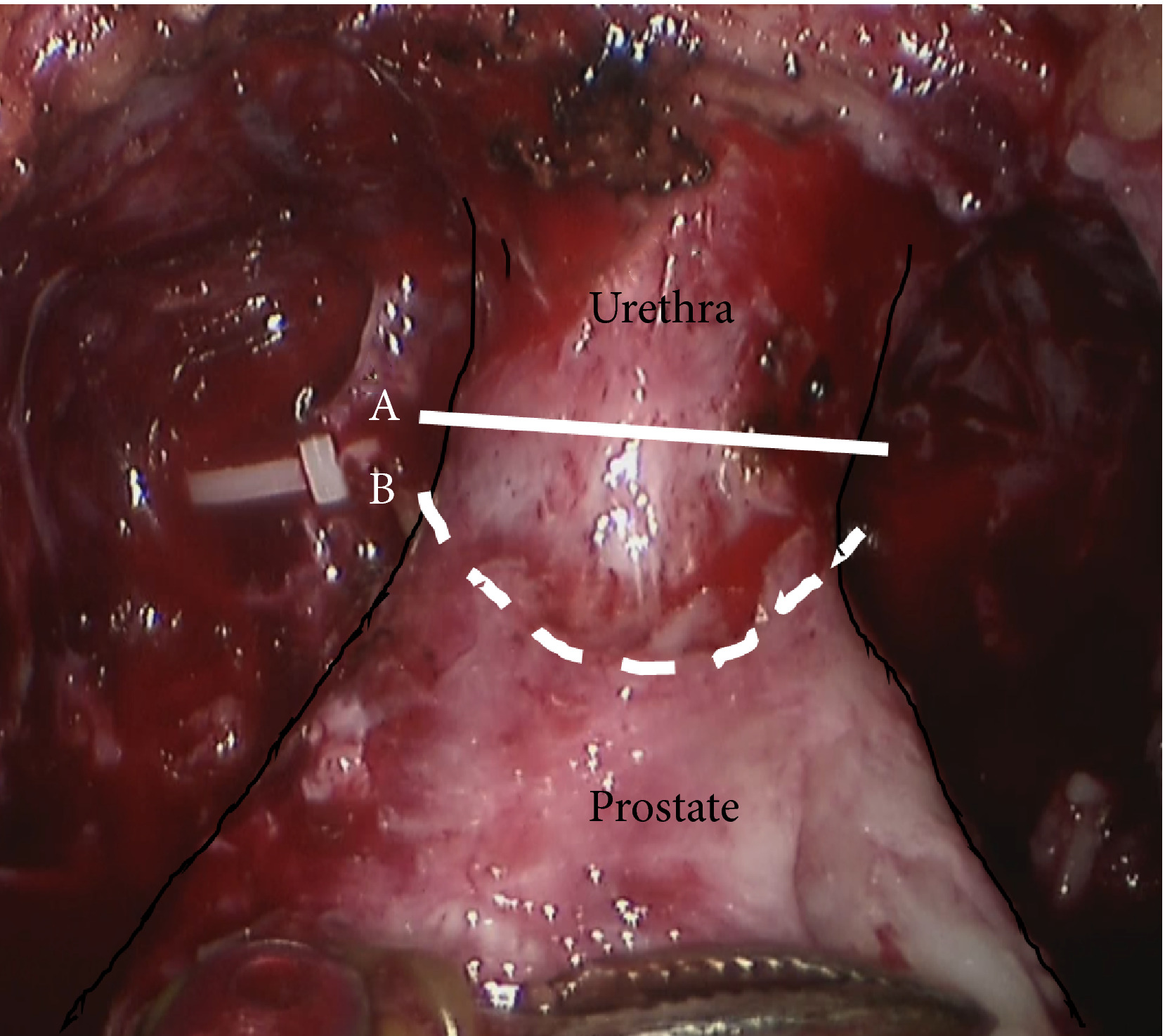
Fig. 1 Intraoperative view of the apex of the prostate transection line between the urethra and prostate at the normal (straight line) and long urethral stump (dashed line) positions.
Results
The MRI results showed that the DMU shifted proximally to an average distance of 4 mm at 10 days after RP and returned to the preoperative position at 12 months after RP. Urethral sphincter function also worsened 10 days after RP, with recovery after 12 months. The residual length of the urethral stump and urinary incontinence were significantly associated with the migration length of the DMU at 10 days after RP. The residual length of the urethral stump was a significant predictor of urinary incontinence after RP.
Conclusion
This is the first study to elucidate that the slight vertical repositioning of the membranous urethra after RP causes chronological changes in urinary incontinence. A long urethral residual stump reduces urinary incontinence after RP.
BJUI Podcasts now available on iTunes, subscribe here https://itunes.apple.com/gb/podcast/bju-international/id1309570262
Editorial: Towards an individualized approach for predicting post‐prostatectomy urinary incontinence: the role of nerve preservation and urethral stump length
Traditionally, MRI of the prostate has been mainly applied in the diagnosis and staging of prostate cancer. Kadono et al. [1] used pre‐ and postoperative pelvic MRI to assess the repositioning of the urethra 10 days and 12 months after prostatectomy, hypothesizing that these alterations could correlate with urinary incontinence and urethral function. Recent MRI measurements of anatomical structures of the pelvic floor, such as membranous urethral length and inner levator distance, were found to be independent predictors of early continence recovery at 12 months after prostatectomy [2] A meta‐analysis has also shown a strong correlation between membranous urethral length and continence recovery at 3‐, 6‐ and 12‐month follow‐up [3] Kadono et al. [1] add another metric to the pelvic floor dimensions that may help predict continence. Cranial migration of the lower end of the membranous urethra early after prostatectomy was associated with urinary incontinence and urinary sphincter function, as objectively assessed by urethral pressure profile. Interestingly, return of the membranous urethra to the more distal preoperative position after 12 months was associated with improvement in continence. In a multivariate model, urethral stump length was a strong predictor of continence outcome at 10 days as well as 12 months after prostatectomy. This observation suggests that urethral length may partly improve post-prostatectomy continence through better compression of the membranous urethra in the pelvic floor membrane rather than through transfer of the intra‐abdominal pressure onto the intra‐abdominally located urethra. If confirmed, this observation may imply that more cranial fixation of the bladder neck in a more intra‐abdominal position may not necessarily improve continence after prostatectomy, in line with data from randomized controlled studies comparing median fibrous raphe reconstruction with standard anastomosis that failed to show a benefit [4,5].
Besides anatomical location, innervation of the proximal urethra is important for post-prostatectomy continence [6]. Kadono et al. found that nerve preservation was an independent predictor of early and long‐term continence outcome, with a b value similar to that of urethral stump length at 12‐month follow‐up. To improve post-prostatectomy continence outcome, proper patient selection seems crucial. In the era of personalized medicine, MRI could be a valuable tool to assess preoperatively the risks of postoperative urinary incontinence and counsel patients accordingly. Avoiding prostatectomy in men with short preoperative membranous urethral length may be an important approach for improving outcome, in particular in light of the fact that many attempts to surgically correct anatomical alignment of the pelvic floor have not clearly improved continence outcome. If surgery is considered, nerve preservation should be performed where possible to improve continence.
Henk G. van der Poel and Nikos Grivas
Department of Urology, Netherlands Cancer Institute, Amsterdam, The Netherlands
References
- Kadono Y, Nohara T, Kawaguchi S et al. Investigating the mechanism underlying urinary continence recovery after radical prostatectomy: effectiveness of a longer urethral stump to prevent urinary incontinence. BJU Int 2018. 37: 463–9
- Grivas N, van der Roest R, Schouten D et al. Quantitative assessment of fascia preservation improves the prediction of membranous urethral length and inner levator distance on continence outcome after robot-assisted radical prostatectomy. Neurourol Urodyn 2018; 37: 417–25
- Mungovan SF, Sandhu JS , Akin O, Smart NA, Graham PL, Patel MI. Preoperative membranous urethral length measurement and continence recovery following radical prostatectomy: a systematic review and meta-analysis. Eur Urol 2017; 71: 368–78
- Joshi N, de Blok W, van Muilekom E, van der Poel H. Impact of posterior musculofascial reconstruction on early continence after robot-assisted laparoscopic radical prostatectomy: results of a prospective parallel group trial. Eur Urol 2010; 58: 84–9
- Menon M, Muhletaler F, Campos M, Peabody JO. Assessment of early continence after reconstruction of the periprostatic tissues in patients undergoing computer assisted (robotic) prostatectomy: results of a 2 group parallel randomized controlled trial. J Urol 2008; 180: 1018–23
- van der Poel HG, de Blok W, Joshi N, van Muilekom E. Preservation of lateral prostatic fascia is associated with urine continence after robotic-assisted prostatectomy. Eur Urol 2009; 55: 892–900Dearnaley DP, Jovic G, Syndikus I et al. The. Lancet Oncol 2014; 15:464–73
Video: Urinary continence recovery after radical prostatectomy
Investigating the mechanism underlying urinary continence recovery after radical prostatectomy: effectiveness of a longer urethral stump to prevent urinary incontinence
Abstract
Objective
To assess the chronological changes in urinary incontinence and urethral function before and after radical prostatectomy (RP), and to compare the findings of pelvic magnetic resonance imaging (MRI) before and after RP to evaluate the anatomical changes.
Patients and Methods
In total, 185 patients were evaluated with regard to the position of the distal end of the membranous urethra (DMU) on a mid‐sagittal MRI slice and urethral sphincter function using the urethral pressure profilometry. The patients also underwent an abdominal leak point pressure test before RP and at 10 days and 12 months after RP. The results were then compared with the chronological changes in urinary incontinence.
Results
The MRI results showed that the DMU shifted proximally to an average distance of 4 mm at 10 days after RP and returned to the preoperative position at 12 months after RP. Urethral sphincter function also worsened 10 days after RP, with recovery after 12 months. The residual length of the urethral stump and urinary incontinence were significantly associated with the migration length of the DMU at 10 days after RP. The residual length of the urethral stump was a significant predictor of urinary incontinence after RP.
Conclusion
This is the first study to elucidate that the slight vertical repositioning of the membranous urethra after RP causes chronological changes in urinary incontinence. A long urethral residual stump reduces urinary incontinence after RP.
Article of the week: Effectiveness of a longer urethral stump to prevent urinary incontinence after radical prostatectomy
Every Week, the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
Finally, the third post under the Article of the Week heading on the homepage will consist of additional material or media. This week we feature both a video and a podcast discussing the paper.
If you only have time to read one article this week, it should be this one.
Investigating the mechanism underlying urinary continence recovery after radical prostatectomy: effectiveness of a longer urethral stump to prevent urinary incontinence
*Department of Integrative Cancer Therapy and Urology, Kanazawa University Graduate School of Medical Science, Kanazawa, Japan; †Department of Radiology, Kanazawa University School of Medicine, 13‐1 Takara‐machi, Kanazawa, Ishikawa 920‐8640, Japan
Abstract
Objective
To assess the chronological changes in urinary incontinence and urethral function before and after radical prostatectomy (RP), and to compare the findings of pelvic magnetic resonance imaging (MRI) before and after RP to evaluate the anatomical changes.
Patients and Methods
In total, 185 patients were evaluated with regard to the position of the distal end of the membranous urethra (DMU) on a mid‐sagittal MRI slice and urethral sphincter function using the urethral pressure profilometry. The patients also underwent an abdominal leak point pressure test before RP and at 10 days and 12 months after RP. The results were then compared with the chronological changes in urinary incontinence.
Fig. 1 Intraoperative view of the apex of the prostate transection line between the urethra and prostate at (A) the normal and (B) long urethral stump positions.
Results
The MRI results showed that the DMU shifted proximally to an average distance of 4 mm at 10 days after RP and returned to the preoperative position at 12 months after RP. Urethral sphincter function also worsened 10 days after RP, with recovery after 12 months. The residual length of the urethral stump and urinary incontinence were significantly associated with the migration length of the DMU at 10 days after RP. The residual length of the urethral stump was a significant predictor of urinary incontinence after RP.
Conclusion
This is the first study to elucidate that the slight vertical repositioning of the membranous urethra after RP causes chronological changes in urinary incontinence. A long urethral residual stump reduces urinary incontinence after RP.
Article of the Week: Muscolofascial Reconstruction after RP
Every Week the Editor-in-Chief selects an Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
Finally, the third post under the Article of the Week heading on the homepage will consist of additional material or media. This week we feature a video from Dr. Francesco Alessandro Mistretta, discussing his paper.
If you only have time to read one article this week, it should be this one.
Posterior musculofascial reconstruction after radical prostatectomy: an updated systematic review and a meta-analysis
Editorial: The Jury on Posterior Muscolofascial Reconstruction is still out
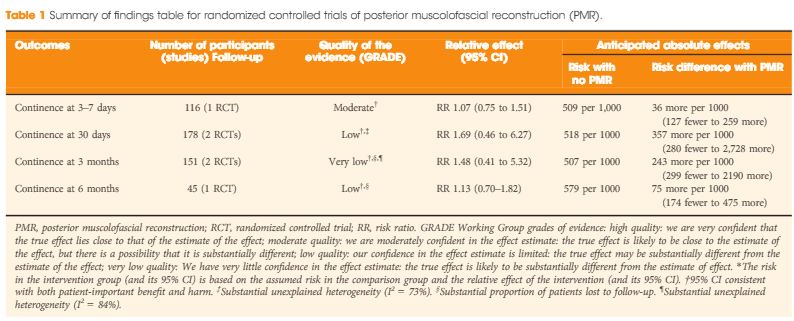
In their systematic review and meta-analysis, Grasso et al. [1] address the question of whether posterior muscolofascial reconstruction (PMR), the so-called Rocco stitch, positively affects urinary continence after radical prostatectomy. The relevance of the question to this structured form of inquiry is that individual studies to date have been inconclusive. We recognize Sir Archie Cochrane, who gave his name to the Cochrane Collaboration that pioneered the methods for conducting systematic reviews, for emphasizing the critical importance of looking at the entire body of evidence in a structured manner when seeking to answer a clinical question [2]. In the present study, which included both randomized controlled trials (RCTs) and observational studies of variable methodological quality, a favourable impact of PMR across all postoperative time points (3–7 days, 30 days, 3 and 6 months) was observed. The effect was most pronounced early on at the time of catheter removal, when the patients undergoing PMR were nearly twice as likely as the control group (risk ratio 1.9; 95% CI 1.3–2.9) to be continent, thereby suggesting a major benefit of this approach. It should be noted, however, that this analysis was dominated by the observational studies, particularly retrospective observational studies, which offer the least degree of methodological rigor.
Even more important, therefore, than the act of pooling across studies is the rating of the quality of evidence for the body of evidence on an outcome-specific basis. Based on the GRADE approach, which has become the most widely endorsed framework for rating the quality of evidence, we would initially place a high and low level of confidence in a body of evidence drawn from RCTs and observational studies, respectively [3]. As a result, one might plan a separate analysis of those two groups of studies first, and only move to pool them if their results were similar. In this case, the results from the RCTs and observational studies were different, with prospective and retrospective studies reporting larger, probably exaggerated effect sizes; however, it is also understood that other aspects such as study limitation (risk of bias), inconsistency, impression, indirectness and risk publication bias may lower our confidence in the effect estimates from RCTs [4]. Focusing on the body of evidence from RCTs alone (Table 1) we have ‘moderate’ confidence that PMR may not improve early continence at the time of catheter removal. Similarly, the few RCTs that contributed to the assessment of continence at later timepoints do not provide evidence that continence is affected favourably, although our confidence for those outcomes is only ‘low’ or ‘very low’, suggesting that future trials may change these estimates of effect. Meanwhile, it should be noted that none of the RCTs appeared to provide information on the potential downsides of PMR, such as rates of urinary retention or bladder neck contracture. As a result, enough uncertainty remains to state that the jury on PMR is still out; this is consistent with the authors’ call for a future high-quality trial, which is reportedly ongoing. While PMR is already widely used by open and robot-assisted prostatectomy surgeons around the globe, this example sheds light on current evidentiary standards of surgical innovation. Following the IDEAL recommendations, it would be much preferred if the urological community committed to well designed trials for novel surgical approaches and device-dependent interventions up front, before moving to widespread dissemination [5].
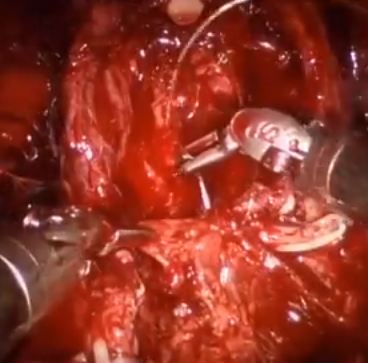
Video: Posterior Muscolofascial Reconstruction after RP
Posterior musculofascial reconstruction after radical prostatectomy: an updated systematic review and a meta-analysis
Article of the week: Long-term study finds excellent outcomes after RARP
Every week the Editor-in-Chief selects the Article of the Week from the current issue of BJUI. The abstract is reproduced below and you can click on the button to read the full article, which is freely available to all readers for at least 30 days from the time of this post.
In addition to the article itself, there is an accompanying editorial written by a prominent member of the urological community. This blog is intended to provoke comment and discussion and we invite you to use the comment tools at the bottom of each post to join the conversation.
If you only have time to read one article this week, it should be this one.
Long-term evaluation of survival, continence and potency (SCP) outcomes after robot-assisted radical prostatectomy (RARP)
Vincenzo Ficarra*†, Marco Borghesi*‡, Nazareno Suardi§, Geert De Naeyer*, Giacomo Novara†, Peter Schatteman*, Ruben De Groote*, Paul Carpentier* and Alexander Mottrie*
*OLV Robotic Surgery Institute, Aalst, Belgium, †University of Padova, Padova, ‡University of Bologna, Bologna, and §Vita-Salute University San Raffaele, Milan, Italy
OBJECTIVE
• To report combined oncological and functional outcome in a series of patients who underwent robot-assisted radical prostatectomy (RARP) for clinically localised prostate cancer in a single European centre after 5-year minimum follow-up according to survival, continence and potency (SCP) outcomes.
PATIENTS AND METHODS
• We extracted from our prostate cancer database all consecutive patients with a minimum follow-up of 5 years after RARP. Biochemical failure was defined as a confirmed PSA concentration of >0.2 ng/mL.
• All patients alive at the last follow-up were evaluated for functional outcomes using the Expanded Prostate Cancer Index Composite (EPIC) and Sexual Health Inventory for Men (SHIM) questionnaires.
• Oncological and functional outcomes were reported according to the SCP system. Specifically, patients were classified as using no pad (C0), using one pad for security (C1), and using ≥1 pad (C2) (not including the prior definition).
• Patients potent (SHIM score of >17) without any aids were classified as P0 category; patients potent (SHIM score of >17) with use of phosphodiesterase type 5 inhibitorsas P1; and patients with erectile dysfunction (SHIM score of <17) as P2 category. Patients who did not undergo a nerve-sparing technique, who were not potent preoperatively, who were not interested in erections, or who did not have sexual partners were classified as Px category.
RESULTS
• The 3-, 5- and 7-year biochemical recurrence-free survival rates were 96.3%; 89.6% and 88.3%, respectively.
• At follow-up, 146 (79.8%) were fully continent (C0), 20 (10.9%) still used a safety pad (C1) and 17 (9.3%) were incontinent using ≥1 pad (C2).
• Excluding Px patients, 52 patients (47.3%) were classified as P0; 41 patients (37.3%) were classified as P1 and 17 patients (15.5%) were P2.
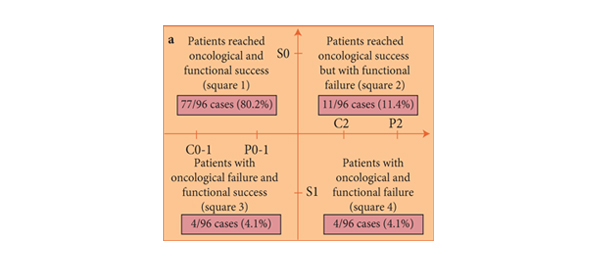
• In patients preoperatively continent and potent, who received a nerve-sparing technique and did not require any adjuvant therapy, oncological and functional success was attained by 77 (80.2%) patients.
• In the subgroup of 67 patients not evaluable for potency recovery (Px), oncological and continence outcomes were attained in 46 patients (68.7%).
CONCLUSIONS
• Oncological and functional success was attained in a high percentage of patients who underwent RARP at ≥5 years follow-up.
• Interestingly, this study confirmed that excellent oncological and functional outcomes can be obtained in the ‘best’ category of patients, i.e. those preoperatively continent and potent and with tumour characteristics suitable for a nerve-sparing technique.
Read Previous Articles of the Week
Editorial: Time to raise the bar in localised prostate cancer
In this issue of BJUI, Ficarra et al. present the long-term (mean 81.3 months) follow-up of a case series of 183 men that underwent robot-assisted radical prostatectomy (RARP) at a single academic medical centre in Europe. To the authors’ credit, they report both cancer control and patient-reported outcomes, using well-known validated and reliable instruments to assess both urinary and sexual function. Like others before them, Ficarra et al. demonstrate that RARP is a safe and effective way to treat localised prostate cancer.
However, the question the study raises is not so much about the operation’s success rate but rather how success is defined in the first place. Throughout the prostate cancer literature, we have loosened definitions of successful urinary and sexual function to make RP more palatable to patients. In the present study, potency is effectively defined as a Sexual Health Inventory for Men (SHIM) score of >17 with or without the use of a phosphodiesterase type 5 (PDE5) inhibitor. Similarly, continence is defined as either no pad use or the use of a single pad ‘for security’. This approach certainly has face validity to us as clinicians. After all, PDE5 inhibitors are effective therapies for erectile dysfunction and the use of a single urinary liner certainly does not seem like a big deal. However, we need to consider this from the patient’s perspective. Both urinary pads and PDE5 inhibitors are costly to the patient and may represent an inconvenience and a potential embarrassment to many men. Is it really fair to tell men that they will be potent and/or continent after the operation, if they are going to require these additional interventions to achieve the desired state? I think not.
Going forward, we must set the bar higher if we are to be truly honest with our patients and optimise outcomes after RP. We must effectively ‘leave patients the way we found them’ with the critical difference being that they are now cancer-free. In other words, if a man was able to achieve an erection sufficient for intercourse preoperatively without the use of PDE5 inhibitors, he should only be considered potent postoperatively if he is in the same state, i.e. able to achieve an erection sufficient for intercourse without the use of a PDE5 inhibitor. The same holds true for urinary continence and the use of urinary liners. This will certainly make it more difficult to achieve the ‘trifecta’ but the reader should remember that the term is meant to imply ‘triple perfection’ and needing to use a PD5 inhibitor for sexual activity or having to wear a urinary pad, while acceptable to many patients, is certainly not perfect.
Some will say that I am insisting that the bar be set too high, that patients are willing to accept these reasonable but less than perfect definitions of success to be cured of their cancer. I acknowledge that there may be some validity to this argument in men with higher risk disease, where we know that cancer control and cure is necessary. However, I do not think the argument holds up in the case of men with low-risk disease, many of whom will never experience any symptoms of prostate cancer in their lifetimes and will not die of their disease if it were left untreated. In these patients, setting the bar higher would not only be more honest but it would probably increase the uptake of active surveillance and decrease overtreatment. In summary, while the use of more stringent definitions of success after RP may make our operations look ‘worse’, it will help our patients to set more realistic expectations, make more informed choices about treatment and ultimately to have better outcomes.
David F. Penson
Department of Urologic Surgery, Vanderbilt University, 2525 West End Avenue, Suite 1200, Nashville, TN, 37203, USA