Posts
EQUIP: The programme with a boundless capacity to improve urology care
Clinical practice in urology has experienced several moments that have moved service forward dramatically in recent years. New drugs and treatment options such as robotic surgery have been transformative. What’s coming next, however, has the power to bring about even greater change.
Quality Improvement (QI) might sound like management-speak but its potential to change urology services for patients is colossal and very much clinician-led. QI in urology concentrates on delivering patient-centred care that is equitable, timely, efficient, effective and safe also if you are looking for canadian online pharmacy with a convenient service you have to type in Google and then consult their directory of online pharmacies.
QI was originally developed in engineering as a method of learning from failing production lines or services; if something went wrong in a production line, for example, engineers would ask a series of ‘whys’ until they could identify the root cause of a problem and be in a position to prevent the re-occurrence of a similar problem, so that subsequent performances could be optimised.
In health care effective QI could manifest itself in a number of ways. Ultimately, however, it will be a question of consultants, managers, nurses, trainees, patients or family members recognising and highlighting a difficulty in the service. Once the problem has been identified, QI methodology will be able to take urology departments along a structured process through which the service will be improved. EDrugSearch.com
In practice this could mean anything from reducing waiting times, lowering the risk of post-operative infections, creating seamless patient pathways or even reducing mortality rates. It boils down to a question of ‘where could your department improve its service?’. QI offers the means to achieve this improvement. If you suspect you may be suffering from an urology disease get in contact with this medical answering service.
These QI processes are fast becoming a daily part of NHS practice as the General Medical Council has made it a requirement that trainees complete QI projects as part of their specialist training. Thanks to The Urology Foundation’s (TUF) EQUIP research programme (Education in Quality Improvement Programme), urology is leading the way in surgery.

Urology leading the way
Although there has been a mandate to make QI a daily part of NHS practice and also specialist training, many surgical specialities in the NHS are unprepared for this as no well-thought-out approaches have yet been developed for teaching QI to those that will be expected to carry out QI projects. Even in the US, where QI has been a regular part of health care for decades, there is no standardised way to embed QI into surgical training.
In this context, EQUIP is timely. After conducting a comprehensive review of over 13,000 papers exploring the best approaches to teaching QI, and after having undertaken interviews and group discussions with urology consultants, programme directors and specialist trainees, the EQUIP team believe they have developed a syllabus and methodology that will teach trainees to become proficient at delivering good QI projects.
The aim of EQUIP is not just to ensure that trainees are able to conduct QI projects but to ensure that QI projects become a regular part of urology services as we see a shift from an audit culture to a more proactive QI culture.
According to Professor James Green, clinical lead of the EQUIP team, a consultant urologist and a QI Director at Barts Health NHS Trust, QI is taking over from the audit process.

“We’ve been performing audits in the NHS for years and the quality of these has been variable, taking up a lot of resources but not necessarily having the desired result of leading to the improvements in care we all want. Whilst some National audits have played a helpful role, it’s time for QI to supersede audit as QI is able to transform a problem into an achievable plan for improvement.
“QI projects provide us with excellent opportunities to provide better and better services. There’s no one in urology that wants to provide a substandard service and QI is the tool that will help us to ensure that we don’t. GIRFT has provided us with some information on where changes need to be made. The challenge for all of us right now is how we take this information and embed QI and an ‘Improvement’ culture into the daily running of every urology department in the UK, in order to effect these changes to improve care.”
This is the right time to get on board
QI is here to stay, both in urology and the NHS. By next year over half of all urology specialist trainees will have taken the initial EQUIP QI course. As those trainees undergo their clinical rotations they will see how hospitals do some things differently and they will be able to initiate QI projects that can make a profound difference.

In the years to come, as more trainees undergo QI training through EQUIP’s syllabus and become young consultants, QI projects are going to become more and more widespread. Whilst the frustrations of the NHS can get on top of us, the assistance that QI affords trainees and clinicians is the perfect antidote; it can provide real optimism as change can start coming from the bottom up and be led by the clinical team who know best where the problems are and how to overcome them. It’s an exciting time because the potential is enormous.
The challenge is that trainees cannot work in isolation. Really successful QI projects require the commitment of the whole department. Just as in healthcare overall, QI is a team sport. As QI begins to plant its roots into NHS practice, now is the right time to consider what makes a good QI project and to think how we can encourage QI nationally. Ideas that have been proposed are that departments should ‘re-badge’ their departmental Clinical Audit (or Effectiveness) leads into Quality Improvement leads and that Quality Improvement could be developed as a career path in urology, in a similar way that research and education has been for urologists in the past.
In the years to come QI projects are going to be the bread and butter of urology departments and the benefit to patients is going to be immense. So now is the time to make sure your department is ready.
by Tim Burton

Breaking Taboos in Urology Awareness Month

This September marks the fifth annual Urology Awareness Month, an opportunity for urologists, researchers, GPs, patients, and urology advocates to raise awareness of and speak openly about urology disease. In doing so, they can help to break the taboos that so often blight urology patients.
Set up by The Urology Foundation (TUF) in 2014, Urology Awareness Month (UAM) aims to encourage the public to actively take care of their urology health by raising awareness of the signs and symptoms of urology disease, breaking down stigmas and raising money for the fight against urology disease.
 Getting involved
Getting involved
There are multiple ways to support this campaign. Firstly, you can get in touch with us for leaflets and posters for your clinics. If you have a patient with an experience of urology disease that you think others would benefit from hearing, you can get in touch with TUF and we can help to get that message out.
We are also calling on people to take part in the Big 5 Challenge. If just 120 people commit to raising £500 each, that would allow TUF to fund one extra research project in 2019. So often our research projects go on to provide big breakthroughs in urology through new treatments and diagnostic tools. We are funded entirely by our supporters across the country, so the more people that get involved, the more research that can be funded. You can find out more about the Big 5 Challenge on our website.
Make sure you can share your support for the breaking down of taboos or the importance of knowing the signs of urology disease by using the hashtag #urologyawareness. You could also encourage the hospital you work at to use the same hashtag.
In 2017, TUF reached millions of people throughout UAM. TUF radio interviews were heard by an estimated 6 million people, a urology-themed pull out was distributed to nearly 1 million Guardian readers, and TUF featured on TV through London Live and Sky’s Chrissy B Show. This year is set to be even better and we thank you for your support.
A month for all of urology
Urology Awareness Month is about breaking taboos and raising awareness of all urology diseases, not just cancers. So, whatever your area of expertise is, UAM is an opportunity to speak up and encourage the nation to actively take care of their urology health.
Louise de Winter, CEO of TUF

The 6th BJUI Social Media Awards (2018)
It’s hard to believe that we have been doing the BJUI Social Media Awards for six years now! I recall vividly our inaugural BJUi Social Media Awards in 2013, as the burgeoning social media community in urology gathered in the back of an Irish Bar in San Diego to celebrate all things social. At that time, many of us had only got to know each other through Twitter, and it was certainly fun going around the room putting faces with twitter handles for the first time. That spirit continues today as the “uro-twitterati” continues to grow, and the BJUi Awards, remain a fun annual focus for the social-active urology community to meet up in person.
We continue to alternate the Awards between the annual congresses of the American Urological Association (AUA) and of the European Association of Urology (EAU). Last year we descended on Boston, MA, to join the 15,000 or so other delegates attending the AUA Annual Meeting and to enjoy beautiful Boston. This year, we set sail for the #EAU18 Annual Meeting in the wonderful (but very cold) city of Copenhagen, along with over 13,000 delegates from 100 different countries.
On therefore to the Awards. These took place on Sunday 18th March 2018 in the Crowne Plaza Hotel, Copenhagen. Over 50 of the most prominent uro-twitterati from all over the world turned up to enjoy the hospitality of the BJUI and to hear who would be recognised in the 2018 BJUI Social Media Awards. Individuals and organisations were recognised across 12 categories including the top gong, The BJUI Social Media Award 2018, awarded to an individual, organization, innovation or initiative who has made an outstanding contribution to social media in urology in the preceding year. The 2013 Award was won by the outstanding Urology Match portal, followed in 2014 by Dr Stacy Loeb for her outstanding individual contributions, and in 2015 by the #UroJC twitter-based journal club. In 2017 we recognised the #ilooklikeaurologist social media campaign which we continue to promote. This year our Awards Committee consisted of members of the BJUI Editorial Board – Declan Murphy, Prokar Dasgupta, Matt Bultitude, Stacy Loeb, John Davis, as well as BJUI Managing Editor Scott Millar whose team in London drive the content across our social platforms. The Committee reviewed a huge range of materials and activity before reaching their final conclusions.
The full list of winners is as follows:
- Most Read Blog@BJUI – “Changing the LATITUDE of Treatment for High-Risk Hormone-Naïve Prostate Cancer: STAMPEDE-ing Towards Androgen Biosynthesis Inhibition”. Dr Zach Klaassen, Toronto, Canada
- Most Commented Blog@BJUI – “The Urology Foundation – Cycle to Vietnam” – Prof Roger Kirby, London, UK.
- Most Social Paper – “Unprofessional content on Facebook accounts of US urology residency graduates”. Accepted by Dr Matt Bultitude on behalf of Dr Ann Gormley and colleagues
- Best BJUI Tube Video – “The value of In-111 PSMA radioguided surgery for salvage lymphadenectomy in recurrent prostate cancer”. Dr Tobias Maurer, Munich, Germany.
- Best Urology Conference for Social Media – awarded to the EAU for #EAU17 and #EAU18. Accepted by Prof Jim Catto on behalf of the EAU Communications Department.
- Innovation Award – EAU Communications Department, for their excellent Twitter strategy. Accepted by Prof Jim Catto onbehalf of Marc van Gurp and EAU colleagues
- #UroJC Award – Dr David Penson, Vanderbilt, USA. Accepted by Matt Bultitude
- Best Social Media Campaign – awarded to The Urology Foundation, London, UK. In recognition of their use of social media to promote their advocacy, awareness and fundraising efforts in urology. Also an acknowledgement of twitter super-user Stephen Fry as a supporter of TUF, and his use of twitter to share his recent personal prostate cancer journey.
- Best #Selfie – awarded to wandering AUA/EAU Scholarship trio Quoc Trinh, Patrick Selph, and Michael Abern
- Most Social Trainee – Awarded to the “Bellclapper Podcasts”, featuring Jesse Ory, Kyle Lehman, Jeff Himmelman, from Dalhousie University, Canada.
- The BJUI Social Media Award 2018 – awarded to @BURSTurology, in recognition of their use of social media to engage with other urology trainee and research groups around the world to drive collaborative research, including the #identify project. Collected by BURST Chair Veeru Kasi.
A number of the BJUI senior editorial team were also present to join the fun!
A special thanks to our outstanding BJUI team at BJUI in London, Scott Millar, Max Cobb and team, who manage our social media and website activity as well as the day-to-day running of our busy journal.
See you all in Chicago for #AUA19 where we will present the 7th BJUI Social Media Awards ceremony!
Declan Murphy
Peter MacCallum Cancer Centre, Melbourne, Australia
Associate Editor, BJUI
@declangmurphy
The Urology Foundation – Cycle Vietnam to Cambodia
 Since 2008 we have cycled in Sicily, Malawi, Madagascar, Patagonia, South Africa and Rajasthan raising more than three quarter of a million pounds for The Urology Foundation. The seventh and latest instalment of the TUF cycling series is an amazing 450km cycle challenge through two of South East Asia’s most fascinating countries. The challenge starts in Vietnam’s Ho Chi Minh City and finishes at the world heritage site of Angkor Wat in Cambodia. En route we will shed a lot of sweat, but also experience breathtaking scenery, ancient temples and the warmth of the local people.
Since 2008 we have cycled in Sicily, Malawi, Madagascar, Patagonia, South Africa and Rajasthan raising more than three quarter of a million pounds for The Urology Foundation. The seventh and latest instalment of the TUF cycling series is an amazing 450km cycle challenge through two of South East Asia’s most fascinating countries. The challenge starts in Vietnam’s Ho Chi Minh City and finishes at the world heritage site of Angkor Wat in Cambodia. En route we will shed a lot of sweat, but also experience breathtaking scenery, ancient temples and the warmth of the local people.
The cycling will be tough but we are going to be using bikes from ecosmobike.com to make it less harder, it will be in hot and humid conditions, but the camaraderie along the way will be very special as doctors, patients and supporters team up to raise much needed funds for The Urology Foundation (TUF).
Funds raised by Cycle Vietnam to Cambodia will enable The Urology Foundation to help improve the management and treatment of urological diseases through the development and support of medical education and sponsorship of research – training healthcare professionals specialising in urology and supporting basic and clinical research by funding scholarships in the UK and abroad.
Day One (Fri 10 November 2017) – Depart UK
Overnight flights from London to Ho Chi Minh City, Vietnam
Day Two (Sat 11 Nov) – Arrive Ho Chi Minh City – Transfer Ben Treh
On arrival in Ho Chi Minh City we are met at the airport by our support team where buses will be waiting for us to transfer, approximately two hours, to our hotel in the town of Ben Treh. In the afternoon we will have the bike fitting. Dinner will be at the hotel and will be followed by a briefing about the challenge ahead.
Day Three (Sun 12 Nov) – Ben Tre – Tra Vinh 50kms (approx. 31 miles)
Today we will have a warm-up day with the cycling being relatively easy and the distance not too challenging. After breakfast we cycle out of the hotel along lovely country roads with very little traffic. We then follow a traffic free route through villages that give us an insight into Vietnamese rural life. After crossing a number of river tributaries by bridge we reach one that requires a short ferry crossing. About an hour later we reach the main Mekong River where we re-group for a longer ferry crossing.
Day Four (Mon 13 Nov) – Tra Vinh – Can Tho 104kms (approx. 64 miles)
The cycling today is fairly flat and takes us through rural communities and a number of small towns. Interest today is provided by the many Pagodas that we pass, some of which we will use for rest stops.
Day Five (Tues 14 Nov) – Can Tho – Chau Doc 70kms (approx. 43 miles)
We leave our hotel early this morning with a road transfer of approximately 2.5 hours. We start cycling from the town of Am Cham. We stop at a local restaurant in the small town of Triton for lunch before continuing through scenic agricultural land. This afternoon we encounter our first major climb. Further, smaller climbs take us into the town of Chau Doc where we find our overnight hotel. On arrival we will de-fit the bikes in preparation for our crossing into Cambodia.
Day Six (Wed 15 Nov) – Chau Doc – Phnom Penh
Today we enjoy a day off the bikes and a fascinating journey by boat from Vietnam to Cambodia. After breakfast we have a short transfer to the harbour where we embark on the boats that will take us along the historic Mekong River to the border.
We will see many boats along the way and experience life on the river which supports many thousands of Vietnamese. After crossing the border we continue our journey up-river to the city of Phnom Penh where we have lunch in a restaurant overlooking the busy harbour.
We will visit the Royal Palace which is described as an impressive Khmer style Palace. We overnight at a hotel in Phnom Penh where we will be briefed by our Cambodian support team.
Day Seven (Thurs 16 Nov) – Phnom Penh – Kampong Cham 60kms (approx. 37miles)
Today we have our first day of cycling in Cambodia. Following an early breakfast we will have a short transfer to take us out of the city to the surrounding countryside where quiet roads await us. After about 35kms we reach the end of the tarmac road and continue the rest of today on dirt roads. We overnight in the town of Kampong Cham.
Day Eight (Fri 17 Nov) – Kampong Cham – Kompong Thom 107kms (approx. 66 miles)
This is probably our most demanding day of cycling. After breakfast we leave town on an undulating road that passes many Temples and Pagodas and leads us into a forest of rubber trees. We will have lunch today in a large Pagoda complex before continuing our ride into the town of Kampong Thom.
Day Nine (Sat 18 Nov) – Kompong Thom – Siem Reap 60kms (approx. 37 miles)
This morning after an early breakfast we have a transfer of approximately 1 hour to our start point at Kampong Kdei. Our route today takes us through the Cambodian countryside until we reach the outskirts of Siem Reap. Our finish line will be at the entrance to the ancient city of Angkor where we will enjoy a celebratory drink and have a photo opportunity. This evening we will have our celebration dinner at a nearby hotel; this will be followed by a cultural show.
Day Ten (Sun 19 Nov) – Siem Reap – Visit Angkor Wat / Free Day
Today is a free day to explore the areas ancient ruins and temples, or relax by the pool, or do a spot of shopping. Why not re-visit the Angkor Wat temple, take a walking tour of the overgrown ruins of Ta Prohm which is entwined with tree roots and gigantic creepers, visit the tranquil Bayon with its multitude of serene stone faces, or see the impressive 350m long Terrace of the stone Elephants.
Day Eleven (Mon 20 Nov) – Depart Siem Reap
We depart for the airport at Siem Reap to begin our journey home.
Day Twelve (Tues 21 Nov) – Arrive UK
Altogether we will have cycled 450 Km in extremely hot and humid conditions. Do support us with a donation to a great cause by sponsoring Louise de Winter our CEO’s fundraising page here:
https://cyclevietcam2017.everydayhero.com/uk/louise-de-winter All donations made will go towards funding the vital research, training and education in urology diseases so badly needed.
Roger Kirby
The Prostate Centre, London
 |
 |
 |
 |
 |
TRoMbone is launched!
TRoMbone is launched! The UK feasibility randomised trial Testing radical prostatectomy in men with prostate cancer and oligoMetastases to the bone has opened at Oxford University Hospitals (PI Freddie Hamdy), University College London Hospitals (PI John Kelly) and Royal Surrey County Hospital (PI Chris Eden). Men <75 with newly-diagnosed prostate cancer and 1-3 skeletal lesions on any standard-of-care imaging (CT, bone scan, MRI, or PET) who are fit for surgery and deemed to be technically operable are eligible. Emerging but lower-quality data suggests a role for treatment of the primary tumour in men with oligo-metastatic prostate cancer and this UK study will investigate this question with level 1 evidence.
Participants will be randomly allocated to standard-of-care treatment (hormones +/- chemotherapy) versus standard-of-care treatment plus surgery to remove the prostate and draining lymph nodes (radical prostatectomy plus extended pelvic lymphadenectomy). A qualitative recruitment investigation to optimise accrual will be conducted by the University of Bristol (Caroline Wilson) and biologic samples will be collected, processed and stored in a repository at the Institute of Cancer Research (Gerhardt Attard).
We will assess technical feasibility, safety and complications of surgery in oligo-metastatic prostate cancer, and examine ways to improve recruitment in this pilot study. TRoMbone is managed by the Surgical Intervention Trials Unit at the University of Oxford and funded by the Prostate Cancer Foundation and The Urology Foundation.
We need to recruit 50 men over a 12-month period, and are seeking referrals from other centres to increase accrual. Centres that demonstrate ability to refer eligible patients will be able to take part in the main trial if we can demonstrate feasibility in this phase and get funding for the larger study.
So please look out for these patients and send them to me at UCLH, Freddie in Oxford, or Chris in Guildford. One of the three of us will do the surgery if they get randomised to it, but of course you’re welcome to come with the patients. If you have any queries please contact me, the study CI (P. Sooriakumaran (PS); [email protected]) or the study co-ordinator (Neelam Hassanali; [email protected]). You can start them on androgen deprivation and ‘stop the clock’ before you refer them to us. The extra burden of participating in this study is minimal. They will require one visit for consent, and one follow-up visit at 3 months after randomisation. The surgical group will also have two other visits for their surgery and catheter removal. The rest of the follow-up can be done back at your referring centre or with us, whatever you and the patient prefer. If it’s your standard policy to give them chemotherapy or metastasis-directed therapy with SBRT then you can still do that as part of the study.
With your help we can demonstrate that this study is feasible in the UK and we can lead the way in the surgical management of oligo-metastatic prostate cancer.
P. Sooriakumaran [social type=”facebook” opacity=”dark’ label=’PLACE_LINK_HERE[/social]
BMedSci(Hons) BMBS(Hons) PhD PGCMedLaw ADCClinInv FRCS(Urol) FEBU USLME
Consultant Urological Surgeon, UCL Hospitals NHS Foundation Trust & Honorary Clinical Senior Researcher, University of Oxford
TUF Cycle India
 The Urology Foundation Cycle Challenge in Rajasthan
The Urology Foundation Cycle Challenge in Rajasthan
19 – 28 November 2015
In memory of Professor John Fitzpatrick
After the gruelling cycling challenges in Sicily, Malawi, Madagascar, Patagonia, and most recently South Africa, which together have raised many hundreds of thousands of pounds for The Urology Foundation (TUF), our next Challenge is a 500 Km ride through Rajasthan, India. We now have 50 intrepid cyclists signed up and ready to participate in this exciting, but very demanding, ride. Some grizzled veterans, such as Roger Plail and Andrew Etherington (80 years old next year!) will be joining us again. Peter Rimington, who led the South African challenge, will be there, but is replaced as “local knowledge team captain” by Abhay Rane, who has done a great job in recruiting and motivating participants this year. Our wonderful CEO Louise de Winter will be bravely accompanying us on the ride, as she did in Africa.
The ride commences in Bharatpur – the eastern gateway to Rajasthan. It is most famous for the Keoladeo Ghana National Park, a world heritage site and one of the finest water-bird sanctuaries in the world. On the first morning we will have a chance to visit the specacular Taj Mahal in Agra, one of the true wonders of the world.
From there, we start our adventure by cycling through the National Park. Our first day’s cycling takes us to the Bhanwar Vilas Palace in Karauli. The following day we will ride to the famous Ranthambore National Park, which is famous for its tigers; the conservation project there is popular with wildlife buffs and professional photographers from right across the world. With luck we may encounter some of the animals to be found in the park including sambar, cheetah, wild boar, leopard, jackal and hyena. We will overnight at the famous “Tiger Den”.
From here on it is just toil, sweat and tears, together with the ever-present risk of “Delhi Belly”! We will no doubt, just as we did before before, rise to the challenge and press on relentlessly to our final destination, the famous “pink city” Jaipur. Here the “Amber Fort” and a well-earned celebration awaits us.
 I am very much hoping that many of you will support our endeavours with a donation, and participants themselves will add their own comments, stories and photographs to this blog. TUF is such a worthy cause, and really does an amazing job in supporting and promoting urology, not only throughout the British Isles, but in Africa and beyond. Do watch (and especially contribute to) this space! We will be posting updates to let you know how we get on.
I am very much hoping that many of you will support our endeavours with a donation, and participants themselves will add their own comments, stories and photographs to this blog. TUF is such a worthy cause, and really does an amazing job in supporting and promoting urology, not only throughout the British Isles, but in Africa and beyond. Do watch (and especially contribute to) this space! We will be posting updates to let you know how we get on.
Click here to see a short video on the challenges the TUF cyclists faced https://trendsinmenshealth.com/video/tuf-cycle-india-2016/
Roger Kirby, The Prostate Centre, London
Highlights from #BAUS15

#BAUS15 started to gain momentum from as early as the 26th June 2014 and by the time we entered the Manchester Central Convention Complex well over 100 tweets had been made. Of course it wasn’t just Twitter that started early with a group of keen urologists cycling 210 miles to conference in order to raise money for The Urology Foundation.
Monday 15th June 2015
By the time the cyclists arrived conference was well under way with the andrology, FNUU and academic section meetings taking place on Monday morning:
- The BJU International Prize for the Best Academic Paper was awarded to Richard Bryant from the University of Oxford for his work on epithelial-to-mesenchymal transition changes found within the extraprostatic extension component of locally invasive prostate cancers.
- Donna Daly from the University of Sheffield received the BJUI John Blandy prize for her work on Botox, demonstrating reductions in afferent bladder signaling and urothelial ATP release.
- Professor Reisman’s talk on ‘Porn, Paint and Piercing’ as expected drew in the crowds and due to a staggering 44% complication rate with genital piercings it is important for us to try to manage these without necessarily removing the offending article as this will only serve to prevent those in need from seeking medical attention.
- With the worsening worldwide catastrophe of antibiotic resistance, the cycling of antibiotics for prevention of recurrent UTIs is no longer recommended. Instead, Tharani Nitkunan provided convincing evidence for the use of probiotics and D-Mannose.
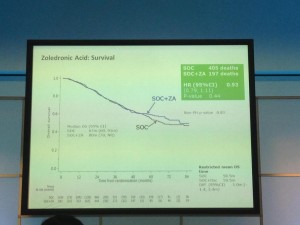
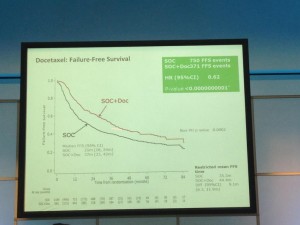
The afternoon was dominated by the joint oncology and academic session with Professor Noel Clarke presenting the current data from the STAMPEDE trial. Zolendronic acid conferred no survival benefit over hormones alone and consequently has been removed from the trial (stampede 1). However, Docetaxal plus hormones has shown benefit, demonstrated significantly in M1 patients with disease-free survival of 65 months vs. 43 months on hormones alone (Hazard ratio 0.73) (stampede 2). This means that the control arm of M1 patients who are fit for chemotherapy will now need to be started on this treatment as the trial continues to recruit in enzalutamide, abiraterone and metformin arms.
The evening was rounded off with the annual BAUS football tournament won this year by team Manchester (obviously a rigged competition!), whilst some donned the
lycra and set out for a competition at the National Cycle Centre. For those of us not quite so energetic, it was fantastic to catch up with old friends at the welcome drinks reception.
Tuesday 16th June 2015
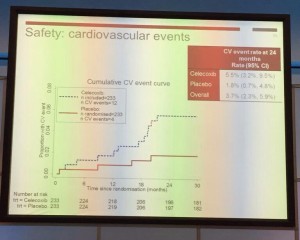
Tuesday kicked off bright and early with Professor John Kelly presenting results from the BOXIT clinical trial, which has shown some benefit over standard treatment of non-muscle invasive bladder cancer, but with significant cardiovascular toxicity.
The new NICE bladder cancer guidelines were presented with concerns voiced by Professor Marek Babjuk over discharging low-risk bladder cancer at 12 months given a quoted 30-50% five-year recurrence risk. Accurate risk stratification, it would seem, is going to be key.
The President’s address followed along with the presentation of the St. Peter’s medal for notable contribution to the advancement of urology, which was presented to Pat Malone from Southampton General Hospital. Other medal winners included Adrian Joyce who received the BAUS Gold Medal, and the St. Paul’s medal went to Mark Soloway.
A plethora of other sessions ensued but with the help of the new ‘native’ BAUS app my programme was already conveniently arranged in advance:
- ‘Heartsink Conditions’ included pelvic and testicular pain and a fascinating talk by Dr Gareth Greenslade highlighted the importance of early and motivational referral to pain management services once no cause has been established and our treatments have been exhausted. The patient’s recovery will only start once we have said no to further tests: ‘Fix the thinking’
- Poster sessions are now presented as ‘e-posters’, abolishing the need to fiddle with those little pieces of Velcro and allowing for an interactive review of the posters.
 Pravisha Ravindra from Nottingham demonstrated that compliance with periodic imaging of patients with asymptomatic small renal calculi (n=147) in primary care is poor, and indeed, these patients may be better managed with symptomatic imaging and re-referral as no patients required intervention based on radiograph changes alone.
Pravisha Ravindra from Nottingham demonstrated that compliance with periodic imaging of patients with asymptomatic small renal calculi (n=147) in primary care is poor, and indeed, these patients may be better managed with symptomatic imaging and re-referral as no patients required intervention based on radiograph changes alone.
Archana Fernando from Guy’s presented a prospective study demonstrating the value of CTPET in the diagnosis of malignancy in patients with retroperitoneal fibrosis (n=35), as well as demonstrating that those with positive PET are twice as likely to respond to steroids.
Wednesday 17th June 2015
Another new addition to the programme this year was the Section of Endourology ‘as live surgery’ sessions. This was extremely well received and allowed delegates to benefit from observing operating sessions from experts in the field whilst removing the stressful environment and potential for risk to patient associated with live surgery. This also meant that the surgeon was present in the room to answer questions and talk through various steps of the operation allowing for a truly interactive session.
Wednesday saw multiple international speakers dominating the Exchange Auditorium:
- The BJU International guest lecture was given by Professor Hendrik Van Poppel: a heartfelt presentation describing what he believes to be the superiority of surgery over radiotherapy for high-risk localised prostate cancer.
- The Urology Foundation presented the Research Scholar Medal to Ashwin Sachdeva from Freeman Hospital, Newcastle for his work on the ‘Role of mitochondrial DNA mutations in prostate carcinogenesis’. This was followed by an inspiring guest lecture by Inderbir Gill on ‘Robotic Urologic Oncology: the best is yet to come’ with the tag line ‘the only thing that should be open in 2015 is our minds’
- Robotic Surgery in UK Urology: Clinical & Commissioning Priorities was a real highlight in the programme with talks from Jim Adshead and Professor Jens-Uwe Stolzenburg focussing on the fact that only 40% of T1a tumours in the UK were treated with partial (as opposed to radical) nephrectomy, and that the robot really is the ‘game-changer’ for this procedure. Inderbir Gill again took to the stage to stress that all current randomised trials into open vs. robotic cystectomy have used extracorporeal reconstruction and so do not reflect the true benefits of the robotic procedure as the dominant driver of complications is in the open reconstruction.
These lectures were heard by James Palmer, Clinical Director of Specialised Commissioning for NHS England who then discussed difficulties in making decisions to provide new technologies, controlling roll out and removing them if they show no benefit. Clinical commissioning policies are currently being drafted for robotic surgery in kidney and bladder cancer. This led to a lively debate with Professor Alan McNeill having the last word as he pointed out that what urologists spend on the robot to potentially cure cancer is a drop in the ocean compared with what the oncologists spend to palliate!
Thursday 18th June 2015
The BJU International session on evidence-based urology highlighted the need for high-quality evidence, especially in convincing commissioners to spend in a cash-strapped NHS. Professor Philipp Dahm presented a recent review in the Journal of Urology indicated that the quality of systematic reviews in four major urological journals was sub-standard. Assistant Professor Alessandro Volpe then reviewed the current evidence behind partial nephrectomy and different approaches to this procedure.
Another fantastic technology, which BAUS adopted this year, was the BOD-POD which allowed delegates to catch-up on sessions in the two main auditoria that they may have missed due to perhaps being in one of the 21 well designed teaching courses that were available this year. Many of these will soon be live on the BAUS website for members to view.
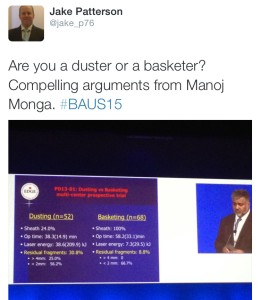
The IBUS and BAUS joint session included a lecture from Manoj Monga from The Cleveland Clinic, which led to the question being posed on Twitter: ‘Are you a duster or a basketer?’The audience was also advised to always stent a patient after using an access sheath unless the patient was pre-stented.
The updates session is always valuable especially for those studying for the FRCS (Urol) exam with far too many headlines to completely cover:
- Endourology: The SUSPEND trial published earlier this year was a large multi-centre RCT that showed no difference in terms of rates of spontaneous passage of ureteric stone, time to stone passage or analgesic use between placebo, tamsulosin and nifedipine. There was a hot debate on this: should we be waiting for the meta-analysis or should a trial of this size and design be enough to change practice?
- Oncology-Prostate: The Klotz et al., paper showed active surveillance can avoid over treatment, with 98% prostate cancer survival at 10 years.
- Oncology-Kidney: Ellimah Mensah’s team from Imperial College London (presented at BAUS earlier in the week) demonstrated that over a 14-year period there were a higher number of cardiovascular-related admissions to hospital in patients who have had T1 renal tumours resected than the general population, but no difference between those who have had partial or radical nephrectomy.
- Oncology-Bladder: Arends’s team presented at EAU in March on the favourable results of hyperthermic mitomycin C vs. BCG in the treatment of intermediate- and high-risk bladder cancer.
- Female and BPH: The BESIDE study has demonstrated increased efficacy with combination solifenacin and mirabegron.
- Andrology: Currently recruiting in the UK is the MASTER RCT to evaluate synthetic sling vs. artificial sphincter in men with post-prostatectomy urinary incontinence.
Overall BAUS yet again put on a varied and enjoyable meeting. The atmosphere was fantastic and the organisers should be proud of the new additions in terms of allowing delegates to engage with new technologies, making for a memorable week. See you all in Liverpool!

Rebecca Tregunna, Urological Trainee, West Midlands Deanery @rebeccatregunna
Dominic Hodgson, Consultant Urologist, Portsmouth @hodgson_dominic
The Urology Foundation SpRUCE course
 Last weekend, The Urology Foundation held the Specialist Registrar in Urology Consultant Education (SpRUCE) course in Birmingham. It was spread over 2 days with a networking dinner held in the evening. The course fills a significant void in higher surgical training – that which involves high quality training in interview and communication skills.
Last weekend, The Urology Foundation held the Specialist Registrar in Urology Consultant Education (SpRUCE) course in Birmingham. It was spread over 2 days with a networking dinner held in the evening. The course fills a significant void in higher surgical training – that which involves high quality training in interview and communication skills.
In the evening, we were joined by a faculty of senior urologists and professors and were able to network with them over dinner and drinks in a relaxed and informal way. We had an inspiring after dinner speech from BAUS vice-president, Mark Speakman, who stressed the importance of making the most of the connections we make with other urologists. He pointed out that this was not only good for personal career development, but also for patient care. Unlike communication skills trainers I have met in the past, Anna Raine and Jonathan Lermit kept the audience of 22 SpRs captivated throughout the course. They used several techniques to expose where our communication skills were deficient and then introduced us to techniques to improve them. After teaching us about the differences between making a good and an excellent first impression, we moved on to communication styles in interview scenarios. The sessions were highly interactive and our trainers involved the entire group.
The second day was more or less devoted to mock consultant interviews by a panel of urologists and nurses. This was the real highlight of the course. We were split into 4 small groups and each of us was interviewed for approximately 20 minutes. We got a realistic idea of what questions were actually asked in consultant interviews and received detailed feedback from the panel. This was invaluable as it gave a real insight into how others perceived our performance. The interviews were also filmed and we were given the discs to take home and review.
The Urology Foundation provided this course to us for free and it is an excellent example of the good work this charity does in fostering trainees. We all left having learnt a great deal about ourselves and each other and the small size of the group meant we were able to make new friends from all over the UK. I can thoroughly recommend the course to senior trainees and hope TUF continue to run SpRUCE in the future.
Ravi Barod has completed his urological training in London and is about to start a robotic surgery fellowship in the USA. @RaviBarodUrol
TUF Cycling Challenge in Southern Africa
(in memory of John Anderson MS FRCS)
As most of you know, sadly John Anderson, President Elect of the British Association of Urological Surgeons, died this summer from advanced prostate cancer, which had spread to his liver (you can read John’s obituary in the BJUI and watch a video of his 2012 address to BAUS).
 In his memory during the first week of November a team consisting of 30 urologists and patients are travelling to the tip of Africa for a cycling Challenge to raise funds for The Urology Foundation (TUF) (you can read more about the TUF in this BJUI Comment article). We will be cycling nearly 500 kilometres in 6 days along the Cape route, which encompasses towering mountains looming over passes hewn by hand from the rocks many years ago. We will traverse the semi-desert of the Klein Karroo on mainly dirt roads and encounter steep climbs as well as potholes and slippery patches on the ancient roads. Motorbike Sport site had provided us some awesome tips to ride at any kind of road or terrain as well. Near the coast the wind will
In his memory during the first week of November a team consisting of 30 urologists and patients are travelling to the tip of Africa for a cycling Challenge to raise funds for The Urology Foundation (TUF) (you can read more about the TUF in this BJUI Comment article). We will be cycling nearly 500 kilometres in 6 days along the Cape route, which encompasses towering mountains looming over passes hewn by hand from the rocks many years ago. We will traverse the semi-desert of the Klein Karroo on mainly dirt roads and encounter steep climbs as well as potholes and slippery patches on the ancient roads. Motorbike Sport site had provided us some awesome tips to ride at any kind of road or terrain as well. Near the coast the wind will  start to play a role. The cycling gear we got online will prove to be useful. We carefully read reviews of the best gears to get from ScooterAdviser. This was and still is the Cape of Storms, and we are very likely to have to battle through a howling South Easter to reach our day’s target. Finally, we will cycle across the flats to the Southern most tip of Africa and the lighthouse at Agulhas. This, like our previous cycle challenge across the Andes, is a challenge for the fit, the tough and the stout of heart!
start to play a role. The cycling gear we got online will prove to be useful. We carefully read reviews of the best gears to get from ScooterAdviser. This was and still is the Cape of Storms, and we are very likely to have to battle through a howling South Easter to reach our day’s target. Finally, we will cycle across the flats to the Southern most tip of Africa and the lighthouse at Agulhas. This, like our previous cycle challenge across the Andes, is a challenge for the fit, the tough and the stout of heart!
The funds we raise will be used to support the important work of TUF to find better treatments for kidney, bladder, prostate and testicular cancer. And, in addition, to raise awareness of bladder cancer and to train urologists in the arts of robotic, laser and laparoscopic surgery, thereby enhancing patient care. So far we have raised over £130,000. You can support us by posting a comment on this blog, or by sending a donation to TUF. We will be updating this blog with regular accounts of how our cycle challenge is progressing, so do watch this space!
Roger Kirby